Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Psicologia, Saúde & Doenças
versão impressa ISSN 1645-0086
Psic., Saúde & Doenças vol.14 no.1 Lisboa mar. 2013
What do pediatrics Residents know about the psychological factors in constipation?
O que Residentes de pediatria sabem sobre os fatores psicológicos na constipação?
Claudia dos Reis Motta1,4, Sandro Iêgo1,2, Juliana de Oliveira3, Hélio de Castro4, Luciana Rodrigues Silva5
1 Federal University of Bahia (UFBA). Salvador, Bahia, Brazil;
2 Instituto Bahiano de Análise do Comportamento (IBAC) Salvador, Bahia, Brazil; 3 Bahia School of Medicine and Public Health. Salvador, Bahia, Brazil; 4 Sede Psicanálise Instuitution, Salvador, Bahia, Brazil; 5 Department of Pediatric Gastroenterology and Hepatology, Complexo Hospitalar HUPES-CPPHO, Federal University of Bahia, Salvador, Bahia, Brazil.
ABSTRACT
The objective of the present work was to evaluate what pediatrics Residents know about constipation and associated psychological factors.A cross-sectional, descriptive study was developed with 42 medical Residents from Salvador, Brazil, using a questionnaire on constipation diagnosis, therapy, complications and related factors.The results show that 95.2% mentioned diet as a triggering factor of constipation, 26.6% organic diseases, 38.0% parents emotional factors, and 23.8% childs emotional factors. Associated aspects included hostile family environment/sexual abuse (88.1%), parental crisis (66.7%), fear/anxiety (78.6%), maternal control (61.9%). Reasons for referring the patient to psychotherapy included psychoaffective aspects (76.1%). Regarding treatment, 97.6% performed dietary changes. All acknowledged the need for more information on Functional constipation (FC). Multidisciplinary educational programs should be developed from undergraduate level up to medical residency.
Keywords- constipation; knowledge; medical residency; psychotherapy.
RESUMO
O objetivo do presente estudo foi avaliar o conhecimento de Residentes de pediatria sobre prisão de ventre e fatores psicológicos associados. Estudo descritivo transversal com 42 residentes de Salvador, Brasil, com questionário sobre diagnóstico, terapêutica, complicações e fatores relacionados. Os resultados mostram que 95,2% citaram dieta como fator determinante da constipação, 26,6% doenças orgânicas, 38,0% fatores emocionais dos pais, e 23,8%, na criança. Aspectos associados mencionados: ambiente familiar agressivo/abuso sexual (88,1%), crise parental (66,7%), medo/ansiedade (78,6%), controle materno. Como indicadores para psicoterapia 76,1% aspectos psicoafetivos. Quanto ao tratamento 97,6% indica mudança dietética. Todos desejam mais informações sobre a CIF. Devem ser desenvolvidos programas educacionais multidisciplinares desde a graduação até a residência médica em Pediatria.
Palavras-chave -constipação intestinal; conhecimento; residência médica; psicoterapia.
Functional constipation (FC), defined according to the Rome III criteria (Rasquin et al., 2006) is a varying combination of chronic gastrointestinal symptoms unexplained by biochemical or physical abnormalities, and is a common condition in children and adolescents of 4-18 years of age. The North American Society for Pediatric Gastroenterology, Hepatology and Nutrition (NASPGHAN) defines FC as a delay or difficulty in evacuating, sufficient to cause significant distress to the patient and present for two or more weeks (van den Berg, Benninga, & Di Lorenzo, 2006).
The causes of functional constipation are multifactorial and include those related to behavioral disorders, to the neurological axis and to alterations in the motility of the digestive tract, as well as psychological and emotional factors (Farnam, Rafeey, Farhang & Khodjastejafari, 2009; Poenaru et al., 1997; Silva, 2009; van den Berg et al., 2010). Psychological distress may lead, for example, to increased bowel motility and abdominal discomfort through the central, autonomic and enteric nervous systems (Drossman, Talley, Leserman, Olden & Barreiro, 1995; Leroi et al., 1995).
In the two categories of idiopathic constipation, slow transit constipation and normal transit constipation, psychological distress and depression may contribute towards maintaining and exacerbating the symptoms of gastrointestinal disorders, and may also be the cause of constipation (Chattat et al., 1997). Some investigators have emphasized the significant and reciprocal relationship between these two functional gastrointestinal disorders and psychological illness (Alander, Svärdsudd, Johansson & Agréus, 2005).
Aspects such as a family history of constipation, an unstable parental relationship, genetic factors, diet, psychological and psychiatric factors, social habits, cultural and social beliefs, the parent-child relationship, stressful events in the family, routine activities and toilet habits, have often been found to be associated with FC (Amendola, De Angelis, Dalloglio, Di Abriola & Di Lorenzo, 2003; Farnam et al., 2009; Poenaru et al., 1997; van den Berg et al., 2006), including stubbornness in general and stubbornness with respect to using the toilet (Burket et al., 2006). Some children with constipation were toilet-trained at an early age and are afraid of sitting on the toilet because they associate evacuation with a painful experience (Motta, Silva & Castro, 2010; Rasquin et al., 2006; Silva, 2009). In addition to these factors, family aggression and hostility have been described as emotional factors associated with FC (Lisboa et al., 2008). Children with nocturnal enuresis, constipation, fecal incontinence and those with a tendency to produce very large stools are at an increased risk of behavioral problems (van Dijk, Benninga, Grootenhuis, & Last, 2010). Investigation of this causal relationship is necessary for the therapeutic management of patients with severe chronic constipation, including behavioral screening in the diagnosis of children and adolescents with FC (Lisboa et al., 2008; van Dijk et al., 2010).
Symbolically, retention indicates possessive control between the mother and child (Freud, 1905). Retention requires control and passivity. Aggressiveness is channeled to the Ego (Freud, 1905). The feces enter into the childs subjectivity through maternal demands (Lacan, 1958). At the same time, the mothers anxiety may be a possible factor leading to constipation in the child (Lisboa et al., 2008) and the profile of an over-strict mother with an obsessive personality (Farnam et al., 2009; Motta et al., 2010) may govern the behavior and destructive personality of her children (Farnam et al., 2009).
Considering that psychological and emotional aspects constitute risk factors for FC, psychological intervention emerges as a promising strategy for the prevention and treatment of the condition. Among the different types of psychotherapeutic management available, psychoanalysis proposes a treatment focussed on confronting the psychic conflicts underlying the symptoms and may be of help in this process by redefining the significance of the subjects relationship with him/herself and with the world. Its crucial the healthcare professional be aware of the fact that physical and psychological issues often overlap. Studies highlight the importance of a multidisciplinary approach that includes the gastroenterologist, the psychologist, the physiotherapist, the nutritionist and sometimes the surgeon to ensure optimal therapeutic management of these patients (Amendola et al., 2003; Nehra, Bruce, Rath-Harvey, Pemberton & Camilleri, 2000; Peppas, Alexiou, Mourtzoukou & Falagas, 2008; Poenaru et al., 1997). This form of management reduces the need for surgery and medication and avoids the abusive use of laxatives, resulting in a good prognosis and ensuring that the individual needs of each child are met (Rogers, 2003). The objective of the present study was to determine the level of knowledge of pediatric medical Residents with respect to functional constipation, evaluating their knowledge on aspects such as diagnosis, possible complications, associated psychosocial aspects and multidisciplinary treatment.
METHOD
Participants
A cross sectional, descriptive study was conducted between October 2010 and January 2011 with a convenience sample consisting of 42 pediatrics residents, from three different public hospitals, referred to here as Hospitals A, B and C, which serve as a reference for training in pediatrics in the city of Salvador, Bahia, Brazil.
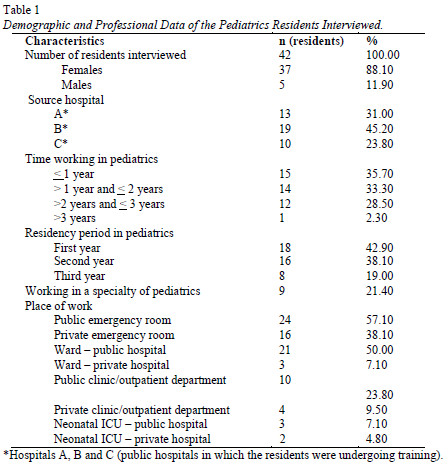
A total 42 medical Residents in pediatrics answered the questionnaire. The majority was female (88.1%), and 21.4% of the Residents were working in some specialty of pediatrics such as neonatology, pediatric neurology or hematology, while 7.1% worked in gastroenterology. The mean age of the Residents was 28.8 ± (SD=2.54) years, with a mean time since graduation of 3.5 years. Overall, 61.9% of the Residents reported having seen an average of 10-50 children and adolescents with constipation (see Table 1).
Materials
A questionnaire was divided into five different domains, including nine objective and 12 subjective questions.
The objective questions approached were the following:
1) Which year of residency are you in? ( ) Residence 1 ( ) Residence 2 ( ) None;
2) Are you working in any specialization? Yes or No
3) Where is your main job? ( ) Outpatients clinics ( ) Ward ( ) Emergency Room ( ) Pediatrics Intensive Care Unit ( ) Neonatal Intensive Care Unit ( ) Private ( ) Public;
4) How many children and adolescents with functional constipation, approximately, have you already seen? ( ) None ( ) Less than 10 ( ) Between 10 and 50 ( ) Between 50 and 100 ( ) More than 100;
5) How long, in the average, does the medical treatment of the functional constipation take? ( ) Until 6 months ( ) Between 6 months and 1 year ( ) 2 years ( ) 3 years ( ) 4 years or more;
6) Does the psyche exert an effect on the neuroendocrine axis in FC? ( ) Yes ( ) No;
7) Whichof the aspects below do you consider to be associated with the intestinal functional constipation? ( ) Stubbornness ( ) Difficulty of the child or adolescent to express aggressiveness ( ) Parents marital crisis ( ) Difficulties at school ( ) Aggression in the family environment ( ) Physical or psychological sexual abuse ( ) Excessive fear ( ) Fathers difficulties in establishing limits ( ) Anxiety ( ) Overly-controlling mother ( ) Depression ( ) Inhibition ( ) Shyness ( ) Difficulty in socializing ( ) Insomnia ( ) Mania;
8) Mark thefactors you think are related to the intestinal functional constipation and their respective frequency, observed in your clinical experience: ( ) strict toilet training ( ) anorexia ( ) bulimia ( ) inadequate diet ( ) family history of constipation ( ) physical or psychological sexual abuse / Frequency: ( ) Almost always ( ) Rarely ( ) Never;
9) When should the doctor recommend psychological treatment for a patient with FC? ( ) Always ( ) Sometimes ( ) Never.
The subjective questions approached the following aspects:
1) How long have you worked in pediatrics?
2) Which pediatrics specialization do you work in?
3) Which are the possible complications resulting from chronic constipation refractory to medical treatment?
4) In a few words, talk about the main factors (environmental, organic and emotional) that may contribute towards triggering FC in children and adolescents.
5) What does the intestinal functional constipation therapeutic treatment consist of?
6) How can the psyche exert an effect on the neuroendocrine axis in FC?
7) When should the toilet training start and how should it be conducted?
8) In your opinion, what is the mothers role in the family?
9) What is the importance of the father in the family?
10) In the question above, why did you state the doctor should ( ) Always, ( ) Sometimes or ( ) Never recommend psychological treatment for a patient with FC?
11) What kind of suffering is important, in the FC, in order to send a patient to the psychologist?
12) Do you think that you need additional information about the questions above? Why?
The domains consisted of: 1) Knowledge and familiarity with the diagnosis of FC and its multifactoriality (clinical and psychological aspects); 2) Concepts regarding maternal and paternal roles, as well as concepts regarding toilet training; 3) The treatment of FC and its multidisciplinary aspects; 4) Referral of the patient with FC for psychotherapy; and 5) The need for further information on the subject.
Procedure
A questionnaire was applied, always by the same investigator, on aspects regarding the residents knowledge on the diagnosis and treatment of FC, psychosocial factors related to FC and the referral of patients with FC for psychotherapy. For the purposes of this study, FC was defined in accordance with the Rome III criteria (Rasquin et al., 2006). Initially, the team of residents was contacted and provided with information on the study through the coordinators of the Pediatrics Departments of each of the three hospitals. Forty-five residents were invited to answer the questionnaire and only three refused to participate. Each resident answered the questionnaire, individually and aloud, in the presence of the researcher, while the investigator herself wrote down each answer. Beforehand, the investigator requested absolute secrecy on what was asked and answered during the application of the questionnaire. This way, the residents, who had not participated yet, would not be influenced by the others opinions.
The data collected were categorized and then analyzed using descriptive measures of frequency and dispersion. The SPSS(Statistical Package for the Social Sciences) software was used throughout the statistical analysis.
The quantitative data were directly analyzed. Some data collected from the subjective answers were, at first, organized with Microsoft Office Excel 2007. Later, they were categorized qualitatively by using the following criteria: the repetition of the most frequent keywords (and its synonymous) present in every residents answer (the manifest content); afterwards, the investigator made inferences to interpret its meanings. It is important to notice that the investigator arranged meetings with two other researchers (a medical student and a psychologist) in order to avoid bias in the interpretation and in the categorizations. The categorization was based on Contents Analysis theory (Bardin, 2010).
This study complies with the ethical principles of the Helsinki declaration and of the Brazilian legislation, and was approved by the Institutional Review Board of the Teaching Hospital, Federal University of Bahia.
RESULTS
According to 45.2% of respondents, the average time required for the medical treatment of FC was between 6 months and 1 year, while 33.3% answered up to 6 months and one resident replied two years. The possible complications resulting from chronic constipation refractory to medical treatment, as mentioned by the respondents, were: pain, hemorrhoids, anal fissure, bowel obstruction and fecaloma (8.1% each), psychological complications and irritability (7.1%).
With respect to the principal factors that may contribute towards triggering FC in children and adolescents, the major environmental factor mentioned by the Residents was diet (95.2%). Among the emotional factors mentioned, 38.0% of respondents referred to emotional factors in the parents, as possible causes of FC in the children. Nevertheless, 23.8% of respondents stated that FC was triggered by emotional factors in the child (see Table 2). The factors mentioned included: anxiety, stress, shyness, social withdrawal, inhibition, insecurity.
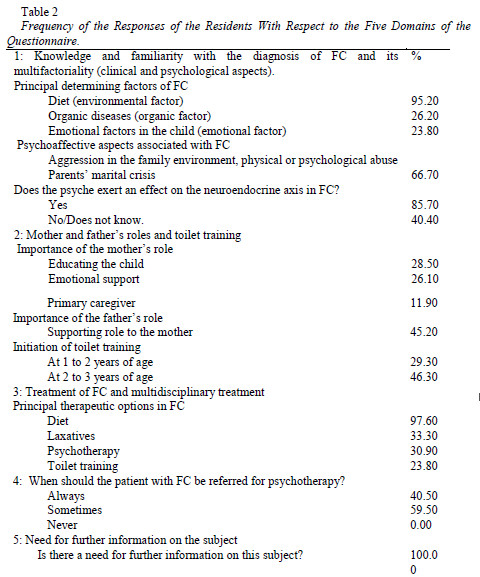

With respect to the psychoaffective aspects associated with FC, almost all the Residents (88.1%) recognized some degree of association between this symptom and family aggression, as well as sexual, physical or psychological abuse (see Table 2).
Half of the Residents (50%) identified childrens difficulties in expressing aggressiveness and 16.7% associated FC with stubbornness in the children and adolescents. More than half of the Residents referred to the presence of fear (78.6%), anxiety (78.6%), depression (57.1%), shyness (69.0%) and a difficulty in socializing (64.3%) in constipated children. Only 19.0% mentioned that FC might be associated with difficulty of the father in establishing limits, whereas 61.9% mentioned an over-controlling mother as being a possible factor in cases of FC (see Table 3).

In response to the question regarding the way in which toilet training should be conducted, 19.0% of the Residents failed to give any answer, merely affirming that at the beginning toilet training should not involve any requirements, i.e. no demands and no chastisement. Others mentioned positive reinforcement and conditioning; 7.1% answered that the child should be instructed to say when he/she wants to go to the bathroom, 19.04% would instruct the child to use the potty and 9.52% suggested toilet training after meals.
With respect to the treatment of FC, 97.6% of the Residents referred to the diet as playing a fundamental role in treatment, albeit in conjunction with other forms of treatment such as laxatives (33.3%), toilet training (23.8%) or psychotherapy (30.9%). Only 7.1% suggested combined treatment (medication and psychotherapy) (see Table 2). The Residents had a vague idea about psychotherapy, with some referring to this form of treatment as being indicated only in severe cases or as support if emotional factors were identified, or with the unique objective of behavioral change. Among these, 11.9% referred the importance of intervening in the family dynamics and of multidisciplinary treatment (2.3%). Only 4.7% of respondents referred to defining the causative factor of FC and the value of doing so for planning the appropriate therapeutic management, and, likewise, only 2.3% suggested disimpaction as part of the treatment.
The respondents were asked to give their opinion on the role of the mother and the importance of the father in the family. With respect to the mother, 28.5% associated this role with educating the child; 11.9% viewed the role of the mother as the childs principal care-giver in the sense of feeding, stimulating and watching for signs of disease in the child. Emotional support as the principal element of the maternal role was mentioned by 26.1% (Table 2). An insignificant number of participants (2.3%) associated the role of the mother with her influence in the father-child relationship, also mentioning an obsessive personality of the mother as a cause of constipation in the child. With respect to the fathers role, 11.9% of respondents believed that he is less important in the childs education than the mother. Approximately half of the Residents (45.2%) believed that the fathers role is similar to that of the mother (see Table 2). Only 2.3% of participants referred to the father as representing an example for the child, while 4.7% referred to him as the head of the family.
In the question regarding when the physician should refer the patient with FC for psychological treatment, only 40.5% of the Residents answered always, while 59.5% answered sometimes (Table 2). When asked to qualify their answers, 59.5% mentioned various conditions for referring patients for psychotherapy: if the physician identified a psychoaffective disorder in the child such as anguish, stress, fear, or anxiety; in cases of abuse; difficulties that prevent the patient from complying with traditional medical treatment. Phrases such as the bowel is an emotional organ and everything that goes through our head is reflected in the bowel were expressed by some of the Residents who stated that they believed it was crucial to refer children and adolescents with FC for psychological therapy; 23.8% of the Residents mentioned the possibility of the failure of medical treatment, in which case they would refer the patient to a psychologist; 11.9% reported that in some cases the psychological aspect is unimportant, and that it is a physical factor or a positive family history of the condition that should be taken into consideration. Nevertheless, in this item of the questionnaire, it was curious to observe that only 16.6% of the Residents mentioned the possibility of multidisciplinary treatment in cases of FC.
On the other hand, in response to the question regarding the type of significant suffering that would justify referral to a psychologist, 76.1% referred psychoaffective disorders such as anxiety and family pressure, the patients aversion to the bathroom, an unbalanced family generating a lack of support, problems/issues in the family environment, separation of parents, abuse, aggression or reprehension by the parents if the child soiled his/her clothing, pain, unsatisfactory domestic and social environment, negligence, resistance to medical treatment, behavior of fecal retention, shyness, fecal soiling, low self-esteem, depression, aggressiveness and irritability. Slightly less than half of the Residents (40.4%) considered difficulties in the family as constituting suffering significant enough to warrant referral for psychotherapy. Physical or psychological abuse was mentioned in this question by 16.6% of the Residents and 7.1% considered that a child with difficulties in socializing represented an important factor for recommending psychotherapy in a patient with FC. Although 23.8% admitted that physical suffering could be a reason for indicating psychotherapy, only 2.3% considered functional constipation in itself to represent a form of suffering. The majority of the Residents (85.7%) agreed that the effect of psychological factors on the neuroendocrine axis could be a determining factor in FC; however, 23.8% gave vague answers, 40.4% stated that they knew nothing about the subject and 9.5% answered incorrectly that there was no association between the two systems or relating the question with hypothyroidism.
With respect to the need for additional information on FC, the respondents unanimously agreed that they did need, and would like to have access to further information on a symptom that is so common in pediatrics outpatient departments and medical offices (see Table 2). Among the Residents who participated in this study, 30.5% reported that they needed more experience and training on this subject, since they had questions regarding several issues. Some of them saw few cases of FC and others focussed more on emergency care rather than outpatient follow-up. They also mentioned that little is discussed about FC and furthermore that their training deals with the subjects in general from a more academic and less practical viewpoint. According to this line of thinking, another 28.5% of the respondents emphasized that investment in knowledge is crucial in obtaining the best possible professional training. Moreover, they affirmed that this is a common topic but that insufficient attention is being given to it. In the words of one respondent: Sometimes we think we know something but in fact we dont know it. Other participants (14.2%) referred to how important it is for the pediatrician to take the psychological factors into consideration in the case of a child with FC in order to provide the family with more appropriate counseling. One of the Residents suggested the inclusion of psychology as part of the undergraduate medical course to make it easier for physicians to help their patients. Despite this reflection, in this final item of the questionnaire, only 4.7% of the Residents mentioned a multidisciplinary approach, while 9.5% referred to the difficulties involved in being able to diagnose and treat cases of FC in children and adolescents more effectively.
DISCUSSION
Functional constipation is a considerably prevalent condition in all age groups; however, in children the condition may become chronic. In the present study, the gaps and contradictions in the Residents knowledge of such a common symptom are striking, particularly with respect to its multifactorial causes (Amendola et al., 2003; Farnam, et al., 2009; Motta et al., 2010; Poenaru et al., 1997; Silva, 2009; van den Berg et al., 2006), as well as the importance of multidisciplinary treatment in cases of FC, as already established in the literature (Altaf & Sood, 2008; Amendola et al., 2003; Nehra et al., 2000; Poenaru et al., 1997). In a systematic review, prevalence rates of constipation in 34 groups of different populations in Europe and Oceania ranged from 0.7% in a pediatric population in Italy to 81.0% in a population of elderly, hospitalized male patients. The majority of cases are functional. Although the specific etiology of FC has yet to be clarified, the following risk factors have been identified: dietary habits, physical inactivity, socioeconomic level, psychological parameters, bowel motility, use of medication, age and gender (Peppas et al., 2008).
The majority of the Residents (95.2%) indicated diet as being a determinant factor in FC. With respect to the treatment, only 7.1% suggested a combination of medication and psychotherapy and 2.3% indicated multidisciplinary treatment. These data regarding the treatment referral highlight the uncertainties of the Residents both with respect to the multifactorial causes of FC and the efficacy of combined, multidisciplinary treatment. FC is known to be a very common idiopathic symptom in children and adolescents (Motta et al., 2010; Rasquin et al., 2006). Nevertheless, 26.6% of the Residents associated the cause of FC with organic diseases and 20% with the individuals bowel rhythm, while 64.2% failed to answer the question. These findings highlight the difficulty of the majority of pediatrics Residents in diagnosing FC, a fundamental step in defining treatment. None, for example, mentioned normal or slow colonic transit as a factor in children with FC (Altaf et al., 2008; van den Berg et al., 2010), showing an obvious need to provide greater in-depth information on these issues.
The clinical complications encountered in chronic cases of FC and those refractory to medical treatment are diverse: recurrent abdominal pain, the presence of blood in feces, urinary infections and urinary retention, enuresis, nausea and vomiting, headache, flatulence, malaise and fecal soiling, in addition to psychological disorders (Nehra et al., 2000; Rogers, 2003). Individuals with functional gastrointestinal disorders (FGID) are at a higher risk of psychological illness and vice-versa (Alander et al., 2005). The percentage of responses regarding the possible complications associated with FC that are in accordance with data published in the literature was low, bearing in mind the importance of the subject: pain, hemorrhoids, anal fissure (mentioned by most), bowel obstruction and fecaloma, psychological complications and irritability. The complications that were not mentioned by any of the participants included urinary infection, and bleeding, as well as the habit of retention with the evacuation of large stools, all of which are associated with functional constipation, and encopresis, which, when added to the scenario, is indicative of the presence of psychological problems (Espinoza, 2002). Indeed, a vicious circle is generally present, the triggering factor of which remains unclear (Mota & Barros, 2008). The importance of understanding this vicious circle involving incomplete evacuation leading to an increased volume of dry feces causing pain at evacuation and resulting in inhibition of sphincter relaxation, thus increasing fecal retention, should be emphasized (Mota & Barros, 2008).
With respect to the Residents knowledge on toilet training, it is feasible to conclude that the majority appears to be aware of the importance of this factor; however, they have only a vague idea of how it should be conducted. It is clear that many of the Residents are still not aware that early toilet training may contribute to the development of FC (Motta et al., 2010; Rasquin et al., 2006; Silva, 2009). Current studies show that inappropriate toilet training is one of the predictive factors for constipation in childhood (Mota & Barros, 2008). Physiological, psychological and sociocultural factors are closely associated in the process of acquiring sphincter control. Over the past 60 years, the strategies involved in toilet training have undergone changes; for example, toilet training is now initiated at a later age (Mota & Barros, 2008). Stressful events such as the birth of a sibling, separation of parents and changes in the home environment are known to hamper sphincter control (Mota & Barros, 2008). Curiously, these aspects may also be associated with functional constipation and encopresis (Martins et al., 1989), emphasizing the need for pediatrics Residents and pediatricians to review their knowledge on the appropriate diagnosis and treatment of FC.
The majority of the Residents were aware of the existence of psychosocial issues in FC. Nevertheless, they perceived these factors more as consequences rather than determinants that could contribute towards triggering this condition. Furthermore, although they demonstrated a certain degree of knowledge regarding the psychoaffective and social issues involved in FC, less than half of the Residents said that they always referred patients with FC for psychotherapy and slightly more than half (59.5%) reported that they did so sometimes. The fact that medical therapy at times fails to achieve the expected results should reinforce the need for reevaluation and psychological and psychiatric treatment; however, physicians seldom indicate these therapeutic options (Espinoza, 2002). Despite parents resistance, physicians should insist on referring the patient for these forms of therapy, since they may result in numerous benefits to the patient (Espinoza, 2002).
The participants of the present study reported that medical treatment resolves the symptoms in six months to two years, but do not know why or how much time they should wait before referring the patient to a multidisciplinary team, perhaps because they were not given this information in their undergraduate course or because they have not been exposed to multidisciplinary teams in their teaching hospitals. Does the patients suffering have to be more intense before multidisciplinary treatment is considered? In the answers given regarding therapy, 30.9% of the Residents mentioned psychotherapy, in addition to having a vague idea about this treatment, which they would only recommend in severe cases or as support therapy. In view of the significant proportion (61.9%) of respondents who admitted that an over-controlling mother could represent a factor in cases of FC, why not refer the patient earlier for psychotherapy? Family aggression, the possessive relationship between the individual in the maternal role and the child, a demanding mother, and the demands of the child for inclusion of the paternal role are some examples of the complexity involved in the diagnosis and treatment of latent psychological aspects in FC (Amendola et al., 2003; Freud, 1905; Grodeck, 1923; Lacan, 1963; Lisboa et al., 2008).
With respect to the roles of the mother and father in the family, the number of clear answers on the subject was minimal. Responses were extremely varied and the percentage representing each opinion was relatively small. In parallel, the Residents did not appear to be clear about the difference between the roles of the mother and father. Only 11.9% of the participants stated that the mother fulfills the more immediate role of primary caregiver, which is in agreement with the literature. The paternal role of representing another possibility of identification for the child, while setting boundaries and testing reality was mentioned vaguely by only 45.2% of the Residents, who referred to the fathers role as being a supportive role to that of the mother. In addition to these data, a further 11.9% of the Residents referred the importance of the father in a supporting role and 7.1% gave evasive answers. Only 9.5% associated the importance of the father in the family with emotional support for the child. These answers reflect the cultural habits of this region in which the majority of the population is unclear about the division of parenteral responsibilities, since childcare remains the exclusive responsibility of the mother in the majority of the cases, while active participation of the father in the childs daily routine is uncommon, particularly in certain socioeconomic strata.
In the question regarding additional aspects associated with FC, the fact that the majority of Residents (88.1%) were aware of the association of sexual, physical and psychological abuse in triggering FC in children and adolescents is noteworthy. However, paradoxically, only 16.6% of the Residents mentioned these factors as constituting significant enough suffering to warrant referral for psychotherapy. Patients with functional gastrointestinal disorders are more likely to report a history of sexual abuse compared to those with gastrointestinal disorders of organic etiology (Drossman et al., 1995).
The participants unanimously admitted the importance and need for additional information on the subject matter of the questionnaire. This confirms that the Residents would like to know more about FC and its latent aspects to enable them to be able to diagnose, treat and refer children and adolescents with FC for multidisciplinary therapeutic management more effectively in the future.
Working in a transdisciplinary team using cooperative intercommunication in favor of collectivity, translating the singularity of the language of each specific area into the construction of scientific knowledge, is an exercise that forms an integral part of the perspective of learning to learn. This movement should begin at undergraduate level to enable physicians to achieve better results in their clinical practice, as well as emphasizing the importance of listening carefully at pediatric consultations to obtain information on the multiple aspects involved in the childs behavior.
This study has some limitations. One of them consists in the fact that the methodology used to collect the data does not allow the investigator to retrieve deeper information from the residents answers. That would be possible, for instance, through open interviews based on a psychoanalytical listening.
The work place and the moment the researcher approached the residents also contributed to limit the study. Those were bias in potential because many residents were interrupted during their meetings and they also had too much work to do. Those facts probably elicited, in some of the respondents, resistence and urgency to answer the questionaire. Another limitation was the fact that the residents knew the investigators profession (a psychoanalist) which may have influenced in their answers about the psychoafective aspects associated to FC and the recommendation to psychotherapy.
Despite the investigator request for confidentiality, this was another uncontrollable variable. The communication among the residents may have occured due to the natural fear and anxiety emerged when facing such an unknown subject.
The results described here highlight the need to conduct more in-depth studies on this subject and to design new protocols. Another limitation refers to the fact that studies with pediatrics Residents from other regions of the country would be necessary in order to determine the level of knowledge of these individuals in different geographical regions, thus allowing more broad-reaching educational programs to be drawn up for this condition that is so common in pediatric practice.
In conclusion, the knowledge of the pediatrics Residents interviewed in this study with respect to FC remains inadequate. The need for relevant and more in-depth information on FC in children and adolescents is crucial and all the Residents recognized this need. The elaboration of continued education programs with a greater emphasis on FC, both at undergraduate level and in medical residency programs, is fundamental since this symptom involves a diverse range of multidisciplinary issues.
REFERENCES
Alander, T., Svärdsudd, K., Johansson, S. E., & Agréus, L. (2005). Psychological illness is commonly associated with functional gastrointestinal disorders and is important to consider during patient consultation: a population-based study. BMC Medicine, 3, 8. doi:10.1186/1741-7015-3-8 [ Links ]
Altaf, M. A., & Sood, M. R. (2008). The nervous system and gastrointestinal function. Developmental Disabilities Research Reviews, 14, 87-95. doi: 10.1002/ddrr.15 [ Links ]
Amendola, S., De Angelis, P., Dalloglio, L., Di Abriola, G. F., & Di Lorenzo, M. (2003). Combined approach to functional constipation in children. Journal of Pediatric Surgery, 38, 819-823. doi:10.1016/jpsu.2003.50174 [ Links ]
Bardin, L. (2010). Análise de Conteúdo (4th ed.). Portugal: Edições 70, Lda. [ Links ]
Burket, R. C., Cox, D. J., Tam, A. P., Ritterband, L., Borowitz, S., Sutphen, J., Kovatchev, B. (2006). Does stubbornness have a role in pediatric constipation? Journal of Developmental & Behavioral Pediatrics, 27, 106-111. [ Links ]
Chattat, R., Bazzocchi, G., Balloni, M., Conti, E., Ercolani, M., Zaccaroni, S., Trombini, G. (1997). Illness behavior, affective disturbance and intestinal transit time in idiopathic constipation. Journal of Psychosomatic Research, 42, 95-100. doi: 10.1016/S0022-3999(96)00217-6 [ Links ]
Drossman, D. A., Talley, N. J., Leserman, J., Olden, K. W., & Barreiro, M. A. (1995). Sexual and physical abuse and gastrointestinal illness. Review and recommendations. Annals of Internal Medicine, 123, 782-794. [ Links ]
Espinoza M., J. (2002). Constipacion in childhood. Revista Chilena de Nutrición, 29, 272-279. doi: 10.4067/S0717-75182002000300001 [ Links ]
Farnam, A., Rafeey, M., Farhang, S., & Khodjastejafari, S. (2009). Functional constipation in children: does maternal personality matter? Italian Journal of Pediatrics, 35, 25-25. doi: 10.1186/1824-7288-35-25 [ Links ]
Freud, S. F.(1905). Três Ensaios sobre a Sexualidade. Obras Completas (2nd ed.). Rio de Janeiro: Imago. [ Links ]
Grodeck, G. (1988). O Livro disso (2nd ed.). São Paulo: Perspectiva. [ Links ]
Lacan, J. (1962-1963). O Seminário. Livro 10. A Angústia (2nd ed.). Rio de Janeiro: Zahar. [ Links ]
Lacan, J. (1957-1958). O Seminário. Livro 5. As Formações do Inconsciente (2nd ed.). Rio de Janeiro: Zahar. [ Links ]
Leroi, A. M., Bernier, C., Watier, A., Hémond, M., Goupil, G., Black, R.,... Devroede, G. (1995). Prevalence of sexual abuse among patients with functional disorders of the lower gastrointestinal tract. International Journal of Colorectal Disease, 10, 200-206. doi: 10.1007/BF00346219 [ Links ]
Lisboa, V. C. A., Felizola, M. C. M., Martins, L. A. N., Tahan, S., Neto, U. F., & de Morais, M. B. (2008). Aggressiveness and hostility in the family environment and chronic constipation in children. Digestive Diseases and Sciences, 53, 2458-2463. doi: 10.1007/s10620-008-0230-1 [ Links ]
Martins, J.L., Petri, M.C.V., Pereira, A.P.A., Fernandes, G.M.M., Silveira, M.L.M, & Pinus, J. (1989). Constipation of phychogenic origin. Pediatria Moderna. 24, 39-42. [ Links ]
Mota, D. M., & Barros, A. J. D. (2008). Toilet training: methods, parenteral expectations and associated disfunctions. Jornal de Pediatria, 84, 9-17. doi:10.2223/JPED.1752 [ Links ]
Motta, C. dos R., Silva, L. R., & Castro, H. de. (2010). A psicanálise da criança – um estudo de caso. Revista de Ciências Médicas e Biológicas, 9, 89-94. [ Links ]
Nehra, V., Bruce, B. K., Rath-Harvey, D. M., Pemberton, J. H., & Camilleri, M. (2000). Psychological disorders in patients with evacuation disorders and constipation in a tertiary practice. The American Journal of Gastroenterology, 95, 1755-1758. doi:10.1111/j.1572-0241.2000.02184.x [ Links ]
Peppas, G., Alexiou, V. G., Mourtzoukou, E., & Falagas, M. E. (2008). Epidemiology of constipation in Europe and Oceania: a systematic review. BMC Gastroenterology, 8, 5. doi: 10.1186/1471-230X-8-5 [ Links ]
Poenaru, D., Roblin, N., Bird, M., Duce, S., Groll, A., Pietak, D.,... Thompson, J. (1997). The Pediatric Bowel Management Clinic: initial results of a multidisciplinary approach to functional constipation in children. Journal of Pediatric Surgery, 32, 843-848. doi: 10.1016/S0022-3468(97)90633-3 [ Links ]
Rasquin, A., Di Lorenzo, C., Forbes, D., Guiraldes, E., Hyams, J. S., Staiano, A., & Walker, L. S. (2006). Childhood functional gastrointestinal disorders: child/adolescent. Gastroenterology, 130, 1527-1537. doi: 10.1053/j.gastro.2005.08.063 [ Links ]
Rogers J. (2003). Management of functional constipation in childhood.British Journal of Community Nursing, 8, 550-553. [ Links ]
Silva, L.R. (2009). Diagnóstico em Pediatria (1st ed.). Rio de Janeiro: Guanabara Koogan. [ Links ]
van den Berg, M. M., Benninga, M. A., & Di Lorenzo, C. (2006). Epidemiology of childhood constipation: a systematic review. The American Journal of Gastroenterology, 101, 2401-2409. doi: 10.1111/j.1572-0241.2006.00771.x [ Links ]
van Dijk, M., Benninga, M. A., Grootenhuis, M. A., & Last, B. F. (2010). Prevalence and associated clinical characteristics of behavior problems in constipated children. Pediatrics, 125, e309-e317. doi: 10.1542/peds.2008-3055 [ Links ]
Recebido em 13 de Setembro de 2012/ Aceite em 13 de Março de 2013













