Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Portuguese Journal of Public Health
Print version ISSN 2504-3137On-line version ISSN 2504-3145
Port J Public Health vol.37 no.2-3 Lisboa 2019
https://doi.org/10.1159/000506015
RESEARCH ARTICLE
Local Health Units in Portugal: The Influence of Chronic Conditions on Inpatient Readmissions
Unidades Locais de Saúde em Portugal: a influência das condições crónicas nas readmissões
Óscar Brito Fernandes a, b, d Sílvia Lopes c, d Ana Patrícia Marques c, d Bruno Moita c, e João Sarmento c Rui Santana c, d
a Department of Health Economics, Corvinus University of Budapest, Budapest, Hungary;
b Department of Public Health, Amsterdam UMC, University of Amsterdam, Amsterdam Public Health Research Institute, Amsterdam, The Netherlands;
c National School of Public Health, NOVA University of Lisbon, Lisbon, Portugal;
d Public Health Research Center, National School of Public Health, NOVA University of Lisbon, Lisbon, Portugal;
e Algarve University Hospital Center, Faro, Portugal
ABSTRACT
Background: In Portugal, a public policy established the Local Health Units (LHUs), merging primary and hospital care providers. LHUs are expected to provide better continuity and coordination of care, thus decreasing the number of unplanned readmissions among those with chronic conditions. This study aims to evaluate the influence of chronic conditions on the risk of readmission at LHUs. - Methods: We used inpatient care administrative databases for the years 2002–2014 ( n = 1,679,634). We assessed the effects of chronic conditions on the risk of readmission with a difference-in-differences technique, comparing LHUs with a control group. Multivariate Cox regression was used to evaluate time to readmission. - Results: The risk of readmission decreased in four LHUs, but significantly only in two. Individuals with more chronic conditions presented a lesser risk of readmission at LHUs, in contrast to those in the control group. - Conclusions: After adjusting for the number of chronic conditions and comorbidities, we concluded that LHUs may successfully decrease unplanned readmissions. Several challenges still have to be addressed to achieve a larger and long-lasting effect. Further investigation is needed to account for contextual and organizational effects that may explain differences across LHUs.
Keywords: Integrated health care Vertical integration Chronic conditions Readmissions Difference in differences Statistical methods
RESUMO
Introdução: Em Portugal, uma política pública estabeleceu as Unidades Locais de Saúde (ULS) que resultam da integração de prestadores de cuidados de saúde primários e hospitalares. É expectável que as ULS prestem melhor continuidade e coordenação de cuidados de saúde e que, consequentemente, consigam reduzir o número de readmissões não planeadas em indivíduos com condições crónicas. O objectivo deste estudo foi avaliar a influência da existência de condições crónicas no risco de readmissão nas ULS. Métodos: Usámos a base de dados de morbilidade hospitalar referente aos anos 2002–2014 (n = 1.679.634). Avaliámos o efeito da existência de condições crónicas no risco de readmissão com a técnica diferença das diferenças, comparando as ULS com um grupo de controlo. Aplicámos uma regressão Cox para avaliar o tempo até ocorrência de readmissão. Resultados: O risco de readmissão diminuiu em 4 ULS; o efeito foi estatisticamente significativo em duas ULS. Indivíduos com maior número de condições crónicas apresentaram menor risco de readmissão nas ULS, em contraste com os indivíduos no grupo de controlo. Conclusões: Tendo em consideração o número de condições crónicas e de comorbidades num indivíduo, as ULS têm potencial para reduzir o número de readmissões não planeadas. Vários desafios devem ser endereçados de modo a serem alcançados resultados mais robustos e de efeito duradouro. Investigações futuras devem considerar possíveis efeitos contextuais e organizacionais que possam explicar a variabilidade de resultados entre ULS.
Palavras Chave: Cuidados de saúde integrados · Integração vertical · Condições crónicas · Readmissões · Diferença das diferenças · Métodos estatísticos
Introduction
More than half of the Portuguese adult population have at least one chronic condition, and one-third live with multiple chronic conditions 1. Individuals with chronic conditions are expected to be high users of varying medical services 2. Thus, these individuals face greater exposure to lack of continuity and coordination of care across the health system 2 ,3 . Partly to address these concerns, some health systems have sought to merge health care providers of different levels of care into a single organization (vertical integration).
Following vertical integration, one expects a decrease in the risk of readmission for individuals with chronic conditions because of better continuity and coordination of care 4 -6 . Reducing readmissions among individuals with chronic conditions is a policy objective for improving health care quality and efficiency. Addressing this problem is a concern to health systems because of the many impacts of aging populations, the increasing prevalence of multiple chronic conditions and the burden of disease. Moreover, readmissions are costly and disruptive of one’s life. However, the evidence on the effects of vertical integration on quality of care indicators is mixed 7 . In Portugal, little evidence has been produced in regard to policies that have sought for better continuity and coordination of care across the health system such as that of the establishment of vertically integrated health care providers.
Since 1999, in the Portuguese National Health Service (NHS), vertical integration is set forth by the Local Health Units (LHUs) 8. Selected public providers were reorganized by the Ministry of Health without a public rationale. LHUs were established between 1999 and 2012; currently, there are eight LHUs in the NHS, which coexist with other public providers. LHUs are accountable for the delivery of care for 12% of the Portuguese mainland population and for 16.9% of the NHS’ budget for hospitals 9. Notwithstanding, little is known about the performance of LHUs on quality of care indicators such as that of the 30-day readmission.
A previous study measured the effect of LHUs on readmissions 10. The findings suggested that following vertical integration, the risk of readmission decreased in LHUs. However, the number of chronic conditions at the individual level was not accounted for. Given that chronic conditions and other comorbidities are the reason for many unplanned readmissions 2 ,11 -13 , our aim was to evaluate the influence of chronic conditions on the risk of readmission in LHUs.
The objective of this study was twofold: (1) to assess the risk of readmission before and after vertical integration, after adjusting for the number of chronic conditions and the Elixhauser comorbidity index and (2) to ascertain associations of individuals’ characteristics (sex, age group, number of chronic conditions and Elixhauser comorbidity index) with time to readmission.
Methods
Study Design
We evaluated the risk of readmission in LHUs before and after vertical integration with a difference-in-differences (DiD) technique. We considered an 8-year time frame for each LHU and compared with that of a control group (5 years before the integration [I–5], the year when the vertical integration occurred [I] and 2 additional years after integration [I+2]). The statistical model included the individuals’ characteristics (individual risk of readmission, number of chronic conditions and Elixhauser comorbidity index) and a set of hospital dummies.
Cox regression was used to understand the association of an individual’s characteristics (sex, age group, number of chronic conditions and Elixhauser comorbidity index) with time to readmission.
Data Sources and Eligibility CriteriaThe Portuguese Central Administration for the Health System (ACSS) provided the administrative databases on inpatient care for the years 2002–2014. Databases included patient-level information registered at public mainland hospitals: unique encoded admission identifier, year, hospital identifier, sex, age, type of admission, discharge date, length of stay, discharge status, principal diagnosis, secondary diagnoses and procedures. The last three were coded with the International Classification of Diseases, 9th revision, Clinical Modification (ICD-9-CM). We considered the first 20 diagnoses of each admission (1 principal diagnosis and 19 secondary diagnoses).
We identified 9,523,432 eligible index admissions, after excluding admissions for the following reasons: data quality (9,111; 0.07%); specialized or low-volume hospital (132,515; 1.1%); deceased, transferred or left against medical advice (1,169,580; 9.4%); without at least 30-day post-discharge follow-up (911,485; 7.4%); and admitted for psychiatric diagnosis, rehabilitation or medical treatment of cancer (645,281; 5.2%). Among eligible index admissions, we selected for analysis those treated at LHUs ( n = 845,275) or at hospitals that composed the control group ( n = 834,359). No missing data were registered on the variables included in the study.
Intervention and Control Group CompositionThe establishment of LHUs occurred in different years: the first in 1999 8, one in February 2007 14, three in September 2008 15, one in November 2009 16, one in June 2011 17 and the last in October 2012 18. These hospitals that transitioned to a vertically integrated model are hereinafter considered as the intervention group (LHU). In contrast to a previous study 10, we increased the sample size by including data of an additional LHU. We excluded from the intervention group the LHU established in 1999 because data were not available for the period before the integration. Hence, we analyzed 7 out of 8 LHUs.
The control group included 6 public hospitals that were not vertically integrated. To compose the control group, we considered ACSS hospital benchmarking groups for financing purposes, created by hierarchical clustering as described elsewhere 19. Control hospitals were similar in dimension and clinical complexity to those of the intervention group. We accounted for possible external systemic effects that could have influenced the evolution of readmissions. Thus, specialty and teaching hospitals, as well as public-private partnerships, were not included as controls.
VariablesThe dependent variable was the occurrence of readmission within a 30-day time frame following an index admission. We identified unplanned readmissions using the Centers for Medicare & Medicaid Services (CMS) hospital-wide all-cause unplanned readmission measure (1: readmitted) 20.
Two complementary measures to assess the level of comorbidity and chronicity were used: Quan’s updated version of the Elixhauser comorbidity index (1: comorbidity present) 21 and the Agency for Healthcare Research and Quality chronic condition indicator (1: chronic condition present) 22. We used ICD-9-CM five-digit codes to compute both measures.
The individual risk of readmission was estimated with generalized linear mixed models at the specialty cohort level as described elsewhere (1: readmitted) 20. To increase the robustness of this estimation we fitted the model considering all eligible index admissions ( n = 9,523,432).
Statistical MethodsWe used absolute and relative frequency to describe admissions to hospitals in the intervention and the control group by sex, age group (0–19, 20–44, 45–64, 65–84, ≥85), number of chronic conditions and Elixhauser comorbidity index (0, 1, 2, 3, 4, ≥5).
A DiD technique via unconditional logit model with fixed effects was used to analyze the effects of vertical integration on the risk of readmission. Given the large sample used, the bias in the unconditional estimator was small 23 and acceptable for the purpose of this research. To relax the parallel trend assumption for the DiD technique, we considered a differential trend model as described elsewhere 24.
The model was as follows:
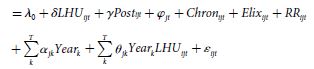
where Y - ijt is a binary variable for episode i in hospital j in year t, assuming value 1 if it is readmission, and 0 otherwise; LHU - ijt is a binary variable taking on value 1 if hospital j in year t is an LHU, and 0 otherwise; Post - ijt is a binary variable taking on value 1 for episode i in hospital j in year t post-integration, and 0 otherwise; φ - jt is a vector of hospital dummies; Chron - ijt is a vector with the number of chronic conditions for individual i admitted to hospital j in year t; Elix - ijt is a vector with the Elixhauser comorbidity index for individual i admitted to hospital j in year t; RR - ijt is a vector with the individual risk of readmission for individual i at hospital j in year t, computed via mixed effects logistic model, as detailed elsewhere 10; Year - k is a set of year dummies; and Year - k LHU - ijt is the interaction between the terms Year and LHU.
Parallel trend assumption was tested using the nonlinear restriction
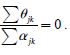
We used Cox regression to study the association of an individual’s characteristics with time to readmission. Hazard function measured the risk of readmission of an individual within a 30-day time frame, adjusting for sex, age group, number of chronic conditions and Elixhauser comorbidity index. We used univariate Cox regression to assess the covariates’ association with time to readmission. Covariates with p < 0.1 were included in the multivariate model. The multivariate model was set up with a stepwise backward likelihood ratio data selection approach. A cutoff of p < 0.05 was considered to remove covariates from the final model. We proceeded with a visual inspection of Kaplan-Meier plots to assess the proportional hazards assumption. The analysis was conducted separately for the intervention and control group.
To compute the individual risk of readmission we used SAS University Edition. All other analyses were performed with Stata (v. 13). The confidence level was set at 95%.
Results
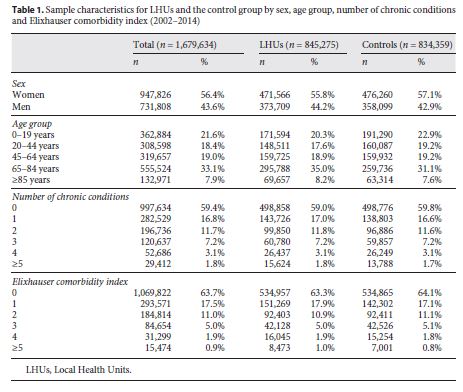
Our study included 1,679,634 index admissions (table 1 ). LHUs accounted for 50.3% of index admissions. The frequency of admissions was greater among women, both in the LHUs and the control group (55.8 and 57.1%, respectively). Individuals admitted to LHUs were older, compared with those in the control group: the average age in LHUs was 51.3 ± 28.4 years and that for the control group 48.5 ± 28.9 years. The distribution of individuals by the number of chronic conditions and comorbidities was similar in both groups.
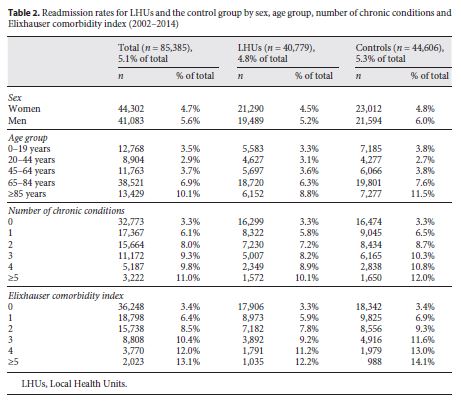
The control group exhibited higher readmission rates (table 2 ). The readmission rate for men was of 5.6%, compared with that of 4.7% for women. Readmission rates increased with age (e.g. the readmission rate for the age group ≥85 years in LHUs was of 8.8%, in contrast to that of 11.5% for the control group). Readmission rates also increased with increasing number of chronic conditions (e.g. the readmission rate for individuals with five or more chronic conditions was 10.1% in LHUs and 12% in the control group). A similar pattern was observed for increasing number of comorbidities.
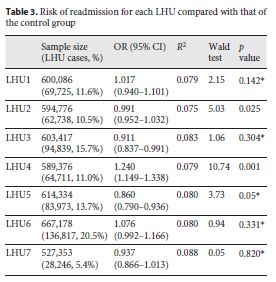
The parallel trend assumption was not observed for LHU2 and LHU4 (table 3 ). Hence, the DiD results for those LHUs were interpreted with caution because the observed effects cannot be solely attributed to vertical integration. LHU1 and control hospitals had a total of 600,086 index admissions, where 11.6% (69,725) were from LHU1. The results suggested a greater risk of readmission for LHU1 compared with that of the control group (odds ratio [OR] 1.017, 95% confidence interval [CI] 0.940–1.101). We observed similar results for LHU4 (OR 1.240, 95% CI 1.149–1.338) and LHU6 (OR 1.076, 95% CI 0.992–1.166). The former showed a statistically significant result, albeit the parallel trend assumption was not verified (Wald test 10.74, p = 0.001). The risk of readmission for LHU2 compared with that of the control group decreased after vertical integration (OR 0.991, 95% CI 0.952–1.032). The results suggested a similar effect for LHU3 (OR 0.911, 95% CI 0.837–0.991), LHU5 (OR 0.860, 95% CI 0.790–0.936) and LHU7 (OR 0.937, 95% CI 0.866–1.013). The results were statistically significant for LHU3 and LHU5.
Both in the intervention and control group, the unadjusted hazard ratio (HR) suggested a decrease in the likelihood of readmission for women (table 4 ). In older age groups, increasing number of chronic conditions and comorbidities were associated with a greater likelihood of readmission. Overall, LHUs presented a lesser risk of readmission for individuals with more chronic conditions and comorbidities, compared with that of the control group.
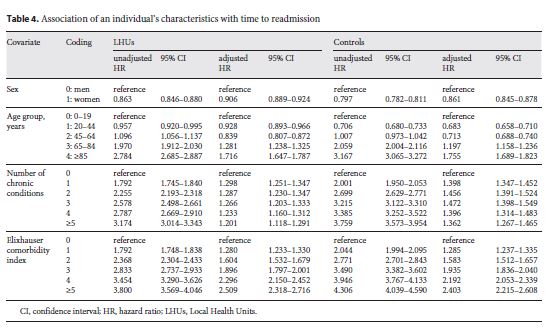
The results of multivariate Cox regression models stressed a similar risk pattern for sex and age in both groups. Women showed a lesser likelihood of readmission in the control group (LHU: HR 0.906, 95% CI 0.889–0.924; control group: HR 0.861, 95% CI 0.845–0.878). The risk of readmission increased across age categories, consistent with the unadjusted HRs (e.g. in LHUs, individuals aged ≥85 years had a 1.7 times greater likelihood of readmission than those aged 0–19 years). The adjusted HR in LHUs decreased with increasing number of chronic conditions, contrasting to the pattern suggested by the unadjusted model. A different pattern was found in the control group, where individuals with three chronic conditions showed a greater likelihood of readmission (HR 1.472, 95% CI 1.398–1.549). Also, an increase in comorbidities was associated with a greater risk of readmission: individuals with five or more comorbidities at LHUs faced a likelihood of readmission 2.5 times greater than those who had no comorbidities.
Discussion
In this study, we assessed the risk of readmission before and after vertical integration, adjusted for an individual’s number of chronic conditions and comorbidities. The association of an individual’s characteristics with time to readmission was analyzed.
Following vertical integration, the risk of readmission did not evolve similarly across LHUs. We found evidence of a positive effect on decreasing the risk of readmission in four LHUs, but with statistical significance for two cases only. Our mixed results on the effect of vertical integration on readmissions are aligned with those suggested by other studies 4 , 5 , 7 , 12 ,25 , 26 . Differences between LHUs may be a result of contextual factors, including that of the implementation process of vertically integrated health care providers in Portugal. The sole responsibility to operationalize the merging of providers was their own, thus yielding different models of care delivery with implications at an operational level. A study developed at LHUs to evaluate the perception of integration among professionals highlighted low levels of perception of clinical integration among physicians and nurses, which increased over time 27. Hence, the ability to provide an interprofessional service delivery that can effectively address the expectations and care needs of those with chronic conditions evolved differently in each LHU. Moreover, LHUs did not receive formal guidance, monitoring or financial incentives by the Ministry of Health to decrease readmissions or to focus on specific needs of those individuals with chronic conditions.
In LHUs, the risk of readmission decreased with increasing number of chronic conditions, which may suggest that LHUs are more responsive to the needs of individuals with multiple chronic conditions. Given that LHUs are responsible for the entire care trajectory, individuals with multiple chronic conditions may be monitored closely, thus delaying or preventing readmissions 28. Also, the interventions that each LHU defined for the period before, during, and after hospital discharge may partly explain this result. These interventions alone have little effect on 30-day readmission rates 29 - 31 , but the effect increases with high-intensity multi-interventions, particularly among individuals with greater risk of readmission 32.
Variability on the risk of readmission signals room for improvement 33. Key barriers to an effective continuum of care are partly configured by: (1) different models of governance and service delivery across vertically integrated providers 34; (2) contextual factors (e.g. geographical distribution of providers and disparities in primary care resources 35); (3) availability of digital health technologies (e.g. real-time data sharing across providers); and (4) the effect of time in fine-tuning a new organizational culture that vertical integration calls on across providers 34.
This research builds on a previous study about the effect of vertical integration on readmissions 10. We extend previous research by illuminating that the risk of readmission varies across LHUs when other patient-level characteristics are considered. Whereas our previous research stressed a positive effect on decreasing the risk of readmission across LHUs 10, in this study a more modest effect was observed. To understand whether these differences were attributed to statistical model specifications, we applied the modeling of our previous research on this new dataset. Computed estimates for the risk of readmission were analogous to those previously reported 36. Hence, we believe that differences between previous estimates of the risk of readmission and our current findings are to a large extent attributed to the inclusion of the number of chronic conditions and the Elixhauser comorbidity index. Given that LHU7 was not included in the previous study, we were not able to compare results.
Our research relies on administrative data and used a retrospective cross-sectional study design, therefore it is limited in its ability to establish causality. Selection bias may have occurred with our choices for the control group, but a randomized control trial design was not feasible for the purpose of this study. We could not account for an extensive list of patient-level factors (e.g. education, income or community support), for these were not available in the Portuguese inpatient databases. Also, organizational-level effects captured by statistical models were limited to two years following vertical integration, when learning effects on vertical integration across LHUs were more intensive. Lastly, the selected model to identify readmissions and to predict an individual’s risk of readmission may be subject to discussion. We chose to use the CMS’ methodological approach for its discriminant power, international widespread use and dense discussion within the research community. Despite these limitations, this study can add new information to the debate on the effects of vertical integration on readmissions, with particular focus on the most vulnerable individuals such as those with multiple chronic conditions.
Conclusion
Our findings suggest mixed results: the risk of readmission decreased in four LHUs, but significantly only in two. Several challenges still have to be addressed to achieve a larger and long-lasting effect on decreasing 30-day hospital readmissions. Hence, it is relevant to develop effective strategies at the hospital level, such as ensuring appropriate discharge planning, effective primary care follow-up after discharge and strengthened communication and collaboration between providers of different levels of care. Additional policies focusing on more vulnerable populations should be considered in combination with fair financial incentives. In addition, making information on risk-adjusted readmission rates publicly available, combined with other performance indicators that matter to citizens, may lead care providers to show greater interest in developing patient-centered strategies.
Finally, the success of the Portuguese vertical integration experience in the NHS cannot be assessed solely by its effects on readmissions. Instead, a wider multidimensional set of performance indicators should be considered, along with an analysis of case studies that further explore the efforts of each LHU to overcome barriers to effective care delivery in vertically integrated organizations.
References
1 Romana GQ, Kislaya I, Salvador MR, Cunha- Gonçalves S, Nunes B, Dias C. Multimorbilidade em Portugal: dados do primeiro inquérito nacional de saúde com exame físico (Multimorbidity in Portugal: results from the first national health examination survey). Acta Med Port. 2019; 32(1): 30–7. [ Links ]
2 Vogeli C, Shields AE, Lee TA, Gibson TB, Marder WD, Weiss KB, et al. Multiple chronic conditions: prevalence, health consequences, and implications for quality, care management, and costs. J Gen Intern Med. 2007 Dec; 22(Suppl 3): 391–5. [ Links ]
3 Balicer RD, Shadmi E, Israeli A. Interventions for reducing readmissions – are we barking up the right tree? Isr J Health Policy Res. 2013 Jan; 2(1): 2. [ Links ]
4 Hesselink G, Schoonhoven L, Barach P, Spijker A, Gademan P, Kalkman C, et al. Improving patient handovers from hospital to primary care: a systematic review. Ann Intern Med. 2012 Sep; 157(6): 417–28. [ Links ]
5 Martínez-González NA, Berchtold P, Ullman K, Busato A, Egger M. Integrated care programmes for adults with chronic conditions: a meta-review. Int J Qual Health Care. 2014 Oct; 26(5): 561–70. [ Links ]
6 Kansagara D, Chiovaro JC, Kagen D, Jencks S, Rhyne K, O'Neil M, et al. Transitions of care from hospital to home: a summary of systematic evidence reviews and recommendations for transitional care in the Veterans Health Administration. Washington, DC: Department of Veterans Affairs; 2015. Available from: https://www.ncbi.nlm.nih.gov/books/NBK311349/pdf/Bookshelf_NBK311349.pdf (cited March 27, 2017). [ Links ]
7 Post B, Buchmueller T, Ryan AM. Vertical integration of hospitals and physicians: economic theory and empirical evidence on spending and quality. Med Care Res Rev. 2018 Aug; 75(4): 399–433. [ Links ]
8 Decreto-Lei 207/99 (Decree-Law 207/99). Diário da República. 1ª Série. nº 133 (1999- 06-09) 3258-64. Available from: https://dre.pt/application/conteudo/310798 (cited March 27, 2017).
9 Portugal. Ministério da Saúde. Administração Central do Sistema de Saúde (ACSS). Termos de referência para a contratualização de cuidados de saúde no SNS para 2019 (2019 reference terms for health care contracting in the NHS). Lisboa: ACSS; 2018. Available from: https://tinyurl.com/y3a78zt6 (cited March 27, 2017).
10 Lopes S, Fernandes OB, Marques AP, Moita B, Sarmento J, Santana R. Can vertical integration reduce hospital readmissions? A difference- in-differences approach. Med Care. 2017 May; 55(5): 506–13. [ Links ]
11 Friedman B, Jiang HJ, Elixhauser A. Costly hospital readmissions and complex chronic illness. Inquiry. 2008–2009; 45(4): 408–21. [ Links ]
12 Schiøtz M, Price M, Frølich A, Søgaard J, Kristensen JK, Krasnik A, et al. Something is amiss in Denmark: a comparison of preventable hospitalisations and readmissions for chronic medical conditions in the Danish Healthcare system and Kaiser Permanente. BMC Health Serv Res. 2011 Dec; 11(1): 347. [ Links ]
13 Ballard J, Rankin W, Roper KL, Weatherford S, Cardarelli R. Effect of ambulatory transitional care management on 30-day readmission rates. Am J Med Qual. 2018 Nov/Dec; 33(6): 583–9. [ Links ]
14 Decreto-Lei 50-B/2007 (Decree-Law 50- B/2007). Diário da República. 1ª Série. nº 42 (2007-02-28) 1414-(29)-(37). Available from: https://dre.pt/application/conteudo/470072 (cited March 27, 2017).
15 Decreto-Lei 183/2008 (Decree-Law 183/ 2008). Diário da República. 1ª Série. nº 171. (2008-09-04) 6225-33. Available from: https://dre.pt/application/conteudo/453991 (cited March 27, 2017).
16 Decreto-Lei 319/2009 (Decree-Law 319/ 2009). Diário da República. 1ª Série. nº 212. (2009-11-02) 8320-9. Available from: https://dre.pt/application/conteudo/483381 (cited March 27, 2017).
17 Decreto-Lei 67/2011 (Decree-Law 67/2011). Diário da República. 1ª Série. nº 107. (2011- 06-02) 3032-41. Available from: https://dre.pt/application/conteudo/673399 (cited March 27, 2017).
18 Decreto-Lei 238/2012 (Decree-Law 238/ 2012). Diário da República. 1ª Série. nº 211. (2012-10-31) 6288-97. Available from: https://dre.pt/application/conteudo/191571 (cited March 27, 2017).
19 Portugal. Ministério da Saúde. Administração Central do Sistema de Saúde (ACSS). Termos de referência para contratualização hospitalar no SNS: contrato-programa 2016 (Reference terms for hospital care contracting in the NHS: contract-program 2016). Lisboa: ACSS; 2016. Available from: https://tinyurl.com/y5nmpy32 (cited March 27, 2017). Local Health Units in Portugal Port J Public Health 2019;37:91–99 99 DOI: 10.1159/000506015
20 Horwitz L, Grady J, Zhang W, Keenan M, Keshawarz A, Dorothy Cohen D, et al. 2015 measure updates and specifications report: hospital- wide all-cause unplanned readmission measure: version 4.0. New Haven, CT: Center for Outcomes Research & Evaluation, Yale New Haven Health Services Corporation; 2015. Available from: https://www.qualitynet.org/inpatient/measures/readmission/resources#tab3 (cited March 27, 2017). [ Links ]
21 Quan H, Sundararajan V, Halfon P, Fong A, Burnand B, Luthi JC, et al. Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med Care. 2005 Nov; 43(11): 1130–9. [ Links ]
22 Agency for Healthcare Research and Quality (AHRQ). Chronic condition indicator (CCI) for ICD-9-CM. Rockville, MD: AHRQ; 2016. Available from: http://tinyurl.com/jg4roeb (cited March 27, 2017). [ Links ]
23 Coupé T. Bias in conditional and unconditional fixed effects logit estimation: a correction. Polit Anal. 2005; 13(3): 292–5. [ Links ]
24 Wagstaff A, Moreno-Serra R. Europe and central Asia's great post-communist social health insurance experiment: aggregate impacts on health sector outcomes. J Health Econ. 2009 Mar; 28(2): 322–40. [ Links ]
25 Plant NA, Kelly PJ, Leeder SR, D'Souza M, Mallitt KA, Usherwood T, et al. Coordinated care versus standard care in hospital admissions of people with chronic illness: a randomised controlled trial. Med J Aust. 2015 Jul; 203(1): 33–8. [ Links ]
26 Balaban RB, Galbraith AA, Burns ME, Vialle- Valentin CE, Larochelle MR, Ross-Degnan D. A patient navigator intervention to reduce hospital readmissions among high-risk safety- net patients: a randomized controlled trial. J Gen Intern Med. 2015 Jul; 30(7): 907–15. [ Links ]
27 Marques A, Barreto X, Lourenço A, Lopes P, Santana R. Medir o processo. In: Santana R, Marques A, editors. A integração vertical de cuidados de saúde. Lisboa: Escola Nacional de Saúde Pública; 2016. p. 153–82. [ Links ]
28 Vanasse A, Courteau M, Ethier JF. The 6W multidimensional model of care trajectories for patients with chronic ambulatory care sensitive conditions and hospital readmissions. Public Health. 2018 Apr; 157: 53–61. [ Links ]
29 Hansen LO, Young RS, Hinami K, Leung A, Williams MV. Interventions to reduce 30-day rehospitalization: a systematic review. Ann Intern Med. 2011 Oct; 155(8): 520–8. [ Links ]
30 Voss R, Gardner R, Baier R, Butterfield K, Lehrman S, Gravenstein S. The care transitions intervention: translating from efficacy to effectiveness. Arch Intern Med. 2011 Jul; 171(14): 1232–7. [ Links ]
31 Verhaegh KJ, MacNeil-Vroomen JL, Eslami S, Geerlings SE, de Rooij SE, Buurman BM. Transitional care interventions prevent hospital readmissions for adults with chronic illnesses. Health Aff (Millwood). 2014 Sep; 33(9): 1531–9. [ Links ]
32 Lee KH, Low LL, Allen J, Barbier S, Ng LB, Ng MJ, et al. Transitional care for the highest risk patients: findings of a randomised control study. Int J Integr Care. 2015 Oct; 15(4):e039. [ Links ]
33 Trudnak T, Kelley D, Zerzan J, Griffith K, Jiang HJ, Fairbrother GL. Medicaid admissions and readmissions: understanding the prevalence, payment, and most common diagnoses. Health Aff (Millwood). 2014 Aug; 33(8): 1337–44. [ Links ]
34 Santana R, Costa C. A integração vertical de cuidados de saúde: aspectos conceptuais e organizacionais (Vertical integration of healthcare: conceptual and organizational aspects). Rev Port Saúde Pública. Temático. 2008; 7: 29–56. [ Links ]
35 Bricard D, Or Z. Impact of early primary care follow-up after discharge on hospital readmissions. Eur J Health Econ. 2019 Jun; 20(4): 611–23. [ Links ]
36 Fernandes OB. Impact of vertical integration on the readmission of individuals with chronic conditions (Master in Health Management dissertation). Lisboa: Escola Nacional de Saúde Pública, Universidade NOVA de Lisboa; 2016. Available from: http://hdl.handle.net/10362/19674 (cited March 27, 2017).














