Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Revista Portuguesa de Medicina Geral e Familiar
Print version ISSN 2182-5173
Rev Port Med Geral Fam vol.36 no.2 Lisboa Apr. 2020
https://doi.org/10.32385/rpmgf.v36i2.12395
ESTUDOS ORIGINAIS
Medication adherence in type 2 diabetes mellitus patients: a cross-sectional study
A adesão à terapêutica medicamentosa nos doentes com diabetes mellitus tipo 2: um estudo observacional transversal
Joana Filipa Ferreira Vieira,1
 https://orcid.org/0000-0003-4740-9658
https://orcid.org/0000-0003-4740-9658
Paulo Santos1-2
1 MEDCIDS, Faculdade de Medicina, Universidade do Porto.
2 CINTESIS, Centro de Investigação em Tecnologias e Serviços de Saúde, Universidade do Porto.
Endereço para correspondência | Dirección para correspondencia | Correspondence
ABSTRACT
Objectives: To evaluate the adherence to medication in patients with type 2 diabetes mellitus and to assess its impact on the disease-oriented outcomes.
Type of study: Cross-sectional.
Location: Porto, Portugal.
Population: Patients with type 2 diabetes mellitus from a primary care setting.
Methods: A convenience sample of patients regularly attending a primary care setting, from July to October 2017, answered anonymously a survey delivered by their family physician. Adherence was assessed by the Treatment Adherence Measure questionnaire. Other evaluated variables were demographic and psychosocial factors and disease-oriented outcomes (weight, height, glycated hemoglobin, and blood pressure).
Results: Eighty-five patients completed the study (54.1% of females) with a mean age of 61.3 years (± 13.8 years). The proportion of patients presenting good adherence to medication was 62.3% (CI95%, 51.8-72.9%). The lowest adherence is more common in patients with depressive symptoms (p=0.004), history of smoking habits (p=0.019), living alone (p=0.009) or living without a marital partner (p=0.039), and it is associated with higher glycated hemoglobin levels (p=0.004).
Conclusions: Poor adherence to medication is a significant problem in the diabetic population, leading to lower glycemic control rates. The identification of its determinants allows us to design a specific intervention in primary care, both in patients’ education and in therapeutic approach, able to improve their health outcomes.
Keywords: Diabetes mellitus, type 2; Adherence; Socioeconomic factors; Depression; Portugal.
RESUMO
Objetivos: Determinar a taxa de adesão à terapia medicamentosa em doentes com diabetes mellitus tipo 2 e avaliar o seu impacto nos parâmetros clínicos.
Tipo de estudo: Observacional, transversal.
Local: Porto, Portugal.
População: Doentes com diabetes mellitus tipo 2 pertencentes a uma Unidade de Saúde Familiar.
Métodos: Uma amostra de conveniência constituída pelos doentes com diabetes mellitus tipo 2 que frequentaram as consultas na Unidade de Saúde Familiar, de julho a outubro de 2017, respondeu anonimamente a um questionário entregue pelo respetivo médico de família. A adesão foi avaliada pelo questionário da Medida de Adesão aos Tratamentos. Outras variáveis testadas consistiram em fatores demográficos e psicossociais e parâmetros clínicos (peso, altura, hemoglobina glicada e pressão arterial).
Resultados: Oitenta e cinco doentes completaram o estudo com idade média de 61,3 ± 13,8 anos (54,1% mulheres). A proporção de doentes que apresentaram boa adesão à medicação foi de 62,3% (IC95%, 51,8-72,9%). A baixa adesão é mais comum em doentes com sintomas depressivos (p=0,004), história de tabagismo (p=0,019), que vivem sozinhos (p=0,009) ou que vivem sem cônjuge (p=0,039) e está associada a níveis aumentados de hemoglobina glicada (p=0,004).
Conclusões: A adesão à medicação é um problema importante na população diabética, levando a um mau controlo glicémico. Identificaram-se vários fatores associados a uma má adesão, permitindo uma intervenção específica nos cuidados primários, tanto na educação como na abordagem terapêutica dos doentes, capaz de melhorar a saúde dos mesmos.
Palavras-chave: Diabetes mellitus tipo 2; Adesão; Fatores socioeconómicos; Depressão; Portugal.
Introduction
Diabetes mellitus (DM) is a common disease. In 2014, the World Health Organization (WHO) estimated that 422 million adults over 18 years old lived with diabetes worldwide.1 Despite the huge investment, official data shows a continuously increasing incidence and a higher burden of disease both for patients and for healthcare systems.
In Portugal, data from the 2015 National Diabetes Observatory Report estimated the prevalence of diabetes of 13.3% among the adult population aged 20-79, representing more than one million patients. The total associated costs were 1,936 million euros (1,893 euros per capita), including direct and indirect costs, about 1% of the Global National Product and 12% of health expenses.2 Given the expected increase in prevalence and population impact, diabetes is considered one of the big-ger challenges in health in the 21st century.3
Patients living with type 2 diabetes mellitus (T2DM) are at increased risk of short and long-term complications, frequently leading to premature death, worsen by the increasing prevalence, the insidious onset, and the belated recognition of the disease.4
The primary goal of diabetic patients is to achieve appropriate glycaemic control.5 Uncontrolled hyperglycemia has been found to increase the incidence of microvascular disease and neuropathy in diabetics.6 It requires active patient involvement to deal with a multifaceted range of self-management skills, including modifying dietary choices, implementing physical exercise regimens, monitoring blood glucose, and the adherence to medical treatments, often complex.4 Treatment with antidiabetic drugs, as well as strict medication adherence, contributes to accomplishing good glycaemic control.4 In clinical practice, this is hard to achieve, and we see that glucose control is frequently suboptimal.7 One of the reasons for this failure is the lack of adherence to the therapeutic regimen.8
Adherence is defined by the extent to which a person’s behavior towards medication or executing lifestyle changes corresponds with agreed recommendations from a healthcare provider.9 Chronic diseases are mostly little symptomatic or even asymptomatic, and patients are more prone to non-adherence. The absence of physical complaints leads to lower motivation for taking correctly the medications. Definitely, this asymptomatic character is one of the constraints to the adherence to medication treatment among people with diabetes, especially in type 2, leading often to the belief that medication is not even necessary.10-11
Non-adherence is associated with poor control of diabetes, with higher levels of glycated hemoglobin (HbA1C). It is also linked to poor control rates in arterial hypertension and dyslipidaemia, leading to an increased risk of hospitalization and mortality. It is also linked to less likelihood of intensifying the treatments when indicated: ‘If the patient doesn’t take these medicines, why to prescribe even more?’12 Non-adherence to medication is still an unsolved problem, with potentially costly and life-threatening sequels. It is crucial to understand patients’ perspectives on diabetes and its medications to promote good adherence, towards efficient and optimum diabetes care.13
Kirkman et al. (2015) studied a large claim database and described several determinants associated with hi-gher adherence in diabetic patients, such as older age, male sex, higher education, higher income, higher daily total pill burden, and lower out-of-pocket costs. Patients who were recently-diagnosed were less likely to be adherent.14 Kivimäki et al. (2013), in Finland, described a decline in adherence to medications after retirement in men with T2DM.15 Higher out-of-pocket costs for antidiabetic medications was also pointed by Piette as a conditioner of non-adherence.16 On its turn, Tunceli, in United Kingdom (2015), found a negative association between younger age and fewer concomitant medications and the adherence to monotherapy in recently diagnosed diabetics.17
Medication adherence is lower when the treatment is perceived as more complex or arduous.18 A systematic review of Claxton et al. (2001) including 76 studies showed that the prescribed number of doses per day was inversely related to medication adherence.19
The prevalence of depression is higher in patients with type 2 diabetes as compared to nondiabetic population, conditioning lower glycemic control, higher risk of complications and poorer self-care behaviors, such as adherence to drug therapy.20-23
Evidence suggests that interventions explicitly tailored to the individual may be the most effective in producing clinically meaningful results,24 but family support and patients’ trust in their physicians have also been recognized as a stimulus for better adherence both to medications and healthy lifestyles, with impact on diabetes’ control.25-26
Few studies have investigated the adherence to medication in Portuguese patients with T2DM. Furthermore, it is important to explore multiple factors acting in the same patient, allowing to understand how different determinants relate to each other. This study aims to characterize the adherence to medication in diabetic patients in a primary care setting, checking for the association between the adherence and the disease-oriented outcomes, and prospecting the potential determinants associated with non-adherence.
Material and methods
Study design, inclusion criteria, and settings
A cross-sectional study was conducted at Unidade de Saúde Familiar Bela Saúde, a primary care setting in Porto, Portugal, from July 2017 to October 2017. Patients aged 18 years old and above, attending this setting and having confirmed diagnosis of T2DM were included.
Exclusion criteria were age below 18 years old, having a mental or physical condition that could interfere with patients’ capacity to understand or answer the questionnaire, and those who were not interested in the study or did not sign the consent form. Analphabet patients could participate if accompanied by someone of their trust to help them answering the questionnaire.
Sample size and sampling
Accepting a margin error of 10%, to a confidence level of 95%, and population size of about 1000 type 2 diabetics, for an unknown response distribution, we calculated the sample size of a minimum of 88 participants to include.27
Patients were invited consecutively as they were present in their scheduled visits. All patients were included if they met the criteria for participation and they accepted to.
Study variables and data collection
Disease-oriented data regarding the patient were collected during the visit by the family physician: weight, height, HbA1c, and systolic and diastolic blood pressure. A questionnaire was distributed to patients to answer after the visit, anonymously and outside the office. The questionnaires were sealed and deposited in a ballot box after. The correspondence between both forms was guaranteed throughout a numbered codification assuring anonymity.
Adherence to medication was assessed using Measure Treatment Adherence (MAT) questionnaire, developed and validated by Delgado and Lima.28 The MAT scale is a variation of the Morisky-Green test, used to assess patients’ behavior patterns associated with the use of medicines. It shows good concurrent validity with high correlations with any answer and a sensitivity and specificity of 0.82 and 0.65, respectively. We used the converted dichotomous scale, according to the following criteria: never (6), and rarely (5), of the Likert scale changed to no (1) in the dichotomous scale; sometimes (3), often (4), almost always (5) and always (6), of the scale of Likert changed to yes (0) in the dichotomous scale.
Variables collected included duration of diabetes, patient’s comorbidities, chronic prescribed medications and number of pills per day.
Stress was assessed through the Perceived Stress Scale - 10 items (PSS-10), of Ribeiro & Marques.29 Depressive symptoms were evaluated using a depression screening questionnaire - Patient Health Questionnaire-2 (PHQ-2).30 Other variables included smoking habits (current smoker, former smoker or never smoker), and smoking history, alcoholic beverages habits, (through AUDIT-c),31 the practice of physical exercise (the type of activity, duration, and frequency), and demographic data (age, gender, employment status, education level, marital status, family structure, socioeconomic status by Grafar classification).
We set < 7% as a reasonable HbA1c cut-off for good control, as this value has been shown to reduce microvascular complications of diabetes.5
Ethical issues
The procedures of this study fulfilled the principles of the Helsinki Declaration on medical research involving human subjects, and the Oviedo Convention. Patients were properly informed about the matters involved in the research, assured of the right to refuse participation, and guarantee that this decision would not affect their treatment. The evaluation instruments were merely observational, without intervention and without entailing a significant physical or psychological risk to the participants. We guaranteed the confidentiality of the answers and their anonymization for computer processing data analysis. The correspondence between the disease-oriented outcomes - collected by the doctors - and the questionnaire given to the patient was assured through a numbered code in the pages. The information was used and treated as a whole, being guaranteed the confidentiality of each participant’s data in the publications and works resulting from this study.
The study protocol was approved by the Ethics Committee for Health of Northern Regional Health Administration.
Statistical analysis
SPSS® v24 of IBM Corporation® was used for data analysis. We calculated frequencies and proportions for descriptive variables (gender, occupation, education level, marital status, household, comorbidities, glycaemic control, medication adherence, exercise habits, depressive symptoms, and alcohol and smoking habits). Mean and the standard deviation was evaluated for quantitative variables (age, duration of diabetes, number of pills, number of medicines, perceived stress, body mass index, HbA1c, and systolic and diastolic pressure). We applied the Mann-Whitney test to study the association of drug adherence with glycaemic control and other factors of metabolic control. A p-value < 0.05 was considered as statistically significant. Logistic binary regression was used to calculate odds ratio (OR) and 95% confidence interval in the other variables.
Results
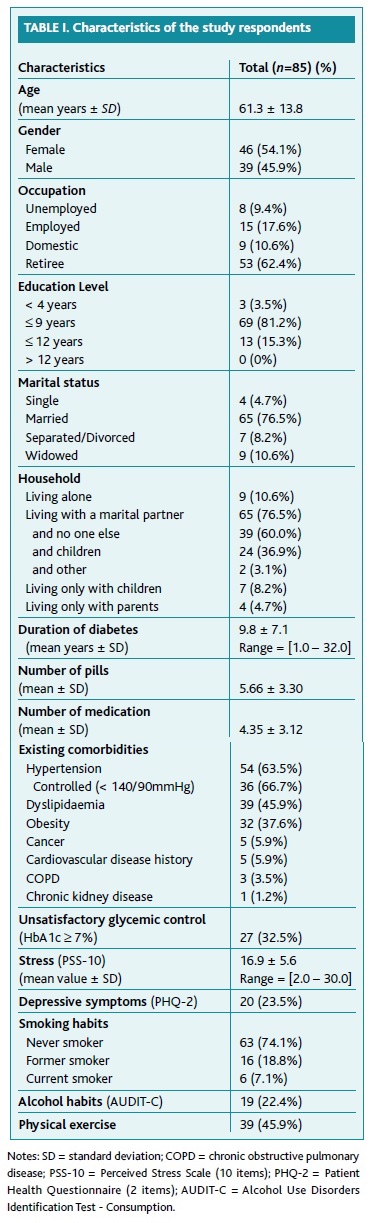
We included 98 patients with T2DM. Thirteen patients were excluded due to non-response or incomplete data, remaining 85 patients for analysis (54.1% of females). Table I shows the description of the sociodemographic and psychological variables of our sample.
The mean age was 61.3 years (± 13.8 years). The majority were married (76.5%), retirees (62.4%), and studied less than nine years at school (84.7%). Only 10.6% of our patients lived alone. The mean duration of diabetes was 9.8 years (± 7.1 years). The average of different medications used by the patient was 4.35 (± 3.12). Arterial hypertension (63.5%), dyslipidemia (45.9%) and obesity (37.6%) were the most common comorbidities. Chronic kidney disease was reported by only one patient (1.2%). Depressive symptoms were found in 23.5% of our patients. Stress scale mean levels were 16.9 ± 5.6, ranging from 2.0 to 30.0. Unsatisfactory glycaemic control (HbA1c > 7%) was found in 32.5% of our patients. The practice of physical exercise more than two times a week was present in 45.9% of our patients. In the lifestyles, we found 7.1% of active smokers and 22.4% with high alcoholic beverages consumption.
The proportion of patients presenting good adherence to medication was 62.3% (95%CI, 51.8-72.9%).
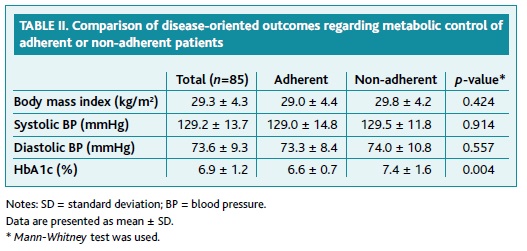
We present a comparison between adherent and non-adherent patients regarding disease-oriented outcomes in Table II. The non-adherence is associated to higher mean HbA1c (7.4 ± 1.6% vs 6.6 ± 0.7%; p=0.004). We did not find any significant differences in the body mass index, systolic blood pressure or diastolic blood pressure.
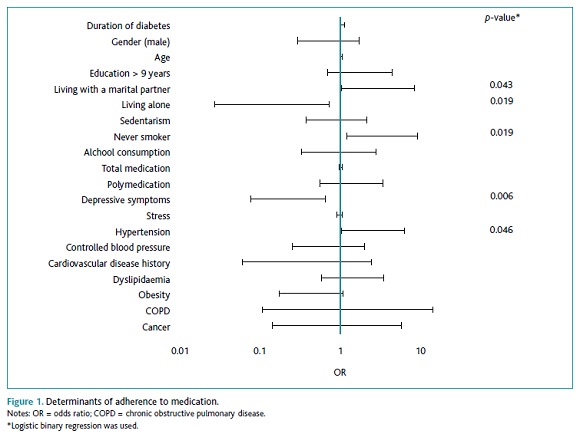
The determinants with influence on adherence to medications are shown in Figure 1. Hypertensive and never smoking patients, as well as patients who lived with their partner, showed statistically significant higher adherence. Depressive symptoms and living alone were associated with lower adherence to the prescribed medication.
Discussion
As far as we know, there is no cure for patients with diabetes mellitus. However, it is possible to live with the disease and to avoid its acute and chronic complications, as long as the access to appropriate medicines is guaranteed and patients take them. In this study, 62.3% of patients presented good adherence to medications, which was associated with a significant and clinically relevant decrease in Hgb A1c levels. In adherent patients, the Hgb A1c average was below 7.0%, meaning good control, as the target set for most patients with diabetes.
The problem of non-adherence is widespread and calls for an integrated approach that addresses patients’ motivation to follow treatment guidelines as well as their ability to do so.32
Several studies estimated the burden of non-adherence. Imtiaz et al., in Multan, Pakistan, described 64% of the diabetic patients as adherent.33 Heissem et al., in Egypt, showed that 73.9% of the participants had good adherence to the oral antidiabetic medications.8 In Uganda, Kalyango found the overall prevalence of adherence among the respondents to be 71.1%.34 Not all the results are concordant. In Brazil, Boas et al. described higher adherence to drug treatment (95.7%),35 and in Pakistan, Shams found only 37.7% of the patients being adherent.36
In Europe, the situation is quite similar. In France (2018), a cross-sectional study including 1,214 diabetic patients revealed that 46.2% were considered strictly adherent to antidiabetic medication. A retrospective chart review of 323 patients with T2DM attending a primary health care center in the eastern part of Bosnia and Herzegovina used a pill count method and evidenced an adherence of 52% to antidiabetic medication. A retrospective cohort study in the United Kingdom showed that 60.1% diabetic patients were adherent to oral antihyperglycemic agents.17 In the USA, Kirkman et al. conducted a retrospective analysis using a large pharmacy claims database including > 200,000 T2DM patients from all 50 states and the larger United States territories, revealing an adherence rate of 69%.14
In Portugal, the full adherence to medical prescriptions is about one-third of the patients’ population undergoing treatment.37 A cross-sectional study conducted by da Costa et al. (2015) in Portugal, recruiting patients via community pharmacies, found 77.2% of adherence to medications in patients with chronic conditions,38 and Dias (2014) described an adherence of 49.6% in patients with ischemic heart disease adhered to the prescribed medication.37 However, we lack a previous study specifically about the adherence in the unique background that is diabetes mellitus.
There are variations in adherence, reflecting an extensive spectrum of results. Worldwide, the rate of adherence to diabetes’ medication varies between 36% and 93%.39 This points the need for studies regarding chronic diseases, to compare the data and determine the contributory factors.
Unsatisfactory glycaemic control (HbA1c ≥ 7%) was observed in 32.5% of the participants. A recent Portuguese study, conducted by Gois et al., has shown suboptimal glycaemic control in 86.6% of diabetics.40 Poor glycaemic control was associated with poor adherence in the current study (p=0.004). Voorham, in Netherlands,41 and Guillausseau, in France,42 concluded the same, demonstrating that low adherence inhibits the intensification of glucose-regulating, and supporting the importance of adherence to medications to achieve the target of HbA1c in diabetics.
Unexpectedly, we found hypertension was positively associated with adherence (p=0.046). This event is not foreseen in the literature. It might result in the fact that patients perceive hypertension as a more severe disease, and so they have a stricter routine concerning medication adherence.
In our study, a statistically significant association was found between depressive symptoms and poor adherence (p=0.004). Other studies have suggested that non-adherence to self-care measures and medications might partially explain unsatisfactory glycaemic control in comorbid depression.43 In a meta-analysis of 47 cohort studies, depression was significantly associated with poor self-care and low adherence to the diabetes treatment regimen.44 A recent cross-sectional study with a sample of 628 outpatients, conducted in Lisbon, Portugal, found a significant association between depressive symptoms and poor glycaemic control in women.40 In this regard, treatment non-adherence may represent an important pathway between depression and worse diabetes disease-oriented outcomes. As far as we know, this is the first report to analyze the relationship between depressive symptoms and adherence in a Portuguese population with T2DM.
The absence of smoking habits was associated with improved adherence (p=0,019). In Hungary, a study undertaken by Hanko et al. concluded that smokers were more likely to neglect to purchase the antidiabetic medicines than non-smokers.45 Other studies focusing on diabetes and smoking habits have shown an enhanced risk for micro and macrovascular disease, as well as premature mortality.46 In a study conducted by Huang et al., current smoking was strongly negatively correlated with the achievement of the HbA1c control.47 Another study in newly diagnosed T2DM patients demonstrated that smoking cessation was associated with improvement of metabolic parameters.48
Smoking cessation did not obtain the attention needed by health care professionals. In our study, only about one-half of the smoking diabetic patients were counseled to quit this habit by their health care providers.46
Concerning demographic factors, our study revealed that patients who live alone have lower adherence to medication (p=0.009). In research undertaken by Silva et al. in Porto, Portugal, the number of people that lived with the patient was modest and positively correlated with insulin treatment adherence; however, there was not a statistically significant correlation between the patient’s household and the adherence to oral antidiabetic treatment.49 One recent systematic review concluded that family support has a positive impact on a healthy diet, higher self-efficacy, improved psychological well-being, and better glycaemic control50 and another pointed family involvement as a facilitator for the disease management.51 On the other hand, reports of family members’ unsupportive behaviors were associated with lower adherence to one’s diabetes medication regimen in several studies.52-53 We also found a higher adherence in the participants who live with a marital partner (p=0.039). These results enhance the importance of family variables, revealing the relevance of including partners on interventions regarding T2DM since they seem to play an important role in patients’ adherence.
Several limitations of this study need to be outpointed. All our patients were recruited from one primary care setting, and thus might not be representative of the general diabetic population in Portugal. The use of self-report data on medication adherence may have a tendency to overestimate adherence, due to recall biases and social desirability. Moreover, the exclusion of anal-phabet patients who were not accompanied by someone of their trust to help them answering the questionnaire may be an important bias. On the other hand, our sample is based on the patients present in a primary care appointment with their doctor. We notice a deviation in general characteristics from those we could expect from the diabetic population of an entire health center, but it does not seem to interfere in the conclusion about the real-world adherence of patients in primary health care.
We were unable to include the contribution of dietary habits, which is an essential part of this disease management. Although PHQ-2 is a commonly used screening tool, patients with probable depression did not take a formal psychiatric examination to validate a diagnosis of major depression. Also, we recommend a larger sample size for future studies. Lastly, due to the cross-sectional nature of our research, we were not able to establish any definite causal relationships.
Non-adherence to medication in patients with T2DM needs to be addressed. In this observational study, the suggested contributory factors for non-adherence are depressive symptoms, history of smoking habits, living alone or living without a marital partner. In diabetic patients with variable glycaemic control, family physicians should be aware that these factors can be associated with a higher risk for T2DM treatment non-adherence and adopt a comprehensive approach. From our results, we endorse the need to screen patients at high risk for poor adherence and to use multiple interventions to improve adherence.
REFERENCES
1. World Health Organization. Global report on diabetes. Geneva: WHO; 2014. [ Links ]
2. Observatório Nacional da Diabetes. Diabetes: factos e números - O ano de 2015. Lisboa: Sociedade Portuguesa de Diabetologia; 2016. [ Links ] ISBN 978-989-96663-2-0
3. International Diabetes Federation. IDF diabetes atlas 2017. 8th ed. Brussels: IDF; 2017. [ Links ] ISBN 978-2-930229-87-4
4. Awodele O, Osuolale JA. Medication adherence in type 2 diabetes patients: study of patients in Alimosho General Hospital, Igando, Lagos, Nigeria. Afr Health Sci. 2015;15(2):513-22. [ Links ]
5. Standards of medical care in diabetes-2016: summary of revisions. Diabetes Care. 2016;39 Suppl 1:S4-5. [ Links ]
6. Sokol MC, McGuigan KA, Verbrugge RR, Epstein RS. Impact of medication adherence on hospitalization risk and healthcare cost. Medical Care. 2005;43(6):521-30. [ Links ]
7. McGovern A, Hinton W, Correa A, Munro N, Whyte M, de Lusignan S. Real-world evidence studies into treatment adherence, thresholds for intervention and disparities in treatment in people with type 2 diabetes in the UK. BMJ Open. 2016;6(11):e012801. [ Links ]
8. Heissam K, Abuamer Z, El-Dahshan N. Patterns and obstacles to oral antidiabetic medications adherence among type 2 diabetics in Ismailia, Egypt: a cross section study. Pan Afr Med J. 2015;20:177. [ Links ]
9. Haynes RB, Taylor DW, Sackett DL. Introduction: the definition of compliance. In: Haynes RB, Taylor DW, Sackett DL, editors. Compliance in health care. Baltimore: Johns Hopkins University Press; 1979. p. 1-6. [ Links ] ISBN 9780801821622
10. Gimenes HT, Zanetti ML, Haas VJ. Factors related to patient adherence to antidiabetic drug therapy. Rev Latin Am Enferm. 2009;17(1):46-51. [ Links ]
11. Rubin RR. Adherence to pharmacologic therapy in patients with type 2 diabetes mellitus. Am J Med. 2005;118 Suppl 5A:27s-34s. [ Links ]
12. Gonzalez JS, Shreck E, Psaros C, Safren SA. Distress and type 2 diabetes-treatment adherence: a mediating role for perceived control. Health Psychol. 2015;34(5):505-13. [ Links ]
13. Islam SM, Biswas T, Bhuiyan FA, Mustafa K, Islam A. Patients’ perspective of disease and medication adherence for type 2 diabetes in an urban area in Bangladesh: a qualitative study. BMC Res Notes. 2017;10(1):131. [ Links ]
14. Kirkman MS, Rowan-Martin MT, Levin R, Fonseca VA, Schmittdiel JA, Herman WH, et al. Determinants of adherence to diabetes medications: findings from a large pharmacy claims database. Diabetes Care. 2015;38(4):604-9. [ Links ]
15. Kivimaki M, Batty GD, Hamer M, Nabi H, Korhonen M, Huupponen R, et al. Influence of retirement on nonadherence to medication for hypertension and diabetes. CMAJ. 2013;185(17):E784-90. [ Links ]
16. Piette JD, Heisler M, Wagner TH. Problems paying out-of-pocket medication costs among older adults with diabetes. Diabetes Care. 2004;27(2):384-91. [ Links ]
17. Tunceli K, Iglay K, Zhao C, Brodovicz KG, Radican L. Factors associated with adherence to oral antihyperglycemic monotherapy in patients with type 2 diabetes mellitus in the United Kingdom. Diabetes Res Clin Pract. 2015;109(3):e27-31. [ Links ]
18. Garcia-Perez LE, Alvarez M, Dilla T, Gil-Guillen V, Orozco-Beltran D. Adherence to therapies in patients with type 2 diabetes. Diabetes Ther. 2013;4(2):175-94. [ Links ]
19. Claxton AJ, Cramer J, Pierce C. A systematic review of the associations between dose regimens and medication compliance. Clin Ther. 2001;23(8):1296-310. [ Links ]
20. Anderson RJ, Freedland KE, Clouse RE, Lustman PJ. The prevalence of comorbid depression in adults with diabetes: a meta-analysis. Diabetes Care. 2001;24(6):1069-78. [ Links ]
21. Lin EH, Rutter CM, Katon W, Heckbert SR, Ciechanowski P, Oliver MM, et al. Depression and advanced complications of diabetes: a prospective cohort study. Diabetes Care. 2010;33(2):264-9. [ Links ]
22. Lustman PJ, Anderson RJ, Freedland KE, de Groot M, Carney RM, Clouse RE. Depression and poor glycemic control: a meta-analytic review of the literature. Diabetes Care. 2000;23(7):934-42. [ Links ]
23. Gonzalez JS, Safren SA, Delahanty LM, Cagliero E, Wexler DJ, Meigs JB, et al. Symptoms of depression prospectively predict poorer self-care in patients with type 2 diabetes. Diab Med. 2008;25(9):1102-7. [ Links ]
24. de Vries McClintock HF, Morales KH, Small DS, Bogner HR. A brief adherence intervention that improved glycemic control: mediation by patterns of adherence. J Behav Med. 2015;38(1):39-47. [ Links ]
25. Santos AL, Marcon SS. How people with diabetes evaluate participation of their family in their health care. Invest Educ Enferm. 2014;32(2):260-9. [ Links ]
26. Ratanawongsa N, Karter AJ, Parker MM, Lyles CR, Heisler M, Moffet HH, et al. Communication and medication refill adherence: the Diabetes Study of Northern California. JAMA Intern Med. 2013;173(3):210-8. [ Links ]
27. Hulley SB, Cummings SR, Browner WS, Grady DG, Newman TB. Designing clinical research. 3rd revised ed. Lippincott Williams and Wilkins; 2007. ISBN 9780781782104
28. Delgado AB, Lima ML. Contributo para a validação concorrente de uma medida de adesão aos tratamentos [Contribution to concurrent validity of treatment adherence]. Psicol Saúde Doenc. 2001;2(2):81-100. Portuguese
29. Pais-Ribeiro JL, Marques T. A avaliação do stresse: a propósito de um estudo de adaptação da escala de percepção de stresse [Stress assessment: a propos of the adaptation study of the perceived stress scale]. Psicol Saúde Doenc. 2009;10(2):237-48. Portuguese
30. Kroenke K, Spitzer RL, Williams JB. The Patient Health Questionnaire-2: validity of a two-item depression screener. Medical Care. 2003;41(11):1284-92. [ Links ]
31. Bush K, Kivlahan DR, McDonell MB, Fihn SD, Bradley KA. The AUDIT alcohol consumption questions (AUDIT-C): an effective brief screening test for problem drinking. Ambulatory Care Quality Improvement Project (ACQUIP). Alcohol Use Disorders Identification Test. Arch Intern Med. 1998;158(16):1789-95. [ Links ]
32. Habib SS, Aslam M. Risk factors, knowledge and health status in diabetic patients. Saudi Med J. 2003;24(11):1219-24. [ Links ]
33. Imtiaz S, Ullah H, Rasool MF, Hashmat F, Saleem M, Khan N. Assessment of compliance of diabetic patients at Nishtar Hospital Multan, Pakistan. Gomal J Med Sci. 2014;12(2):84-8. [ Links ]
34. Kalyango JN, Owino E, Nambuya AP. Non-adherence to diabetes treatment at Mulago Hospital in Uganda: prevalence and associated factors. Afr Health Sci. 2008;8(2):67-73. [ Links ]
35. Villas-Boas LC, Foss-Freitas MC, Pace AE. Assessment of compliance of diabetic patients at Nishtar Hospital Multan, Pakistan [Adherence of people with type 2 diabetes mellitus to drug treatment]. Revista Bras Enferm. 2014;67(2):268-73. Portuguese
36. Shams N, Amjad S, Kumar N, Ahmed W, Saleem F. Drug non-adherence in type 2 diabetes mellitus: predictors and associations. J Ayub Med Coll Abbottabad. 2016;28(2):302-7. [ Links ]
37. Dias A, Pereira C, Monteiro MJ, Santos C. Patients’ beliefs about medicines and adherence to medication in ischemic heart disease. Aten Primaria. 2014;46 Suppl 5:101-6. [ Links ]
38. da Costa FA, Pedro AR, Teixeira I, Braganca F, da Silva JA, Cabrita J. Primary non-adherence in Portugal: findings and implications. Int J Clin Pharm. 2015;37(4):626-35. [ Links ]
39. Wabe NT, Angamo MT, Hussein S. Medication adherence in diabetes mellitus and self management practices among type-2 diabetics in Ethiopia. N Am J Med Sci. 2011;3(9):418-23. [ Links ]
40. Gois C, Duarte TA, Paulino S, Raposo JF, do Carmo I, Barbosa A. Depressive symptoms are associated with poor glycemic control among women with type 2 diabetes mellitus. BMC Res Notes. 2018;11(1):38. [ Links ]
41. Voorham J, Haaijer-Ruskamp FM, Wolffenbuttel BH, Stolk RP, Denig P. Medication adherence affects treatment modifications in patients with type 2 diabetes. Clin Ther. 2011;33(1):121-34. [ Links ]
42. Guillausseau PJ. Influence of oral antidiabetic drugs compliance on metabolic control in type 2 diabetes: a survey in general practice. Diabetes Metab. 2003;29(1):79-81. [ Links ]
43. Katon W, Russo J, Lin EHB, Heckbert SR, Karter AJ, Williams LH, et al. Diabetes and poor disease control: is comorbid depression associated with poor medication adherence or lack of treatment intensification? Psychosom Med. 2009;71(9):965-72. [ Links ]
44. Gonzalez JS, Peyrot M, McCarl LA, Collins EM, Serpa L, Mimiaga MJ, et al. Depression and diabetes treatment nonadherence: a meta-analysis. Diabetes Care. 2008;31(12):2398-403. [ Links ]
45. Hanko B, Kazmer M, Kumli P, Hragyel Z, Samu A, Vincze Z, et al. Self-reported medication and lifestyle adherence in Hungarian patients with type 2 diabetes. Pharm World Sci. 2007;29(2):58-66. [ Links ]
46. Haire-Joshu D, Glasgow RE, Tibbs TL. Smoking and diabetes. Diabetes Care. 1999;22(11):1887-98. [ Links ]
47. Huang Y, Li J, Zhu X, Sun J, Ji L, Hu D, et al. Relationship between healthy lifestyle behaviors and cardiovascular risk factors in Chinese patients with type 2 diabetes mellitus: a subanalysis of the CCMR-3B STUDY. Acta Diabetol. 2017;54(6):569-79. [ Links ]
48. Voulgari C, Katsilambros N, Tentolouris N. Smoking cessation predicts amelioration of microalbuminuria in newly diagnosed type 2 diabetes mellitus: a 1-year prospective study. Metabolism. 2011;60(10):1456-64. [ Links ]
49. Silva I, Pais-Ribeiro JL, Cardoso H. Adesão ao tratamento da diabetes mellitus: a importância das características demográficas e clínicas [Diabetes mellitus treatment adherence: The relevance of demographic and clinical characteristics]. Rev Referência. 2006;2(2):33-41. Portuguese
50. Pamungkas RA, Chamroonsawasdi K, Vatanasomboon P. A systematic review: family support integrated with diabetes self-management among uncontrolled type II diabetes mellitus patients. Behav Sci. 2017;7(3)62. [ Links ]
51. Sohal T, Sohal P, King-Shier KM, Khan NA. Barriers and facilitators for type-2 diabetes management in South Asians: a systematic review. PloS One. 2015;10(9):e0136202. [ Links ]
52. Mayberry LS, Osborn CY. Family support, medication adherence, and glycemic control among adults with type 2 diabetes. Diabetes Care. 2012;35(6):1239-45. [ Links ]
53. Mayberry LS, Osborn CY. Family involvement is helpful and harmful to patients’ self-care and glycemic control. Patient Educ Counsel. 2014;97(3):418-25. [ Links ]
Endereço para correspondência | Dirección para correspondencia | Correspondence
Joana Filipa Ferreira Viana
E-mail: joanavieira_12@hotmail.com
Acknowledgments
We thank the family physicians of Unidade de Saúde Familiar Bela Saúde for embracing the project and being involved in data collection.
Conflicts of interest
The authors have no conflicts of interest to declare.
Funding
The authors declare that the study did not receive any type of funding.
Recebido em 26-04-2018
Aceite para publicação em 03-12-2019