Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Acta Obstétrica e Ginecológica Portuguesa
versión impresa ISSN 1646-5830
Acta Obstet Ginecol Port vol.13 no.4 Coimbra dic. 2019
ISSUE IMAGE/IMAGEM DO TRIMESTRE
Prolonged retention of a second trimester tubal pregnancy
Retenção prolongada de gravidez tubária do segundo trimestre
Verónica São Pedro1, Ricardina Rangeiro2, Cassimo Bique2
Centro Hospitalar e Universitário de Coimbra Hospital Central de Maputo
1 Interna de Formação Específica de Ginecologia e Obstetrícia, Centro Hospitalar e Universitário de Coimbra
2 Assistente Hospitalar de Ginecologia e Obstetrícia, Hospital Central de Maputo
Endereço para correspondência | Dirección para correspondencia | Correspondence
ABSTRACT
Outcomes of tubal ectopic pregnancy include tubal rupture with major hemorrhage, tubal miscarriage, or pregnancy failure with spontaneous resolution but there are some reported cases of advancing pregnancy until 2nd or even 3rd trimester. We present the case of a 34-year-old woman admitted to the Gynecology emergency room with pelvic pain and fever as a consequence of a tubo-ovarian abscess in the context of a 16 weeks demised tubal pregnancy. Pelvic ultrasound enlightened the diagnosis and the woman was submitted to surgery with a favorable recovering.
Keywords: Advanced ectopic pregnancy; Prolonged retention.
Ectopic pregnancy is still a first trimester leading cause of morbidity and mortality, particularly in low income countries lacking accurate diagnostic resources. The site of ectopic implantation may play a role in its clinical course. The isthmic location accounts for 12% of the cases1 and compared with the ampulla, allows a better muscular support and blood supply. Consequently, the pregnancy is more likely to progress and rupture with more abrupt hemodynamic compromise2. The mean gestational age at tubal rupture has been pointed at 7.8 ± 1.093 weeks but there are a few cases of advancing tubal pregnancy in the literature, being the highest gestational age reported at 30 weeks2.
When fetal demise occurs before tubal rupture, there are four processes that a fetus may undergo if not removed: skeletonization, adipocere (soft parts replaced by fatty acids), suppuration and lithopedion formation (literally “stone child”, following sterile infiltration with calcium salts). There are only 330 cases of lithopedion reported in literature, all with abdominal location (primary or after tubal or uterine rupture), the majority of them incidentally found4.
Our patient was a 34-year-old black woman, with a non-investigated primary infertility since her eighteens and with no known diseases or infections. Her menstrual cycles were regular, and she had menstruated 5 days before. She presented with lower abdominal pain and intermittent fever evolving since the previous week. At admission she was febrile (39,5º C), hemodynamically stable and presented a painful lower-quadrants abdominal palpation without rebound tenderness, a non-purulent vaginal discharge and an enlarged uterus with motion tenderness.
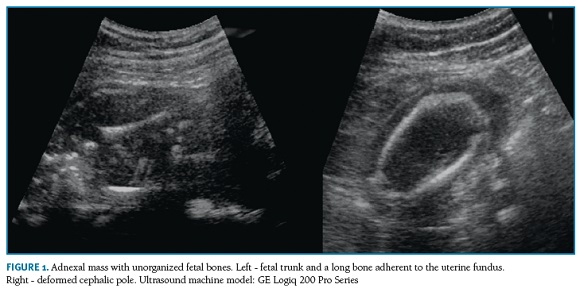
Abdominal gynecological ultrasound examination revealed a prominent nodular formation (compatible with an intramural leiomyoma) and an adnexal formation adherent to the right uterine fundus and right ovary containing unorganized fetal bones and liquid components (Figure 1). A long bone, interpreted as the femur and measuring 22.1 mm, was compatible with a 16 weeks pregnancy at fetal demise. The main differential diagnoses were demised abdominal pregnancy presenting as pelvic abscess, pelvic inflammatory disease with incidental lithopedion or ovarian neoplasm namely an immature teratoma.
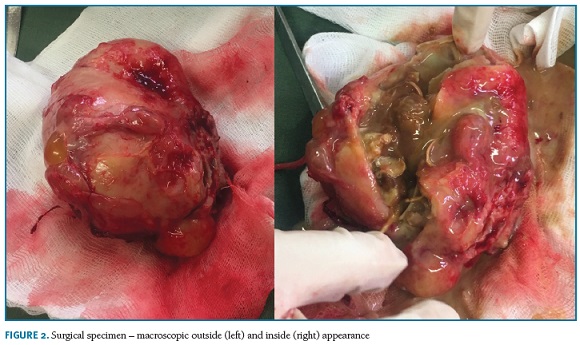
Blood testing revealed a microcytic anemia (hemoglobin level - 7.2 g/dL), leukocytosis (13.9 x 109/L) and were negative for malaria. Neither chorionic gonadotropin nor other ovarian tumor markers were available. She started treatment with ceftriaxone and metronidazole, underwent blood transfusion and a laparotomy was performed. Her pelvic cavity presented severe adhesions and an important anatomic distortion of the right adnexa, where a 9 cm mass with a smooth surface was found and removed. The fibrous capsule was opened revealing purulent material and the remains of an “old pregnancy” (Figure 2). The post-operative recovery was uneventful, and the patient was discharged home three days after.
The histological analysis allowed to classify the original pregnancy as isthmic and the procedure as an adnexectomy (ovarian tissue present) but gave no clues about how long that pregnancy was retained. The tubal location may have played a role in subsequent infection and suppuration process.
REFERENCES
1. Bouyer J, et all. Sites of ectopic pregnancy: a 10-year population-based study of 1800 cases. Hum Reprod 2002; 17(12): 3224-3230. [ Links ]
2. Koçak I, et all. Advanced tubal pregnancy at 30 weeks. J Obstet Gynaecol 2005; 31(4): 341343.
3. Goksedef BPC, et all. Risk factors for rupture in tubal ectopic pregnancy: definition of the clinical findings. Eur J Obstet Gyn R B 2011; 154:96-99.
4. Santoro G, et all. Developmental and Clinical Overview of Lithopaidion. Gynecol Obstet Invest 2014; 78:213-223.
Endereço para correspondência | Dirección para correspondencia | Correspondence
Verónica São Pedro
Portela Lrs, Portugal,
E-Mail: veronicasaopedro@gmail.com
Recebido em: 01/05/2019
Aceite para publicação: 22/11/2019