Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Acta Obstétrica e Ginecológica Portuguesa
versão impressa ISSN 1646-5830
Acta Obstet Ginecol Port vol.10 no.2 Coimbra jun. 2016
IMAGE OF THE TRIMESTER/IMAGEM DO TRIMESTRE
Heterotopic Pregnancy - urgent ultrasonographic diagnosis
Gravidez heterotópica - diagnóstico ecográfico de urgência
Tânia Lima*, Cristina Dias**, Teresa Oliveira***
Centro Materno-Infantil do Norte/ Centro Hospitalar do Porto
*Interna de Ginecologia e Obstetrícia
**Assistente Hospitalar Graduada
***Assistente Hospitalar Sénior
Endereço para correspondência | Dirección para correspondencia | Correspondence
ABSTRACT
Heterotopic pregnancy refers to the coexistence of intrauterine and extrauterine gestations, which can occur in two or more implantation sites. Although still a rare event, its incidence is increasing because of the use of assisted reproductive techniques (ART). The diagnosis is often delayed, which can lead to serious complications. We present a case of heterotopic pregnancy diagnosed in the emergency room in a pregnant woman with hypovolemic shock with the intrauterine pregnancy reaching term.
Keywords: Heterotopic pregnancy; Reproductive techniques; Hemorrhagic shock
Heterotopic pregnancy is defined as the presence of simultaneous pregnancies at two different sites of implantation. The most common place of implantation is the ampulla (70%), followed by the isthmus (12%), the fimbria (11,1%), the ovary (3,2%), the interstitium (2,4%) and the abdomen (1,3%)1. It is often a serious emergency and can become a life-threatening situation in cases of delayed diagnosis. When occur spontaneously, its incidence is estimated to be 1 in 30 000 pregnancies. The use of assisted reproductive techniques (ART) has significantly increased the occurrence of heterotopic pregnancy with estimated rates near 1%2. Several factors contribute to this increased incidence such as an increased incidence of pelvic inflammatory disease, endometriosis, tubal surgery, intrauterine device use and ART procedures with superovulation/ transfer of two or more embryos3.
The most frequent symptoms may mimic those of threatened abortion or ectopic pregnancy, such as abdominal pain, adnexal mass and hypovolemic shock. However, vaginal bleeding that can occur in ectopic pregnancy is unusual to be observed in heterotopic pregnancy due to intact endometrium4. Because of the lack of clinical symptoms, the diagnosis of heterotopic pregnancy can be delayed and lead to major complications because of the rupture of the ectopic pregnancy. Vaginal ultrasound is the gold standard for diagnosis, but at early gestational ages an existing intrauterine pregnancy may lead to a miss diagnosis of an heterotopic pregnancy.
We present a case of a 29-year-old primigravida referred to our emergency with severe abdominal pain and vomiting. She had been diagnosed with primary infertility and the current pregnancy occurred after an Intracytoplasmatic Sperm Injection procedure; two embryos were transferred. An ultrasound was performed during her first medical consultation showing an intrauterine gestational sac with a crown to rump length of 6+1 weeks and with cardiac activity; no other findings were documented.
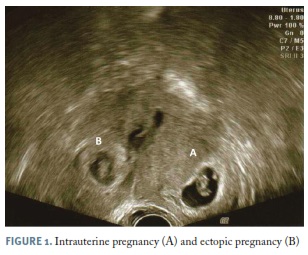
On admission, vital signs were stable and gynaecologic examination was normal without vaginal bleeding. Transvaginal ultrasound revealed two gestational sacs containing two viable embryos - one inside the uterine cavity and other in the right Fallopian tube (Figure 1), both with a crown-rump length of 7 weeks.
Immediately after ultrasound examination, patient presented stronger pain and syncope. Because of hemodynamic instability, we performed an emergent laparotomy under general anesthesia, which revealed a large hemoperitoneum and rupture of the right Fallopian tube that was excised. The anatomopathological examination confirmed an ectopic pregnancy. Intrauterine pregnancy progressed uneventfully till 40 weeks’ gestation when a vaginal delivery occurred.
Since heterotopic pregnancy is a rare event, no treatment standard recommendations exist. Literature advises to perform laparotomy when the patient is hemodynamically unstable or large hemoperitoneum is suspicious. Medical options involve local injection of methotrexate or potassium chloride5 but surgical treatment remains the most common approach. In stable patients, laparoscopy can be a safe and successful option2.
REFERENCES
1. Brown J, Wittich A. Spontaneous heterotopic pregnancy successfully treated via laproscopic surgery with subsequent viable intrauterine pregnancy: a case report. Military medicine 2012; 177:1227-1230. [ Links ]
2. Eom JM, Choi JS, Ko JH, Lee JH, Park SH, Hong JH, et al. Surgical and obstetric outcomes of laparoscopic management for women with heterotopic pregnancy. J Obstet Gynaecol Res 2013; 39:1580-1586. [ Links ]
3. Uysal F, Uysal A, Oztekin DC. Heterotopic quadruplet pregnancy and successful twin outcome. Arch Gynecol Obstet 2013; 288:715-717. [ Links ]
4. Alptekin H, Dal Y. Heterotopic pregnancy following IVF- -ET: successful treatment with salpingostomy under spinal anesthesia and continuation of intrauterine twin pregnancy. Arch Gynecol Obstet 2014; 289:911-914. [ Links ]
5. Wright A, Kowalkzyc CL, Quintero R, Leach RE. Selective embryo reduction in a heterotopic pregnancy using potassium chloride injection resulting in a hematosalpinx. Fertil Steril 1996; 66:1028-1030. [ Links ]
Endereço para correspondência | Dirección para correspondencia | Correspondence
Tânia Lima
E-mail: tanialima_med@hotmail.com
The authors declare no conflict of interest.
Recebido em: 23-02-2016
Aceite para publicação: 23-04-2016