Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Motricidade
versão impressa ISSN 1646-107X
Motri. vol.12 no.1 Ribeira de Pena mar. 2016
https://doi.org/10.6063/motricidade.6020
ARTIGO ORIGINAL
Acute effect of resistance exercise performed at different intensities on the hemodynamics of normotensive men
Efeito do exercício resistido realizado em diferentes intensidades sobre a hemodinâmica de homens normotensos
Mauricio Assis Saldanha1; José Vilaça-Alves1,2*; Gabriel Rodrigues Neto3; Jefferson Da Silva Novaes3; Francisco Saavedra1,2; Victor Machado Reis1,2; Heloisa Thomaz Rabelo4
1 Sport Sciences, Exercise and Health Department, University of Trás-os-Montes e Alto Douro, Vila Real, Portugal
2 Research Center in Sports Sciences, Health Sciences and Human Development, Vila Real, Portugal
3 Department of gymnastics, Federal University of Rio de Janeiro, UFRJ, Rio de Janeiro, RJ, Brazil
4 Exercise Research Laboratory, University Center East of Minas Gerais, Ipatinga, Brazil
ABSTRACT
The aim of this study was to investigate the acute effect of resistance exercise performed at different intensities on the hemodynamics of normotensive men. The study included 10 normotensive and recreationally-trained men (25.40 ± 6.90 years) performed the following three experimental protocols in a randomized order: a) 60% of 8RM; b) 80% of 8RM; c) 100% of 8RM. All protocols performed six exercises (Leg Press, Vertical Bench Press, Leg Flexion, Close-Grip Seated Row, Leg Extension and Shoulder Press) with three sets of eight repetitions for each exercise. Systolic blood pressure (SBP), diastolic blood pressure (DBP), heart rate (HR) and double product (DP) were measured at rest, at the end of exercise and during the 60-minute post-exercise. The findings showed that there was a significant reduction in the faster SBP with a longer duration (p< 0.0001) for the 100% of 8RM intensity, but without significant decreases in DBP for all intensities (p> 0.05). There were significantly higher elevations in HR and DP for 100% of 8RM at all times (p<0.0001). We conclude that high intensities (100% of 8RM) promote post-exercise hypotension with faster responses and greater duration and increase HR and DP in normotensive men.
Keywords: post-exercise hypotension, blood pressure, double product, heart rate
RESUMO
O objetivo do presente estudo foi verificar o efeito agudo do exercício de força realizado em diferentes intensidades sobre a hemodinâmica de homens normotensos. Participaram do estudo 10 homens aparentemente saudáveis (25.40 ± 6.90) divididos aleatoriamente em três protocolos experimentais: a) 60% de 8RM; b) 80% de 8RM; c) 100% de 8RM. Todos os protocolos realizaram seis exercícios (leg press 45°, supino vertical, flexão de joelhos, remada sentada fechada, extensão de joelhos e desenvolvimento na máquina), com três series de oito repetições para cada exercício. A pressão arterial sistólica (PAS), diastólica (PAD), freqüência cardíaca (FC) e o duplo produto (DP) foram mensurados em repouso, no final dos exercícios e durante os 60 minutos pós-exercício. Os resultados mostram que houve redução significativa na PAS mais rápida com maior duração (p< 0.05) para intensidade 100% de 8RM, porém sem reduções significativas na PAD para todas as intensidades (p> 0.05). Houve maiores elevações significativas na FC e no DP para 100% de 8RM em todos os momentos (p> 0.05). Conclui-se que altas intensidades (100% de 8RM) promovem hipotensão pós-exercício com respostas mais rápidas e de maior duração e eleva a FC e o DP de homens normotensos.
Palavras-Chave: hipotensão pós-exercício, pressão arterial, duplo produto, frequência cardíaca
INTRODUCTION
Arterial hypertension (AH) is considered one of the fastest growing chronic dysfunctions among modern societies. This condition is associated with an increased incidence of causes of deaths from cardiovascular disease, stroke, coronary disease, heart failure, peripheral arterial disease and renal failure (ACSM, 2004; Mancia et al., 2007). Genetic, low levels of physical activity, poor dietary habits and excess body fat, can be highlighted as the main cause for the establishment of hypertension (Hagberg, Park, & Brown, 2000; Mancia et al., 2007). Thus, changes in lifestyle through combined resistance exercise (RE) with aerobic exercise are recommended as an important non-pharmacological tool for prevention and treatment of hypertension in normotensive and hypertensive subjects, respectively (ACSM, 2014).
In this sense, the RE has been used in order to reduce systolic blood pressure (SBP) and diastolic blood pressure (DBP) to values below resting levels after the RE session, this phenomenon being known as post-exercise hypotension (PEH) (De Salles et al., 2010; Rezk, Marrache, Tinucci, Mion Jr, & Forjaz, 2006). PEH varies considerably depending on different RE prescription variables (intensity, training volume, muscular action, number of sets, number of repetitions, load, speed, recovery interval, order of exercises and weekly frequency) and the health status of the participants (De Salles et al., 2010; Jannig, Cardoso, Fleischmann, Coelho, & Carvalho, 2009; Matos et al., 2013; Melo, Alencar Filho, Tinucci, Mion Jr, & Forjaz, 2006; Tibana, Boullosa, Leicht, & Prestes, 2013).
The intensity of the RE is one of the most manipulated variables. So, to programme a save and efficiently the RE training, it is important to know the influence of the intensity on the hemodynamic responses in normotensive subjects.
Studies have evaluated hypotensive responses after RE sessions held at different intensities (Bentes et al., 2015; Matos et al., 2013; Mohebbi, Rahmaninia, Vatani, & Faraji, 2009; O'Connor, Bryant, Veltri, & Gebhardt, 1993; Polito, Simão, Senna, & Farinatti, 2003; Simão, Fleck, Polito, Monteiro, & Farinatti, 2005). Studies by Simão, Fleck, Polito, Monteiro, and Farinatti (2005) and Polito, Simão, Senna, and Farinatti (2003) suggest that RE sessions with high intensities (100% of 6RM to failure) are more effective than moderate intensity programs (12 repetitions with 50% of 6RM) resulting in a longer duration PEH in trained subjects. Mohebbi, Rahmaninia, Vatani, and Faraji (2009) and Matos et al. (2013) compared the effect of different intensities (40% and 80% of 1RM) with different volumes of training (70%, 80% and 90% of 1RM) respectively on blood pressure (BP) in normotensive men. Both studies showed significant reductions in SBP, but without significantly reducing DBP. Bentes et al. (2015) observed significant reductions in SBP and DBP after submitting 13 women to different intensities (60% and 80% of 1RM) and different order of exercises. Diverging from these studies, O'Connor, Bryant, Veltri, and Gebhardt (1993) investigated the effect of RE performed at different intensities (40%, 60%, 80% of 10RM) on the blood pressure of normotensive trained women. The authors found no significant reductions in post-exercise BP.
The resistance training methods used in the presented study, alternated resistance exercises by segments, are routinely applied in the fitness centers and their influence in the hemodynamics responses are scarcity in the current scientific literature. To your Knowledge, only Bentes et al., (2015), analyzed the effect of the resistance exercise intensities on the hypotensive response, when the resistance training methodology were alternated the exercise by segments, but in normotensive women. In order that, the aim of this study was to investigate the acute effect of resistance exercises performed at different intensities (60%, 80% and 100% of 8RM), when the resistance training methodology were alternated the exercises by segments, on the hemodynamics of normotensive men.
METHOD
Participants
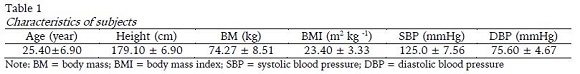
Ten normotensive and recreationally-trained men (18-34 years) participated in the study (Table 1). The sample size was made using the G*Power 3.1 software. Based on a post hoc analysis, we adopted α = 0.05, a correlation coefficient of 0.5, a Nonsphericity correction of 1 and an effect size of 0.50. It was found that the sample size was sufficient to provide a statistical power of 89.9%. Procedures suggested by Beck (2013) were adopted to calculate the sample.
Were excluded from the study: (a) smokers, (b) those who had some type of musculoskeletal injury in their superior or inferior limbs, and (c) those who answered affirmatively to any of the items of the Physical Activity Readiness Questionnaire (PAR-Q) (Shephard, 1988). After being explained the risks and benefits of the study, subjects signed an agreement form prepared in accordance with the Declaration of Helsinki. The study was approved by the Ethics Committee on Human Research under protocol number 61.318.12.
Measures
After the anthropometrical evaluation, participants were prepared through three nonconsecutive sessions for the session of RE. The resistance exercises were conducted alternately in segments, in the following order: 45° leg press (45° LP), vertical bench press (VBP), leg flexion (LF), close grip seated row (CGSR), leg extension (LE) and shoulder press (SP).
Then, we evaluated muscle strength (8RM test and retest) on nonconsecutive days. After these visits participants, randomly by raffle, performed all three experimental protocols in a crossover model: a) intensity 60% of 8RM; b) intensity 80% of 8RM; c) intensity 100% of 8 RM. Each protocol performed 3 sets of 8 reps with a two-minute rest between sets and exercises. The movement of realization of repetitions was kept at a cadence of 60 beats/min controlled by a metronome (Sanny AD1010, São Paulo, Brazil).
All three procedures were performed at the same time of day (between 09h and 11h) to control the diurnal variation in BP and HR. The measurement of SBP, DBP and HR was measured before (pre), immediately after (post), 10 min (post-10), 20 min (post-20), 30 min (post-30), 40 min (post-40) 50 min (post-50) and 60 min (after-60) after all protocols.
This study used a randomized crossover design. Participants were tested > 2 hours postprandial and were instructed to avoid caffeine, alcohol, chocolate, medicine and exercises before and on the day of testing. During all sessions of strength exercises, subjects were instructed not to perform the Valsalva maneuver.
Procedures
Anthropometric Assessment
Height and weight were measured to the nearest 0.5 cm and 0.1 kg, respectively, using a stadiometer of Welmy (Santa Barbara D'oeste, São Paulo, 2002) and a Sanny scale (AD1010, São Paulo, Brazil).
Blood Pressure, Heart Rate and Double Product
Before and after each session, participants were provided with an electronic BP monitor (Microlife ® BP 3AC1-1, China). The cuff placed on the right arm was completely wrapped, covering at least two thirds of the upper arm. This equipment was used for all pre- and post-session measurements of BP. HR was continuously monitored throughout the pre- and post-session (Polar FT-1, Oulu, Finland). Double product (DP) was obtained by multiplying the HR (bpm) x SBP (mmHg). All measurements were performed according to the guidelines of the American Heart Association (Pickering et al., 2005).
Eight Repetitions Maximum Test (8RM)
To obtain the reliability of the load in the 8RM test, the test and retest were conducted during two nonconsecutive days separated by a minimum of 72 hours. For 8RM testing, each individual performed a maximum of 3 attempts at each exercise with an interval of 5 minutes between attempts. After discovering the 8RM load for a particular exercise, an interval of no less than 10 min was allowed before the determination of 8RM for the next exercise. The weight considered as maximum load (100% of 8 RM) was the one which allowed the volunteer to stand the entire movement until the last repetition without concentric failure in his real limit for the stipulated speed. The following strategies were chosen to reduce the margin of error in data collection procedures: (a) standardized instructions were given before testing, so that each test subject was aware of all the routines involved in the data collection; (b) the tested individual was instructed on the proper technique of performing the exercise, in which no break was allowed between the concentric and eccentric phases, and the movement of realization of repetitions was set at a rate of 60 beats/min, controlled by a metronome (Sanny AD1010, São Paulo, Brazil); (c) all participants received standardized verbal encouragement during testing and (d) all tests were performed at the same time of day for each session. The highest load reached between both days was considered the 8RM test.
Statistical analyses
Statistical analysis was initially performed using the Shapiro-Wilk normality test, and data sphericity through the Levene and Mauchly test respectively. Variables showed a normal distribution of homoscedasticity (p> 0.05). To test the reproducibility of the load between the 8RM test and retest, we used the intraclass correlation coefficient (ICC). Repeated measures analysis of variance (GLM) was followed by the post hoc Bonferroni test to determine possible differences in dependent variables. Furthermore, partial eta (hp2) was calculated to evaluate effect size. The significance level was set at p< 0.05. All statistical analyses were performed using SPSS statistical software, package version 20.0 (SPSS Inc., Chicago, IL).
RESULTS
The intraclass correlation coefficients of the 8RM test for each exercise were: 45° LP=0.96; VBP=0.97; LF=0.83; CGSR=0.91; LE=0.80, SP=0.90.
Blood Pressure
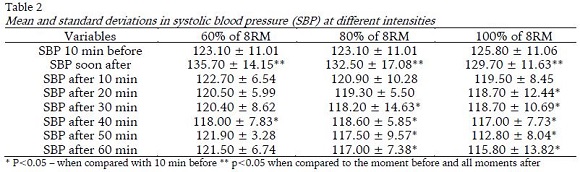
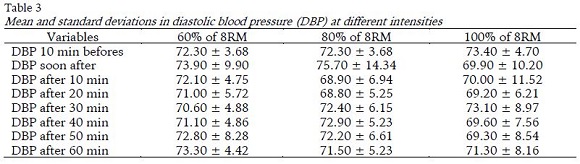
In the comparative analysis of SBP, no significant differences between protocols (intensity) were observed, for all moments (p> 0.05). In the analysis of moments, significant reductions (F= 10.845; p< 0.001; hp2= 0.287) were found for all intensities when comparing pre-exercise moments and post-exercise moments. PEH occurred faster inversely to the used intensity, starting at the moments 20, 30 and 40 minutes after the 100%, 80% and 60% sessions of 8RM, respectively (Table 2). In the comparative analysis of DBP, it was noted that there were no significant effects between moments and protocols (p> 0.05), as shown in Table 3.
Heart Rate
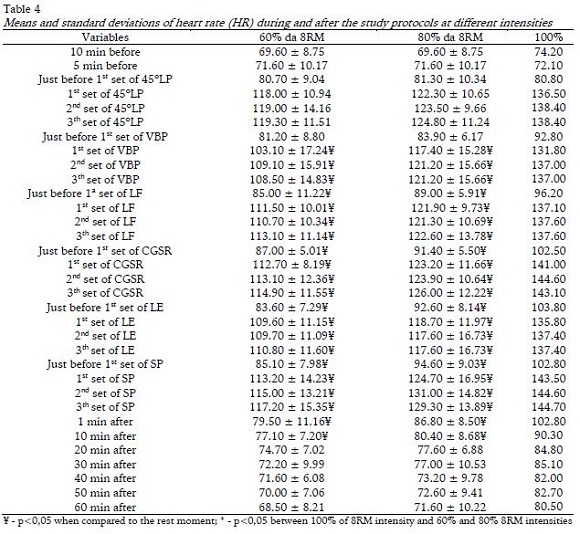
Table 4 shows the comparative analysis of HR between protocols. It was observed that there were significant increases comparing the intensity of 100% of 8RM to the intensities 60% and 80% of 8RM, at all moments during and after the RE sessions (F= 13.468; p< 0.001; hp2= 0.499). In the analysis between moments, significant increases were observed (F= 235.843; p< 0.001; hp2= 0.897), with higher values until 10 minutes after the intensities 60% and 80% of 8RM, when compared to the rest moment. For the intensity 100% of 8RM, the increase compared with rest was extended up to 50 minutes.
Double Product
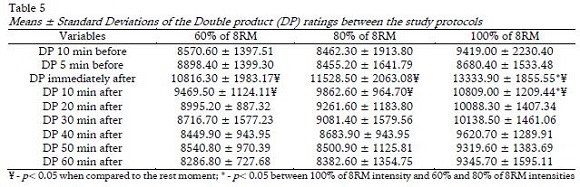
In the comparative analysis of the DP, significant differences were observed (F= 4.344; p= 0.023; hp2= 0.102) between intensities. When comparing intensities (100% vs. 60% 8RM) it was observed that the 100% of 8RM intensity showed significantly higher values than the 60% of 8RM intensity, in the moments immediately after and 10 minutes after. In the analysis of the moments, we observed significant increases for the three protocols (F= 43.967; p< 0.001; hp2= 0.620) when comparing the pre-exercise moment with the moments immediately after and 10 minutes after (Table 5).
DISCUSSION
This study investigated the acute effect of RE performed at different intensities (60%, 80% and 100% of 8RM), when the resistance training methodology were alternated the exercises by segments, on the hemodynamics of normotensive men. The main finding of this study was that the duration of the PEH is not connected to the intensity of ER load and the different intensities resulted in a hypotensive effect of the SBP at 60 min post exercise session in the high intensities analyzed. However, after comparing the intensities, no significant differences were observed between intensities. Our results are not corroborated by studies by Simão et al. (2005) and Polito et al. (2003), which reported that significant reductions in SBP are influenced by high intensities (100% of 6RM), causing a PEH of longer duration, but corroborated with Bentes et al. (2015). A possible reason for this contradiction with the present study may be related to the order organization of the exercises used on the present study and Bentes et al. (2015), study who were different from Simão et al. (2005) and Polito et al. (2003). It seems that when the resistance exercises were alternated by segments in the same sessions, the different intensities not influence the hypotensive responses. These results may be explained by the large muscle mass involved on the resistance exercises promoting a greater vasodilation and when the alternation between upper and lower body exercise order were performed can resulting in a greater decrease in vascular resistance.
The differences between the times on the PEH when analyzed the intensities individually showed a faster PEH when was used the intensity of 100% of 8RM. It is likely that RE performed at high intensity is able to promote higher blood mobilization (Copeland et al., 1996). In this way, it is speculated that, because a greater blood volume is mobilized, the high-intensity protocol may have stimulated an increased production of nitric oxide, which is a powerful vasodilator agent (Brown et al., 2000), promoting a relaxation in the endothelium and consequently a reduction in SBP.
Regarding DBP, no significant change was observed in this experiment. This fact may be related to the sample characteristics – specifically trained and healthy subjects. More significant changes in DBP are mainly found in sedentary and hypertensive subjects (Kenney & Seals, 1993; Mediano, Paravidino, Simão, Pontes, & Polito, 2005). Sedentary and hypertensive subjects have an increased sympathetic activity and peripheral vascular resistance (PVR). Moreover, physically trained individuals have significant autonomic and hemodynamic adaptations, such as resting bradycardia and decreased PVR, influencing the cardiovascular system (Monteiro & Sobral Filho, 2004). These findings corroborate studies by Mohebbi et al. (2009) and Matos et al. (2013) which compared the effect of different intensities (40% and 80% of 1RM and 70%, 80% and 90% of 1RM, respectively) on BP of apparently healthy normotensive men. Both studies showed significant reductions in SBP, but without significantly reducing DBP.
Regarding HR, significant increases were observed with the use of the intensity 100% of 8RM in relation to intensities 60% and 80% of 8RM, at the moments during and after RE. During exercise, the amount of blood pumped by the heart depends on the increased oxygen demand of the skeletal muscles involved. Therefore, in higher rates of work, stimulation of the sinoatrial and atrioventricular nodes of the sympathetic nervous system causes increased strength of the myocardial contraction considerably raising HR (Powers & Howley, 2009). Regarding the HR response after exercise, most studies demonstrated an increase in this variable when using high and moderate intensities (Cléroux, Kouame, Nadeau, Coulombe, & Lacourciere, 1992; Forjaz, Matsudaira, Rodrigues, Nunes, & Negrão, 1998). In the present investigation, the HR after exercise was significantly higher compared to rest until the 20th minute with intensities 80% and 60% of 8RM, and until the 50th minute at 100% intensity. It seems that increasing the intensity of exercise may have resulted in increased concentrations of metabolite, reducing the intracellular hydrogen ionic potential. The presence of a buffering system is needed, this mechanism possibly being more time consuming according to the cumulative levels of hydrogen ions (Ascensão, Magalhães, Oliveira, Duarte, & Soares, 2003). In this sense, it seems that the regulation of muscle sympathetic afferent activity is influenced by the accumulation of adenosine, hydrogen and other metabolites, impeding the reduction of HR to pre-exercise levels (Forjaz et al., 1998).
In turn, the DP variable was significantly greater for the protocol performed with the intensity of 100% of 8RM compared with the intensity of 60% of 8RM at the moments soon after and 10 minutes after, which reflects an increased cardiac effort at higher RE intensities.
Some studies in hypertensive elderly individuals explain PEH mainly through changes in cardiac output (Hagberg, Montain, & Martin, 1987). Other studies on young healthy subjects explain PEH by peripheral vascular resistance (Halliwill, Taylor, Hartwig, & Eckberg, 1996). In our study, one explanation for the PEH effect takes into account the change in cardiac output (CO) due to a decrease in stroke volume (SV). Thus, the observed increase in HR after exercise is probably due to the attempt of the body to compensate for the reduction of SV to keep the CO. It is noteworthy that the reduction of SV is proportional to the exercise intensity (Halliwill et al., 1996), which explains the increase in HR after more strenuous exercise. It is believed that peripheral vascular resistance also had an important responsibility for PEH in our study, given the various substances produced by exercise which are responsible for presenting a local vasodilation effect in the active muscles (lactate, potassium, adenosine) and inactive muscles (opioids, decreased muscle sympathetic activity). In our experiment the method we used was by alternating segments, a method which promotes greater vascular mobilization (Jannig et al., 2009). Therefore, it is likely that this method may have contributed to the decrease in PVR. Thus, in this study, it seems that the highest DP, determined by the higher load intensity of RE, was crucial to a greater reduction in SV and PVR after the exercise intensity of 100% of 8RM, thus influencing the duration of the PEH effect in SBP.
CONCLUSION
Different intensities (60%, 80% and 100% of 8RM) can be effective in controlling blood pressure in normotensive adult men. The duration of the PEH is not connected to the intensity of ER load and the different intensities resulted in a hypotensive effect of the SBP at 60 min post exercise session in the high intensities analyzed. The elevations of HR and DP variables are proportional to the intensity of RE, with higher values when greater load intensity is used, during and after RE. It is important to refer that the conclusions of this study only should been applied when the order of organization of resistance exercises are alternated by segments and in normotensive men.
REFERENCES
American College of Sport Medicine. (2014). ACSMs Guidelines for Exercise Testing and Prescription. Lippincott Williams & Wilkins. [ Links ]
Ascensão, A., Magalhães, J., Oliveira, J., Duarte, J., & Soares, J. (2003). Physiology of muscle fatigue. Conceptual definition, study models and fatigue mechanisms of central and peripheral origin. Revista Portuguesa de Ciências do Desporto, 3(1), 108-123. [ Links ]
Beck, T. W. (2013). The importance of a priori sample size estimation in strength and conditioning research. Journal of Strength and Conditioning Research, 27(8), 2323-2337. doi: 10.1519/JSC.0b013e318278eea0 [ Links ]
Bentes, C. M., Costa, P. B., Neto, G. R., Costa e Silva, G. V., de Salles, B. F., Miranda, H. L., & Novaes, J. S. (2015). Hypotensive effects and performance responses between different resistance training intensities and exercise orders in apparently health women. Clinical Physiology and Functional Imaging, 35(3), 185–190. https://doi.org/10.1111/cpf.12144 [ Links ]
Brown, M. D., Srinivasan, M., Hogikyan, R. V., Dengel, D. R., Glickman, S. G., Galecki, A., & Supiano, M. A. (2000). Nitric oxide biomarkers increase during exercise-induced vasodilation in the forearm. International Journal of Sports Medicine, 21(2), 83-89. [ Links ]
Brown, S. P., Clemons, J. M., He, Q., & Liu, S. U. (1994). Effects of resistance exercise and cycling on recovery blood pressure. Journal of Sports Sciences, 12(5), 463-468. [ Links ]
Cléroux, J., Kouame, N., Nadeau, A., Coulombe, D., & Lacourciere, Y. (1992). After effects of exercise on a regional and systemic hemodynamics in hypertension. Hypertension, 19(2), 183-191. [ Links ]
Copeland, S. R., Mills, M. C., Lerner, J. L., Crizer, M. F., Thompson, C. W., & Sullivan, J. M. (1996). Hemodynamic effects of aerobic vs resistance exercise. Journal of Human Hypertension, 10(11), 747-753. [ Links ]
Cornelissen, V. A., & Fagard, R. H. (2005). Effect of resistance training on resting blood pressure: a meta-analysis of randomized controlled trials. Journal of Hypertension, 23(2), 251-259. [ Links ]
Cornelissen, V. A., & Smart, N. A. (2013). Exercise Training for Blood Pressure: A Systematic Review and Meta-analysis. Journal of the American Heart Association, 2(1), e004473. doi: 10.1161/JAHA.112.004473 [ Links ]
De Salles, B. F., Maior, A. S., Polito, M., Novaes, J., Alexander, J., Rhea, M., & Simão, R. (2010). Influence of rest interval lengths on hypotensive response after strength training sessions performed by older men. Journal of Strength and Conditioning Research, 24(11), 3049-3054. doi: 10.1519/JSC.0b013e3181ddb207 [ Links ]
Focht, B. C., & Koltyn, K. F. (1999). Influence of resistance exercise of different intensities on state anxiety and blood pressure. Medicine and Science in Sports and Exercise, 31(3), 456-463. [ Links ]
Forjaz, C. L. M., Matsudaira, Y., Rodrigues, F. B., Nunes, N., & Negrão, C. E. (1998). Post-exercise changes in blood pressure, heart rate and rate pressure product at different exercise intensities in normotensive humans. Brazilian Journal of Medical and Biological Research, 31(10), 1247-1255. [ Links ]
Hagberg, J. M., Montain, S. J., & Martin, W. H. (1987). Blood pressure and hemodynamic responses after exercise in older hypertensives. Journal of Applied Physiology, 63(1), 270-276. [ Links ]
Hagberg, J. M., Park, J. J., & Brown, M. D. (2000). The role of exercise training in the treatment of hypertension. Sports Medicine, 30(3), 193-206. [ Links ]
Halliwill, J. R., Taylor, J. A., Hartwig, T. D., & Eckberg, D. L. (1996). Augmented baroreflex heart rate gain after moderate-intensity, dynamic exercise. American Journal of Physiology, 270(2), 420-426. [ Links ]
Jannig, P. R., Cardoso, A. C., Fleischmann, E., Coelho, C. W., & Carvalho, T. (2009). Influence of resistance exercises order performance on post-exercise hypotension in hypertensive elderly. Revista Brasileira de Medicina do Esporte, 15(5), 338-341. [ Links ]
Kenney, M. J., & Seals, D. R. (1993). Postexercise hypotension. Key features, mechanisms, and clinical significance. Hypertension, 22(5), 653-664. [ Links ]
Mancia, G., De Backer, G., Dominiczak, A., Cifkova, R., Fagard, R., Germano, G., . . . Laurent, S. (2007). Guidelines for the management of arterial hypertension The Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). European Heart Journal, 28(12), 1462-1536. [ Links ]
Matos, D. G., Aidar, F. J., Filho, M. L. M., Silva, S. R., Oliveira, J. C., Klain, I. P., . . . Dantas, E. H. M. (2013). Analysis of hemodynamic responses to resistance exercise performed with different intensities and recovery intervals. Health, 5(2), 159-165. doi: 10.4236/health.2013.52021 [ Links ]
Mediano, M. F. F., Paravidino, V., Simão, R., Pontes, F. L., & Polito, M. D. (2005). Subacute behavior of the blood pressure after power training in controlled hypertensive individuals. Revista Brasileira de Medicina do Esporte, 11(6), 337-340. [ Links ]
Melo, C. M., Alencar Filho, A. C., Tinucci, T., Mion Jr, D., & Forjaz, C. L. M. (2006). Postexercise hypotension induced by low-intensity resistance exercise in hypertensive women receiving captopril. Blood Pressure Monitoring, 11(4), 183-189. [ Links ]
Mohebbi, H., Rahmaninia, F., Vatani, S. D., & Faraji, H. (2009). Post-resistance exercise hypotensive responses at different intensities and volumes. Facta Universitatis, 7(2), 171-179. [ Links ]
Monteiro, M. F., & Sobral Filho, D. C. (2004). Physical exercise and blood pressure control. Revista Brasileira de Medicina do Esporte, 10(6), 513-516. [ Links ]
O'Connor, P. J., Bryant, C. X., Veltri, J. P., & Gebhardt, S. M. (1993). State anxiety and ambulatory blood pressure following resistance exercise in females. Medicine and Science in Sports and Exercise, 25(4), 516-521. [ Links ]
Pickering, T. G., Hall, J. E., Appel, L. J., Falkner, B. E., Graves, J., Hill, M. N., . . . Roccella, E. J. (2005). Recommendations for blood pressure measurement in humans and experimental animals part 1: blood pressure measurement in humans: a statement for professionals from the Subcommittee of Professional and Public Education of the American Heart Association Council on High Blood Pressure Research. Circulation, 111(5), 697-716. [ Links ]
Polito, M. D., Simão, R., Senna, G. W., & Farinatti, P. T. V. (2003). Hypotensive effects of resistance exercises performed at different intensities and same work volumes. Revista Brasileira de Medicina do Esporte, 9(2), 74-77. [ Links ]
Powers, S. K., & Howley, E. D. (2009). Exercise physiology: Theory and Application to Fitness and Performance (6ª ed.). Barueri: Manole. [ Links ]
Rezk, C. C., Marrache, R. C. B., Tinucci, T., Mion Jr, D., & Forjaz, C. L. D. M. (2006). Post-resistance exercise hypotension, hemodynamics, and heart rate variability: influence of exercise intensity. European Journal of Applied Physiology, 98(1), 105-112. [ Links ]
Shephard, R. J. (1988). PAR-Q, Canadian Home Fitness Test and exercise screening alternatives. Sports Medicine, 5(3), 185-195. [ Links ]
Simão, R., Fleck, S. J., Polito, M., Monteiro, W., & Farinatti, P. (2005). Effects of resistance training intensity, volume, and session format on the postexercise hypotensive response. Journal of Strength and Conditioning Research, 19(4), 853-858. [ Links ]
Tibana, R. A., Boullosa, D. A., Leicht, A. S., & Prestes, J. (2013). Women with metabolic syndrome present different autonomic modulation and blood pressure response to an acute resistance exercise session compared with women without metabolic syndrome. Clinical Physiology and Functional Imaging, 33(5), 364-372. doi: 10.1111/cpf.12038. [ Links ]
Acknowledgments:
Nothing to declare
Conflict of interest:
Nothing to declare
Funding
Nothing to declare
Manuscript received at October 23rd 2014; Accepted at October 24th 2015
*Corresponding author: University of Trás-os-Montes and Alto Douro, Sports Sciences Dept., Sport Complex of UTAD, Quinta de Prados, 5000-000, Vila Real, Portugal E-mail: josevilaca@utad.pt