Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Angiologia e Cirurgia Vascular
versão impressa ISSN 1646-706X
Angiol Cir Vasc vol.14 no.4 Lisboa dez. 2018
ARTIGO DE REVISÃO
Acute carotid stent thrombosis - A rare clinical entity?
Trombose aguda de stent carotídeo - Uma entidade clínica rara?
Andreia Coelho1,2, Miguel Lobo1, Clara Nogueira1,2, Jacinta Campos1,2, Rita Augusto1,2, Nuno Coelho1,2, Ana Carolina Semião1, João Pedro Ribeiro1, Alexandra Canedo1,2
1Serviço de Angiologia e Cirurgia Vascular, Centro Hospitalar de Vila Nova de Gaia e Espinho
2Faculdade de Medicina da Universidade do Porto
Endereço para correspondência | Dirección para correspondencia | Correspondence
ABSTRACT
Introduction: Acute carotid stent thrombosis (ACST), defined according to the Academic Research Consortium as occurring in the first 24 hours after the procedure, is described as an exceedingly rare complication of CAS but it can lead to catastrophic neurologic consequences. The European Society for Vascular Surgery updated guidelines state that thrombolysis and intravenous abciximab may be effective, but provide no specific recommendations.
Given the lack of data concerning the optimal management, the purpose of this review was to evaluate the current literature and report on ACST aetiology and management strategies.
Methods: Literature review was performed in the MEDLINE database.
Results: No data on ACST is evident in large randomized controlled trials. ACST incidence rate ranges from 0.5-0.8%, reaching as high as 33% in acute-setting.
Considering aetiology, it can be subdivided into 2 main groups: systemic causes and technical complications. In the first antiplatelet non-compliance/resistance were the most reported while in the latter carotid artery dissection and plaque protrusion were the most common causes. Dual layer stents have been associated with greater risk for ACST in the literature.
There are three main approaches for ACST: pharmacologic, endovascular and surgical. Pharmacologic management included anticoagulation, thrombolysis and facilitated thrombolysis. A role for thrombolysis and facilitated thrombolysis is still to be determined. Endovascular treatment was the most common approach to intraprocedural ACST: mechanical thrombectomy and thrombus aspiration with or without simultaneous facilitated thrombolysis. Surgical options included carotid endarterectomy with stent explantation which was a bail-out after failed endovascular treatment with excellent recanalization rates. In asymptomatic ACST conservative management with anticoagulation was unanimous.
Discussion: As a conclusion, ACST is probably an underestimated clinical entity associated with multiple risk factors. Decision on the best approach depends if ACST occurs intraprocedural or afterwards, on the development of neurologic status deterioration and on centre's experience. Additional studies must be undertaken to better define optimal management.
Keywords: Carotid stenosis [MeSH Terms], Carotid Artery Diseases [MeSH Terms], Stents [MeSH Terms], Carotid Artery Thrombosis [MeSH Terms]
RESUMO
Introdução: A trombose aguda de stent carotídeo (ACST), que se define de acordo com o Academic Research Consortium como o evento que ocorre nas primeiras 24 horas após o procedimento, é descrita como uma complicação rara de stenting carotídeo mas tem consequências potencialmente catastróficas. A European Society for Vascular Surgery atualizou as suas guidelines concluindo que trombólise e o abciximab poderão ser eficazes, mas não fornece recomendações terapêuticas específicas.
O objetivo deste artigo foi sumariar a evidência existente relativa à etiologia e abordagem de ACST.
Métodos: Uma revisão de literatura foi realizada usando a base de dados MEDLINE.
Resultados: Não são reportados dados relativos à taxa de incidência de ACST nos grandes ensaios clínicos randomizados publicados. Em cohorts publicados, a taxa de incidência varia entre 0,5 a 0,8% na maioria dos estudos, mas pode atingir os 33% em contexto agudo pós-acidente vascular cerebral (AVC).
Considerando a etiologia, podemos subdividir em 2 categorias principais: causas sistémicas e complicações técnicas. No primeiro caso, a não adesão / resistência aos antiagregantes plaquetários foram as causas mais reportadas, enquanto que nas complicações técnicas inclui-se a dissecção da artéria carótida e a protrusão da placa. De salientar também que dual layer stents foram associados a maior risco de ACST.
Existem três abordagens principais para o ACST: farmacológica, endovascular e cirúrgica. A abordagem farmacológica inclui a hipocoagulação, a trombólise e a trombólise facilitada, apesar de o papel das duas últimas continuar por esclarecer.
O tratamento endovascular foi a abordagem mais comum para ACST intraprocedimento: trombectomia mecânica com ou sem trombólise facilitada concomitante. As opções cirúrgicas incluíram endarterectomia carotídea com explantação do stent, que foi também o bail-out após mau resultado com tratamento endovascular, atingindo excelentes taxas de recanalização. Nos casos de ACST assintomáticos, o tratamento conservador com hipocoagulação foi unânime.
Discussão: Como conclusão, o ACST é provavelmente uma entidade clínica subestimada associada a múltiplos fatores de risco. A decisão relativa à melhor abordagem deve depender se o ACST ocorre intraprocedimento ou não, da constatação ou não de deterioração do estado neurológico e da experiência do centro. Estudos adicionais devem ser realizados para melhor definir a abordagem ideal.
Palavras-chave: Estenose carotídea; Doença Carotídea; Stents; Trombose da artéria carótida;
Introduction
Stroke remains nowadays the leading cause of death and permanent disability in Portugal. Data from DGS (Direção Geral de Saúde) estimates an incidence of 2 cases/1000habitants/year, with 30% mortality within the first year and 40% of permanent disability in first year survivors.(1)
Carotid bifurcation atherosclerotic disease is one of the most common correctable culprits.(2) Management options for carotid atherosclerotic disease depend on whether carotid disease is symptomatic or asymptomatic and on patients surgical risk. Options include best medical treatment (BMT) alone or associated with carotid artery revascularization with open carotid endarterectomy (CEA) and carotid artery stenting (CAS). Traditionally, CEA has been the gold standard for management of both symptomatic and asymptomatic high-grade carotid artery stenosis, and original indications for CAS were limited to anatomically and physiologically high-risk patients.(2) However, the minimally invasive nature, shorter procedure and patient-recovery times, and expanded pool of physicians capable of performing the procedure, have popularized CAS beyond its original indications.(3)
Nowadays, according to the 2017 update to European Society for Vascular Surgery (ESVS) Carotid and Vertebral Artery Disease Guidelines, CAS and BMT may be considered in symptomatic or asymptomatic carotid artery disease (Class IIb Level of evidence B).(2)
Acute carotid stent thrombosis (ACST), defined according to the Academic Research Consortium as occurring in the first 24 hours after the procedure(4), is described as an exceedingly rare complication of CAS even though it can lead to catastrophic neurologic consequences.(5) However, this may be grossly underestimated as randomized controlled trials (RCTs) published on CAS are omissive regarding this complication. A follow-up study on ACST using serial Computed Tomography Angiography (CTA) revealed that the occurrence rate of acute or subacute in-stent thrombosis among 23 cases of CAS reached 43.5%. The eccentric hypodense area in the stent lumen was thrombotic material, most of which resolved within 12 weeks owing to endogenous thrombolysis.(6)
Management of ACST and the outcome after successful rescue of carotid thrombosis remain currently unclear.(7)
Given the lack of data concerning the optimal management, the purpose of this review was to evaluate the current literature and report on ACST aetiology and management strategies.
Methods
Literature review was performed in the MEDLINE database with the following query: (acute carotid stent thrombosis) OR (carotid artery stenting AND acute thrombosis) OR (acute carotid stent occlusion) in order to identify manuscripts on the subject.
Additionally, relevant randomized controlled trials published on CAS were reviewed in order to identify reports on ACST incidence.
Results
Data from CAS RCTs
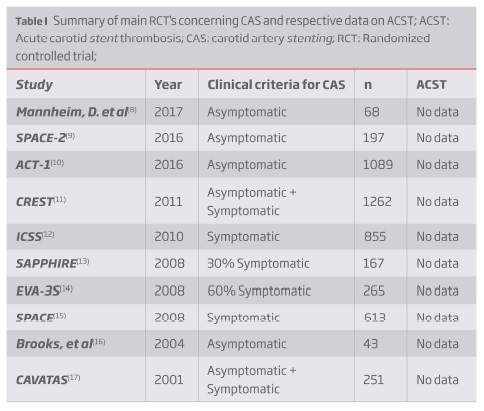
Data from Table 1 summarizes the main RCT's published concerning CAS safety comparing it with carotid endarterectomy (CEA). All RCT report on complications such as stroke and myocardial infarction as primary endpoints, but none report on ACST.
ACST Incidence Rate
ACST incidence rate is very difficult to establish as the main RCT's on CAS do not report this complication (Table 1). Data on ACST incidence rate come from observational studies only, with a reported incidence of 0.5-0.8% in most studies.(7, 18-21) The biggest reported series includes 674 patients, with an ACST incidence rate of 0.59%.(19)
There are however reports of incidence rates reaching as high as 33%, when CAS is performed in acute phase post-stroke.(22-24)
Aetiology
Aetiology for ACST is usually subdivided in 2 main groups: Local/technical causes and systemic causes. In the latter group, antiplatelet non-compliance is systematically identified as the most important potentially preventable cause for ACST.(2) Other causes include antiplatelet resistance and hypercoagulable states (such as thrombocythemia, diabetes mellitus and heparin resistance) and antiplatelet resistance.(21)
Standard antiplatelet therapy recommendation is dual antiplatelet therapy with aspirin and clopidogrel preoperatively that should be continued for at least one month, followed by clopidogrel thereafter. In acute setting, loading doses of both clopidogrel and aspirin as well as intravenous continuous administration of a third antiaggregant (GPIIb/IIIa inhibitor) are usually administered. Most operators administer 5000 IU of intravenous heparin prior to the procedure.(2)
Aspirin resistance has been defined clinically as the development of thrombotic and vascular events although therapeutic doses of aspirin are given. On the other hand, clopidogrel resistance has been defined as the continued activity of the target of clopidogrel (platelet P2Y12 receptors) despite the adequate antiplatelet therapy.(25) Fifi et al reported aspirin resistance prevalence of 5.2% and clopidogrel resistance of 36.5% among 96 patients who underwent neurovascular stenting.(26) Recent data however, recommend against routine testing for clopidogrel and ASA resistance as randomized trials have failed do demonstrate any benefit of platelet function monitoring to adjust therapy.(27)
Technical causes include vessel dissection, severe plaque protrusion, early stent restenosis and stent underexpansion. Furthermore, deployment of the stent and balloon angioplasty ruptures the luminal plaque, exposing thrombogenic material, thereby potentially promoting thrombosis both locally within the stent and remotely at the distal protection device. Descriptions in the literature of sequential occlusion of distal protection device and carotid stent exist.(28)
Also concerning technical complications, type of carotid stent deserves special consideration. ICSS RCT reported significantly lower 30-day risks of death/stroke in CAS patients where closed cell designed stents were used (5.1%), versus 9.5% in patients where open cell designed stents were used (OR 10.53, 95% CI 0.31-0.91, p .024).(12) The rationale for this difference is the greater risk for plaque protrusion during CAS with open cell stents in unstable plaques. Plaque protrusion is strongly associated with ischemic complications.(29) Open cell stents have also been associated with greater incidence of post-procedural complications.(30)
Regarding micromesh or dual layer stents, there is currently no evidence that they reduce procedural risks after CAS.(2) The rationale for this stent is the increased flexibility and conformability and improved device navigation when compared to closed-cell stents. Open cell stent platform enables device to conform to difficult anatomies, while closed cell lattice can trap atherosclerotic/thrombotic material and prevent protrusion. However, regarding the risk for ACST associated with dual layer stents, in a single report in the setting of emergency CAS with intra-cranial thrombectomy, the dual-layer Casper RX, Microvention, Tustin, CA was reported to have a significantly higher rate of acute occlusion with an odds ratio of 21.3 (45% Vs 3.7%; p=0.0001).(24)
Diagnosis
Post-CAS surveillance is extremely variable between studies, which may explain in part the differences in ACST incidence between studies, as asymptomatic ACST may be missed. In patients with multiple risk factors for ACST, examination with ultrasound Doppler at least twice in the first week after CAS has been recommended.(31)
Management
Decision on the best approach should depend on 3 main factors: whether ACST occurs intra-procedural or afterwards, on the presence or absence of neurologic status deterioration and finally on the centre's and surgeon's experience.
Management options can be subdivided into 3 main categories: farmacologic, endovascular and surgical treatment.
Pharmacologic treatment includes anticoagulation, GP IIb/IIIa Inhibitors, thrombolysis and facilitated thrombolysis. Anticoagulation may be used alone or as an adjuvant, but in asymptomatic cases, conservative management with anticoagulation alone was an unanimous option in studies.(18)
GP IIb/IIIa inhibitor abciximab administered both intravenously (iv) or catheter directed intra-arterially, has been reported to recanalize acutely occluded stents.(32) Thrombolysis has been referenced in ESVS guidelines as worth of consideration in ACST(2) The combined therapeutic regimen consisting of dethrombosis (GP IIb/IIIa inhibitors) and fibrinolysis (as alteplase) - termed “facilitated thrombolysis” can improve recanalization rates even further. Steiner-Böker et al described facilitated thrombolysis as a rescue therapy for in-stent thrombosis. In their case report they used locally administered intra-arterial tPA plus abicixmab and additional heparin with restoration of blood flow occurring within 15 min. They argued that this method could provide a more rapid means to restore blood flow, thereby minimizing potential adverse neurologic sequelae.(33)
The literature remains sparse on effective and reliable endovascular treatment strategies should medical therapy fail. Thrombectomy with devices such as the Penumbra System (PS; Penumbra, Alameda, Calif) was first used for recanalization of acute intracranial large arterial vessels, however it has a potential to resolve ACST during CAS. Nevertheless if ACST is caused by severe plaque protrusion caution is warranted.(34)
Dhall et al described successful simultaneous direct thrombosuction with the guiding sheath with facilitated thrombolysis for intraprocedural ACST.(35)
Setacci et al described 2 cases of successful thrombectomy by careful aspiration. The entire clot was pulled out by using forceps and an aspirator, and an excellent runoff was achieved without the need to remove the stent.(21)
In-stent PTA performed under distal protection without additional placement of stent was described in one case successfully.(7) Stent-in-stent has been described more often with encouraging results.(36)
The management of ACST may require emergent definite surgical repair, particularly when neurologic status deterioration ensues or as a bailout after failed endovascular revascularization attempt. Stent removal and CEA is effective in rapid reestablishment of cerebral perfusion and neurologic status improvement, but there are concerns with the time-consuming aspect of this procedure. Also emergent CEA in an acute post-ACST setting is associated with higher morbidity associated with dual-antiplatelet therapy and anticoagulation and greater risk for cranial nerve damage.(37)
Discussion
There is an astonishing variability in ACST incidence rate in the literature. This is probably due to two main factors. The first is the difference is in post-CAS surveillance with some centres performing routine ultrasound Doppler follow-up while others only reporting ACST in symptomatic patients. The second is the difference between included patients in different case series, with acute phase stenting seemingly associated with increased risk.
In patients with neurological deterioration, surgical management was able to achieve recanalization through removal of thrombogenic material. But there were some concerns regarding time-consuming aspects of surgical approach and increased morbidity in such circumstances. Endovascular treatment including thrombectomy, thromboaspiration, PTA-in-stent and stent-in-stent could be applied quickly during the procedure. But, long-term efficacy is still debatable. A role for thrombolysis and facilitated thrombolysis is still to be determined.
In the absence of RCTs, it is difficult to compare the efficacy of different treatment modalities. The critical prognostic points of this potentially devastating complication are the initial clinical presentation expressing the grade of ischemic brain damage, the accurate and timely recognition of the thrombosis and the prompt restoration of oxygenated blood flow into the viable tissue at risk of infarction (ischemic penumbra). Prompt revascularization remains the key to the successful outcome in symptomatic patients and can also justify discrepancies between delayed successful recanalization of the thrombosed stent and functional recovery. In asymptomatic patients, conservative management with anticoagulation still seems the safest option.
As a conclusion, ACST is probably an underestimated clinical entity associated with multiple risk factors. Additional studies must be undertaken to better define optimal management.
REFERENCES
1. Portugal - Doenças cérebro-cardiovasculares em números - 2013: Programa Nacional para as Doenças Cérebro-cardiovasculares; Ferreira, R.C., Neves, R.C., Rodrigues, V.; Direção Geral de Saúde; Lisboa, 2013;
2. Writing G, Naylor AR, Ricco JB, de Borst GJ, Debus S, de Haro J, et al. Editor's Choice - Management of Atherosclerotic Carotid and Vertebral Artery Disease: 2017 Clinical Practice Guidelines of the European Society for Vascular Surgery (ESVS). European journal of vascular and endovascular surgery : the official journal of the European Society for Vascular Surgery. 2018;55(1):3-81.
3. Nallamothu BK, Gurm HS, Ting HH, Goodney PP, Rogers MA, Curtis JP, et al. Operator experience and carotid stenting outcomes in Medicare beneficiaries. Jama. 2011;306(12):1338-43. [ Links ]
4. Moulakakis KG, Mylonas SN, Lazaris A, Tsivgoulis G, Kakisis J, Sfyroeras GS, et al. Acute Carotid Stent Thrombosis: A Comprehensive Review. Vasc Endovascular Surg. 2016;50(7):511-21. doi: 10.1177/1538574416665986. Epub 2016 Sep 19. [ Links ]
5. Xiromeritis K, Dalainas I, Stamatakos M, Katsikas V, Martinakis V, Stamatelopoulos K, et al. Acute carotid stent thrombosis after carotid artery stenting. Eur Rev Med Pharmacol Sci. 2012;16(3):355-62. [ Links ]
6. Watarai H, Kaku Y, Yamada M, Kokuzawa J, Tanaka T, Andoh T, et al. Follow-up study on in-stent thrombosis after carotid stenting using multidetector CT angiography. Neuroradiology. 2009;51(4):243-51. doi:10.1007/s00234-009-0498-7. Epub 2009 Jan 27. [ Links ]
7. Masuo O, Terada T, Matsuda Y, Ogura M, Tsumoto T, Yamaga H, et al. Successful recanalization by in-stent percutaneous transluminal angioplasty with distal protection for acute carotid stent thrombosis. Neurol Med Chir (Tokyo). 2006;46(10):495-9. [ Links ]
8. Mannheim D, Karmeli R. A prospective randomized trial comparing endarterectomy to stenting in severe asymptomatic carotid stenosis. The Journal of cardiovascular surgery. 2017;58(6):814-7. [ Links ]
9. Eckstein HH, Reiff T, Ringleb P, Jansen O, Mansmann U, Hacke W, et al. SPACE-2: A Missed Opportunity to Compare Carotid Endarterectomy, Carotid Stenting, and Best Medical Treatment in Patients with Asymptomatic Carotid Stenoses. European journal of vascular and endovascular surgery : the official journal of the European Society for Vascular Surgery. 2016;51(6):761-5. [ Links ]
10. Rosenfield K, Matsumura JS, Chaturvedi S, Riles T, Ansel GM, Metzger DC, et al. Randomized Trial of Stent versus Surgery for Asymptomatic Carotid Stenosis. The New England journal of medicine. 2016;374(11):1011-20. [ Links ]
11. Silver FL, Mackey A, Clark WM, Brooks W, Timaran CH, Chiu D, et al. Safety of stenting and endarterectomy by symptomatic status in the Carotid Revascularization Endarterectomy Versus Stenting Trial (CREST). Stroke. 2011;42(3):675-80. [ Links ]
12. International Carotid Stenting Study i, Ederle J, Dobson J, Featherstone RL, Bonati LH, van der Worp HB, et al. Carotid artery stenting compared with endarterectomy in patients with symptomatic carotid stenosis (International Carotid Stenting Study): an interim analysis of a randomised controlled trial. Lancet (London, England). 2010;375(9719):985-97. [ Links ]
13. Gurm HS, Yadav JS, Fayad P, Katzen BT, Mishkel GJ, Bajwa TK, et al. Long-term results of carotid stenting versus endarterectomy in high-risk patients. The New England journal of medicine. 2008;358(15):1572-9. [ Links ]
14. Mas JL, Trinquart L, Leys D, Albucher JF, Rousseau H, Viguier A, et al. Endarterectomy Versus Angioplasty in Patients with Symptomatic Severe Carotid Stenosis (EVA-3S) trial: results up to 4 years from a randomised, multicentre trial. The Lancet Neurology. 2008;7(10):885-92. [ Links ]
15. Eckstein HH, Ringleb P, Allenberg JR, Berger J, Fraedrich G, Hacke W, et al. Results of the Stent-Protected Angioplasty versus Carotid Endarterectomy (SPACE) study to treat symptomatic stenoses at 2 years: a multinational, prospective, randomised trial. The Lancet Neurology. 2008;7(10):893-902. [ Links ]
16. Brooks WH, McClure RR, Jones MR, Coleman TL, Breathitt L. Carotid angioplasty and stenting versus carotid endarterectomy for treatment of asymptomatic carotid stenosis: a randomized trial in a community hospital. Neurosurgery. 2004;54(2):318-24; discussion 24-5. [ Links ]
17. Endovascular versus surgical treatment in patients with carotid stenosis in the Carotid and Vertebral Artery Transluminal Angioplasty Study (CAVATAS): a randomised trial. Lancet (London, England). 2001;357(9270):1729-37. [ Links ]
18. Moulakakis KG, Mylonas SN, Lazaris A, Tsivgoulis G, Kakisis J, Sfyroeras GS, et al. Acute Carotid Stent Thrombosis: A Comprehensive Review. Vascular and endovascular surgery. 2016;50(7):511-21. [ Links ]
19. Moulakakis KG, Kakisis J, Tsivgoulis G, Zymvragoudakis V, Spiliopoulos S, Lazaris A, et al. Acute Early Carotid Stent Thrombosis: A Case Series. Ann Vasc Surg. 2017;45:69-78.(doi): 10.1016/j.avsg.2017.04.039. Epub May 5. [ Links ]
20. Koklu E, Yuksel IO, Bayar N, Arslan S. Is Acute Carotid Artery Stent Thrombosis an Avoidable Complication? J Stroke Cerebrovasc Dis. 2015;24(10):2219-22. doi: 10.1016/j.jstrokecerebrovasdis.2015.05.029. Epub Aug 21. [ Links ]
21. Setacci C, de Donato G, Setacci F, Chisci E, Cappelli A, Pieraccini M, et al. Surgical management of acute carotid thrombosis after carotid stenting: a report of three cases. J Vasc Surg. 2005;42(5):993-6. doi: 10.1016/j.jvs.2005.06.031. [ Links ]
22. Deguchi I, Hayashi T, Neki H, Yamane F, Ishihara S, Tanahashi N, et al. Carotid Artery Stenting for Acute Ischemic Stroke Patients after Intravenous Recombinant Tissue Plasminogen Activator Treatment. Intern Med. 2016;55(19):2869-72. doi: 10.169/internalmedicine.55.7038. Epub 2016 Oct 1. [ Links ]
23. Steglich-Arnholm H, Holtmannspotter M, Kondziella D, Wagner A, Stavngaard T, Cronqvist ME, et al. Thrombectomy assisted by carotid stenting in acute ischemic stroke management: benefits and harms. Journal of neurology. 2015;262(12):2668-75. [ Links ]
24. Yilmaz U, Korner H, Muhl-Benninghaus R, Simgen A, Kraus C, Walter S, et al. Acute Occlusions of Dual-Layer Carotid Stents After Endovascular Emergency Treatment of Tandem Lesions. Stroke. 2017;48(8):2171-5. [ Links ]
25. Koklu E, Arslan S, Yuksel IO, Bayar N, Koc P. Acute Carotid Artery Stent Thrombosis Due to Dual Antiplatelet Resistance. Cardiovasc Intervent Radiol. 2015;38(4):1011-4. doi: 10.07/s00270-014-0959-1. Epub 2014 Aug 13. [ Links ]
26. Fifi JT, Brockington C, Narang J, Leesch W, Ewing SL, Bennet H, et al. Clopidogrel resistance is associated with thromboembolic complications in patients undergoing neurovascular stenting. AJNR American journal of neuroradiology. 2013;34(4):716-20. [ Links ]
27. Valgimigli M, Bueno H, Byrne RA, Collet JP, Costa F, Jeppsson A, et al. 2017 ESC focused update on dual antiplatelet therapy in coronary artery disease developed in collaboration with EACTS. Kardiol Pol. 2017;75(12):1217-99. [ Links ]
28. Munich S, Moftakhar R, Lopes D. Recanalization of acute carotid stent occlusion using Penumbra 4Max aspiration catheter: technical report and review of rescue strategies for acute carotid stent occlusion. J Neurointerv Surg. 2014;6(8):e42. doi: 10.1136/neurintsurg-2013-010706.rep. Epub 2013 Oct 22. [ Links ]
29. Kotsugi M, Takayama K, Myouchin K, Wada T, Nakagawa I, Nakagawa H, et al. Carotid Artery Stenting: Investigation of Plaque Protrusion Incidence and Prognosis. JACC Cardiovasc Interv. 2017;10(8):824-31. [ Links ]
30. Bosiers M, de Donato G, Deloose K, Verbist J, Peeters P, Castriota F, et al. Does free cell area influence the outcome in carotid artery stenting? European journal of vascular and endovascular surgery : the official journal of the European Society for Vascular Surgery. 2007;33(2):135-41; discussion 42-3. [ Links ]
31. Kanemaru K, Nishiyama Y, Yoshioka H, Satoh K, Hashimoto K, Hanihara M, et al. In-stent thrombosis after carotid artery stenting despite sufficient antiplatelet therapy in a bladder cancer patient. Journal of stroke and cerebrovascular diseases : the official journal of National Stroke Association. 2013;22(7):1196-200. [ Links ]
32. Tong FC, Cloft HJ, Joseph GJ, Samuels OB, Dion JE. Abciximab rescue in acute carotid stent thrombosis. AJNR Am J Neuroradiol. 2000;21(9):1750-2. [ Links ]
33. Steiner-Boker S, Cejna M, Nasel C, Minar E, Kopp CW. Successful revascularization of acute carotid stent thrombosis by facilitated thrombolysis. AJNR Am J Neuroradiol. 2004;25(8):1411-3. [ Links ]
34. Kim SH, Qureshi AI, Levy EI, Hanel RA, Siddiqui AM, Hopkins LN. Emergency stent placement for symptomatic acute carotid artery occlusion after endarterectomy. Case report. J Neurosurg. 2004;101(1):151-3. doi: 10.3171/jns.2004.101.1.0151. [ Links ]
35. Dhall A, Malani SK, Chadha DS. Thrombosuction for procedural acute thrombosis during high-risk carotid angioplasty-a case report. The Journal of invasive cardiology. 2010;22(8):E144-6. [ Links ]
36. Choi JY, Lee JI, Lee TH, Sung SM, Cho HJ, Ko JK. Emergent Recanalization with Stenting for Acute Stroke due to Athero-Thrombotic Occlusion of the Cervical Internal Carotid Artery : A Single Center Experience. Journal of Korean Neurosurgical Society. 2014;55(6):313-20. [ Links ]
37. Iancu A, Grosz C, Lazar A. Acute carotid stent thrombosis: review of the literature and long-term follow-up. Cardiovasc Revasc Med. 2010;11(2):110-3. doi: 10.1016/j.carrev.2009.02.008. [ Links ]
Endereço para correspondência | Dirección para correspondencia | Correspondence
Correio eletrónico: andreiasmpcoelho@gmail.com (A. Coelho).
Recebido a 27 de julho de 2018
Aceite a 17 de janeiro de 2019