Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Psicologia
versão impressa ISSN 0874-2049
Psicologia vol.26 no.1 Lisboa 2012
Improving provision of effective psychological care for LGB persons: client perceptions of diversity competences of clinical psychologists and psychotherapists
Como Promover a Qualidade das Intervenções Psicológicas com Pessoas LGB: As percepções dos/as clientes sobre as competências para a diversidade de psicólogos/as clínicos/as e psicoterapeutas
Carla Moleiroa*, Nuno Pintob
aAssistant Professor – Lisbon University Institute – ISCTE‑IUL / CIS
bPhD Student in Psychology – Lisbon University Institute – ISCTE‑IUL / CIS
ABSTRACT
While clinicians are becoming increasingly aware of the need to be competent in terms of cultural and individual diversity, European professional associations have made little progress in establishing guidelines and standards of care, practice and training – contrary to their North American counterparts. The purpose of the present paper is to contribute to the recognition of clinician diversity competences as viewed by LGB clients. It further aims to describe the perceptions that these clients have of these competences, in terms of their dimensions, illustrations, and their presence/absence in actual clinical practice. The present study utilizes a qualitative methodological approach, involving the use of 3 focus groups with 15 LGB persons. A focus group plan was developed and focus groups were conducted in a non‑clinical setting, after recruitment through LGBT associations. Content analysis was conducted on the transcripts of the focus groups. Results included similar proportions of units of analysis in the dimensions of awareness (31%), knowledge (37%) and skills (32%). Clinician LGB awareness, however, was evaluated as more central in relation to the other two dimensions; and, overall, perceptions of competences actually present in clinical practice only made up 6% of units of analysis. The results argue for the foundational role of clinicians LGB diversity competences when working with sexually diverse individuals.
Keywords: LGBT; diversity; diversity competence; psychotherapy
RESUMO
Apesar do facto de ser cada vez mais reconhecida a necessidade dos/as psicólogos/as clínicos/as e psicoterapeutas serem competentes em termos da diversidade individual e cultural, as organizações profissionais Europeias ainda não desenvolveram guidelines e standards para a prática e a formação nesta área – contrariamente ao que acontece na América do Norte. O objectivo deste artigo é contribuir para o reconhecimento das competências clínicas para a diversidade na perspectiva dos próprios clientes LGB. Pretende ainda descrever as percepções que estes clientes têm destas competências, em termos das suas dimensões, ilustrações, e a sua presença/ausência na prática clínica. O estudo utiliza uma metodologia qualitativa, envolvendo a participação de 15 pessoas LGB em 3 grupos de discussão focalizada. Foi desenvolvido um plano para os grupos de discussão focalizada, que decorreram em contexto não‑clínico, após recrutamento junto de associações comunitárias LGBT. A análise de conteúdo foi realizada com base nas transcrições dos grupos. Os resultados revelaram uma proporção semelhante de unidades de análise nas dimensões de consciência (31%), conhecimento (37%) e competências práticas (32%). A consciência LGB foi, ainda assim, avaliada como mais central do que as restantes duas dimensões; e, de um modo geral, as competências avaliadas como presentes actualmente na prática clínica foram apenas 6% das unidades de análise. Os resultados alertam para o papel fundamental das competências clínicas para a diversidade LGB.
Palavras‑chave: LGBT; diversidade; competências para a diversidade; psicoterapia
Introduction
In an increasingly diverse world, psychologists and other mental health professionals have recognized that clinicians need to be able to work with people who are culturally different from themselves (La Roche & Christopher, 2010). These differences include those related to values and behaviours based on age, gender, sexual orientation, gender identity, ethnic origin, colour, language, religion, socio‑economic level, and (dis)ability status. However, it is indisputable that most psychological treatments have been historically rooted in theories that were not sensitive to that diversity. For those reasons, a recent focus has been given to the promotion of individual and cultural diversity competences among clinical psychologists and psychotherapists (Daniel, Roysircar, Abeles & Boyd, 2004). This focus developed from the initial contributions of the multicultural counselling literature (e.g. Sue, Arredondo & Davis, 1992) and their extension to work with other minorities, such as lesbian, gay and bisexual (LGB) clients (Israel & Selvidge, 2003). At present, internationally, the need for culturally responsive treatments is increasingly acknowledged, although there is still great debate regarding its relevance and process.
In fact, in the case of sexual orientation, it was not until the early 1970s that homosexuality ceased to be conceptualized as a psychopathology by the American Psychiatric Association and even later by the World Health Organization. Recent reports still evidence that there are therapies (and therapists) aimed toward changing the sexual orientation of non‑heterosexual clients, even though they are widely questioned, both ethically and scientifically (American Psychological Association, 2009; Bartlett, Smith & King, 2009; Haldeman, 2002).
The growing empirical and clinical literature on LGB issues has been mostly invisible in mainstream psychology (Goldfried, 2001). However, in the last two decades a number of researchers and clinicians have dedicated themselves to furthering our understanding in such areas as life development among LGB individuals, determinants of well‑being and risk factors for mental and physical health, parenting/family and couple relationships, among others. This research has uncovered some elevated risk for stress‑sensitive disorders among LGB persons (Cochran, Sullivan & Mays, 2003; Meyer, 2003), such as suicide, substance abuse, and affective and anxiety disorders (e.g. PTSD). A critical role is attributed to the social stigma surrounding homosexuality itself, experiences of social inequalities, and incidents of discrimination and victimization (Cochran, 2001). The specificities of the experiences and mental health issues of this population have led some (e.g. APA, 2009; Eubanks‑Carter, Burckell & Goldfried, 2005) to argue for the need to train clinical psychologists and psychotherapists in working affirmatively with LGB clients, including therapist self‑awareness of their own (even if subtle) biases toward homosexuality and specific areas of knowledge and skills these clinicians need to be familiar with (Pachankis & Goldfried, 2004).
Israel and Selvidge (2003) extended the expertise regarding multicultural counselling (e.g. Sue et al., 1992) in order to conceptualize clinicians competence with LGB clients – building a broader vision of clinical individual and cultural diversity competences. As in multicultural competence, this model asserts that a psychotherapist competent in working with LGB clients should have appropriate knowledge, attitudes and skills. Firstly, the knowledge component of multicultural competence is intended to bring the psychotherapists up to date with unfamiliar cultures or groups. In the case of LGB competence, Israel and Selvidge (2003) propose that mental health practitioners should be knowledgeable about issues such as socio‑political history, biases in assessment and mental health services, diversity within groups, LGB identity development, the coming out process, LGB parenting and family structures, family of origin concerns, among others. Secondly, the multicultural counselling literature emphasizes the importance of psychotherapists exploring their own stereotypes and prejudices about minority populations. Awareness of the cultural background of the client and its impact on presenting concerns is perceived as essential, as well as awareness of the role of the clinicians values and attitudes in the development of the therapeutic relationship. Israel and Selvidge (2003) propose that clinicians develop an awareness of their reactions to LGB clients (attitudes and values, homophobia, stereotypes), and seek training and supervision in order to demonstrate sensitivity to sexual diversity. Thirdly, these authors exemplify some of the skills that an LGB competent psychotherapist can demonstrate. These include being able to recognize when sexual orientation should be part of the focus of clinical attention (and when it should not); to tailor his or her interventions to the clients sexual identity development; to educate his or her clients about internalized homophobia; to be familiar with resources of social support within the LGB community in order to provide information on them to his or her clients; to advocate for LGB clients by disseminating accurate information through research and outreach; among others.
While clinicians are becoming increasingly aware of the need to be competent in terms of cultural and individual diversity, European professional associations have made little progress in establishing guidelines and standards of care, practice and training – contrary to their North American counterparts. In February 2000, a joint task force of members of the Committee on Lesbian, Gay, and Bisexual Concerns and the Division 44 of the APA developed a set of guidelines for Psychotherapy with Lesbian, Gay and Bisexual Clients (2000). These guidelines were adopted by APA the same year and intended to guide both graduate student training and clinical practice in their clinical work with LGB clients. These guidelines were updated in 2011 (APA, 2011), which also followed a report with recommendations on appropriate therapeutic responses to sexual orientation (APA, 2009). Training program accreditation guidelines in North American also mandate adequate preparation of clinicians in work with a variety of minority groups. Finally, a project was initiated by Marvin Goldfried (see Goldfried, 2001), who developed a network called AFFIRM: Psychologists Affirming their Lesbian, Gay, Bisexual, and Transgender Family. This network has been involved in efforts to incorporate LGB issues into mainstream psychology.
No similar efforts have been made by European Associations. While a few countries (e.g. UK; see King, Semlyen, Killaspy, et al., 2007) have national criteria and guidelines, these constitute a limited number, and only a small percentage of psychotherapists actually have training in LGB diversity sensitivity. Furthermore, there are new trends in client and family diversity resulting from recent legislature in a few European countries on LGB issues (e.g. civil marriages in countries such as the Netherlands, UK, Spain and Portugal; adoption rights in the UK or Spain). Thus, while the European Diploma for Psychology and the European Federation of Psychotherapy Associations do not specify training requirements in this area, European individual and family psychotherapists are faced with sexually diverse clients, regardless of their level of training in working with LGB clients and their families.
The purpose of the present paper is to contribute to the recognition of clinician LGB diversity competences, in particular from the perspective of LGB clients. To date, few studies have taken this client‑centered approach (Burckell & Goldfried, 2006), when in fact clients experiences and understanding may constitute an important (even indispensable) source of information in identifying not only their needs, but also the experienced barriers in the care that is provided to them. This perspective may be perceived in line with a community empowerment approach, which involves providing the opportunity for the voices of minority groups to emerge and be heard (Hur, 2006). It also argues, along with other authors (e.g. Minas, 2007; Vandrevala, Willis & John, 2007), for the involvement of service users in health care planning and delivery.
Hence, this study aims to describe the perceptions that these clients have of the LGB diversity competences required of mental health clinicians (particularly, clinical psychologists and psychotherapists), in terms of their basic dimensions, including some illustrations of particular competences, and their presence/absence in actual clinical practice. Ultimately, it aims to encourage the future development of standards of care for improving provision of effective treatment for LGB persons within Europe, where mobility of both clients and clinicians is increasing among countries with a variety of political, social and family contexts for these clients.
Method
Study Design
The present study utilizes a qualitative methodological approach, involving the use of focus groups (Krueger & Casey, 2000) with LGB persons. A focus group plan was developed and focus groups were conducted in a non‑clinical setting, after recruitment through LGBT associations. Confidentiality and anonymity of the participants was guaranteed, as well as voluntary participation (APA, 2002; Ordem dos Psicólogos Portugueses, 2011).
Sample
The sample included 15 persons who participated in one of 3 focus groups – 6 women and 9 men, with a mean age of 29.7 years old. Most identified as gay (n=8) or as lesbian (n=5), with only a few identifying as bisexual (n=2). With regards to sexual behaviours and relationships (see Kinsey Homosexuality Scale; Kinsey, Pomeroy & Martin, 1948), all males except one (n=8) endorsed exclusively homosexual, while female participants (lesbian and bisexual) varied in their endorsements from exclusively homosexual to predominantly homosexual, only incidentally heterosexual and equally homosexual and heterosexual. All but one participant held a college degree, and some had masters or PhD diplomas (n=5). No participants identified as transgender, or as a member of an ethnic minority in Portugal. Nine (60%) participants had previously sought psychotherapy for help with LGB‑related issues.
The composition of the groups varied. The first group was conducted with gay males, and was composed of 7 participants. The second group was composed of lesbians, in which 4 women participated. Finally, a heterogeneous group was assembled, with 4 participants (2 males and 2 females), who identified as gay, lesbian or bisexual. This choice for group composition was intentional and aimed to ensure both more homogenous groups (Groups 1 and 2) and a group which could allow for the contrasting of possibly diverse opinions (Krueger & Casey, 2000). While we aimed to ensure the presence of 6 to 8 participants in each group, as recommended by Krueger and Casey (2000), recruitment of participants for this topic and population was more challenging than expected, and hence Groups 2 and 3 did not reach the expected size.
Instruments
A semi‑structured plan was developed for conducting the focus groups, which were led by the junior researcher and an independent PhD student. The group was asked to build a list of 1‑8 items of relevant competences for clinicians working with LGB clients (key question; Krueger & Casey, 2000). In order to build up to that group task, transition questions were asked regarding: (1) experienced difficulties and challenges regarding identity as LGB (What were some of the problems or challenges you faced or experienced as a lesbian/gay/bisexual person?); (2) resources and coping strategies utilized, at an individual, familial, social and/or community level (What were some of the resources and strategies you used to face those difficulties?); and (3) experiences and/or expectations regarding seeking help from clinical psychologists or psychotherapists (e.g. As one of those resources, did you ever seek help from a psychologist or psychotherapist? If so, what was your experience in terms of the way he/she was able to handle your concerns as a LGB person?). Opening and concluding questions (Krueger & Casey, 2000) were also included to help people feel comfortable and to verify the adequacy of the summary of the discussion, respectively.
Data Analysis
The data collected were subjected to content analysis (Bauer, 2000), with the support of MaxQDA 10 software. The approach utilized a blended model, incorporating features of thematic content analysis (see Morant, 2006) and also Consensual Qualitative Research (Hill, Thompson & Williams, 1997; Hill, Knox, Thompson, Williams & Hess, 2005), since it most adequately fit the goals and methodology of the study. Initial content domains were established based on a three‑dimensional model of the conceptualization of LGB competence (Israel & Selvidge, 2003). Analysis was guided by the a priori study objectives to investigate the dimensions of LGB diversity competences of clinicians that participants identified, whilst also allowing unanticipated themes in the data to shape the analysis and categories. Thus, initially the data were grouped into the categories knowledge, awareness, and skills. Subsequently, sub‑categories were generated using open coding. Firstly, two coders worked independently on the data, and final categories were reached in a second step by the team of researchers who made decisions on the data by consensus, following Hill and colleagues (1997; 2005). For the present paper, the corpus of analysis consisted of both (1) the lists of 1‑8 items of relevant competences for clinicians working with LGB clients made by the 3 groups; and (b) the discourse of participants during the discussions regarding the construction of the lists. These two text materials were analysed separately, even though their interpretation was integrated in the discussion of the overall results.
Results
The lists of relevant LGB clinical competences created by each of the three focus groups accounted for a total of 24 units of analysis, distributed relatively equally in the categories awareness, knowledge and skills. The knowledge domain accounted for a total of 9 items. Specific examples of knowledge were provided, namely, a competent psychotherapist should have information about homosexuality, [such as] the difficulties faced by lesbians, or they must know that there are various forms of homophobia, whether physical, verbal, psychological. From the point of view of these participants, psychotherapists should, in addition, know LGBT Associations and include LGBT issues in their basic training. A total of 8 units were assigned to the content domain of awareness. This dimension was expressed, for example, as being sensitive to differences, not being homophobic or being aware of own limits and refer [clients] to colleagues when necessary. Finally, essential clinical skills were identified, in a total of 7 units. Those included skills within the therapeutic relationship (such as being able to work on internalized homophobia and adapt to different family contexts), but also outside of it (such as the use of LGBT associations as resources or be a change agent in their workplace).
In addition, the discourse of participants during the discussions and the responses regarding psychotherapist qualities preferred in working with LGB clients were also analysed. Again, data was categorised according the three‑dimensional model of LGB competences. A total of 68 units of analysis were coded, with a relatively even distribution among the 3 categories: 25 segments fit the knowledge dimension, 22 the skills dimension and 21 were related to the awareness dimension. These discursive segments included participants perceptions of the presence or absence of some particular competence in the actual work of therapists with LGB clients. Thus, 3 sub‑categories were created for each initial dimension: (a) neutral formulation, when the discursive segment did not indicate the perception of the presence or absence of the particular competence; (b) presence, when the discursive segment revealed the participants perception of its habitual presence in actual practice; and (c) absence, when the discursive segment revealed the participants perception of its usual absence in real clinical practice. All units of analysis, as categorised under the three initial domains, were also analysed according to these three sub‑categories (see Table 1).
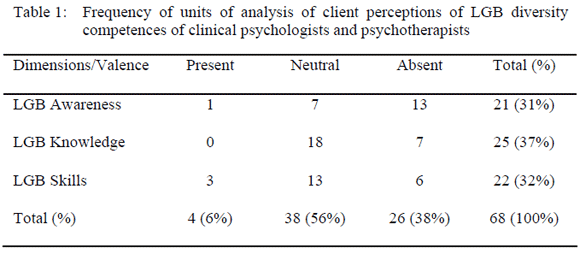
With regards to clinicians LGB knowledge, participants discourse was mostly neutral. Indeed, 18 of the 25 units of analysis referring to LGB knowledge did not reveal the perception of their presence or absence in the provision of care from actual clinical psychologists and psychotherapists. An illustration was that [LGB] information is important, not only for them [clinicians] but also to transmit to the patient. On the other hand, 7 of the 25 units of analysis were formulated in terms of their absence, showing the perception of the lack of specific LGB knowledge. For example, [clinical] psychologists and all health professionals have little information in these specific issues. No units of analysis related to knowledge were formulated in such a way as to indicate the perception of their regular presence among clinicians.
In relation to the segments referring to the clinicians awareness, 13 of the 21 were categorized as absent, indicating that this dimension was perceived as mostly missing. A participant, for instance, reported that a homophobic person can actually practice psychology [...]. A psychologist can, thus, have a profound influence on many negative experiences of others, and another stated I believe many psychotherapists are not [prepared to work with LGB clients], I believe that many [...] are homophobic, are completely outdated in relation to LGBT relationships. Still in relation to awareness, 7 units of analysis were formulated in a neutral way. For example, one participant said that psychologists must know their prejudices and if they are able to work with this issue. Only 1 segment revealed a participants perception of the presence of this dimension, making reference to the awareness required to recognize the need to refer cases to colleagues who may be more prepared (If you are [a psychologist and] homophobic, and if you are seeing a homosexual patient, you refer them to another [psychologist]).
Finally, the majority of the discursive units referring to the skills that a LGB‑competent psychotherapist can demonstrate were formulated in a neutral form, accounting for 13 of 22 units of analysis (for instance: to be an agent of change within their professional group). Moreover, 6 segments were illustrated and perceived as generally absent (most psychologists do not make an assessment of the community resources, such as ILGA and other associations, and do not use it in their work) and 3 segments revealed the participants perception of the presence of specific skills of clinicians working with LGB clients. An example of the latter was provided by a participant, who stated that the issue of the personal coming out is always taken into account.
Additional main themes related to experienced difficulties of LGB persons included internalized homophobia, challenges of coming out, non‑acceptance of family and peers, discrimination experiences in specific contexts (such as the workplace, or living in rural areas), specific challenges of gay men, of lesbians, of bisexual identities, and religious conflicts with sexual orientation. Common coping strategies and resources included peer support, family support, LGB peer groups, web resources, and volunteer involvement in the LGB community.
Discussion
The present paper aimed to contribute to the recognition of clinician diversity competences, and their dimensions, by exploring client perceptions of clinicians LGB diversity competences. Our findings suggest that client‑identified competences may fit the 3‑dimensional model of individual and cultural diversity competences – awareness, knowledge and skills – posited by previous literature (Sue et al., 1992; Israel & Selvidge, 2003). With regards to clinician competences, the relevance of clinician self‑awareness, as well as awareness of LGB issues, was perceived as fundamental. These dimensions were, nonetheless, evaluated as mostly lacking in light of actual experiences and perceptions of clinical psychologists and psychotherapists in Portugal. In fact, only a few competences were perceived as existent or mostly present, in any of the three dimensions – awareness, knowledge and skills. This seems consistent with the invisibility of this population and its issues among training programs in our country, which contrasts with the training requirements in other countries in North America and Europe.
The meaning of these results seems to be translated into a paradox. While participants may recognize and value the use of psychotherapy as a resource for coping and may idealize the clinician as impartial and non‑homophobic, they also realize that few (if any) health professionals have systematic training, knowledge and skills in this area. This finding is consistent with those found by other authors regarding the expectations and help‑seeking behaviours of ethnic minorities and migrants (Moleiro, Silva, Rodrigues & Borges, 2009). This paradox may be a risk factor for early drop‑out from treatment, which is a particular concern among minority group members, given their increased exposure to minority stress and experiences of prejudice and discrimination (Meyer, 2003). Additionally, it further supports the need for the development of both national and European guidelines to help systematize the competences necessary to work with the LGB population.
Our findings also suggest that clients experiences and perspective can be a rich source of information in identifying therapist preferred qualities, as suggested by Burckell and Goldfried (2006). This provides support to others (Minas, 2007; Vandrevala, Willis & John, 2007) that have argued for the involvement of service users in health care planning and delivery.
While we recognize the contributions of this study, we also acknowledge some limitations, in particular related to the small size of the sample and its non‑representativeness. Furthermore, qualitative analysis was conducted by the authors, and not by independent raters or judges. Notwithstanding, and in conclusion, this paper defends the foundational role of clinician LGB diversity competences when working with diverse individuals.
References
American Psychological Association [Division 44/Committee on Lesbian, Gay, and Bisexual Conce
American Psychological Association (2002). Ethical principles of psychologists and code of conduct. American Psychologist, 57(12), 1060‑1073. [ Links ]
American Psychological Association (2009). Report of the American Psychological Association Task Force on Appropriate Therapeutic Responses to Sexual Orientation. Washington, DC: Author. [ Links ]
American Psychological Association (2011). Practice guidelines for LGB clients: guidelines for psychological practice with lesbian, gay, and bisexual clients. American Psychological Association. Retrieved January, 15, 2011, from www.apa.org/pi/lgbt/resources/guidelines.aspx. [ Links ]
Bartlett, A., Smith, G., & King, M. (2009). The response of mental health professionals to clients seeking help to change or redirect same‑sex sexual orientation. BioMed Central Psychiatry, 9(11). Available from: www.biomedcentral.com/1471‑244X/9/11 [ Links ]
Bauer, M. (2000). Classic content analysis: A review. In M. Bauer & G. Gaskell (Eds.), Qualitative researching with text, image and sound: A practical handbook (pp. 131‑151). London: Sage Publications. [ Links ]
Burckell, L.A., & Goldfried, M.R. (2006). Therapist qualities preferred by sexual minorities. Psychotherapy Theory, Research, Practice and Training, 43, 32‑49. [ Links ]
Cochran, S.D. (2001). Emerging issues in research on lesbians and gay mens mental health: Does sexual orientation really matter? American Psychologist, 56, 931‑947. [ Links ]
Cochran, S.D, Sullivan, J.G., & Mays, V.M. (2003). Prevalence of Mental Disorders, Psychological Distress, and Mental Health Services among Lesbian, Gay, and Bisexual Adults in the United States. Journal of Counseling and Clinical Psycholog, 71(1), 53‑61. [ Links ]
Daniel, J.H, Roysircar, G., Abeles, N., & Boyd, C. (2004). Individual and cultural‑diversity competency: Focus on the therapist. Journal of Clinical Psychology, 60(7), 755-770. [ Links ]
Eubanks‑Carter, C.F., Burckell, L.A., & Goldfried, M.R. (2005). Enhancing therapeutic effectiveness with lesbian, gay, and bisexual clients. Clinical Psychology: Science and Practice, 12, 1‑18. [ Links ]
Glaser, B. G., & Strauss, A. L. (1967). The Discovery of Grounded Theory: Strategies for Qualitative Research. New York: Aldine Publishing Company. [ Links ]
Goldfried, M.R. (2001). Integrating lesbian, gay, and bisexual issues into mainstream psychology. American Psychologist, 56, 977-988. [ Links ]
Haldeman, D.C. (2002). Gay rights, patient rights: The implications of sexual orientation conversion therapy. Professional Psychology: Research and Practice, 33, 260-264. [ Links ]
Hill, C., Knox, S., Thompson, B.J., Williams, E.N., Hess, S.A., & Ladany, N. (2005). Consensual qualitative research: An update Journal of Counseling Psycology, 52(2), 196-205. [ Links ]
Hill, C. E., Thompson, B.J., & Williams, E.N. (1997). A guide to conducting consensual qualitative research. The Counseling Psychologist, 25, 517‑572. [ Links ]
Hur, M. H. (2006) Empowerment in terms of theoretical perspectives: exploring a typology of the process and components across disciplines. Journal of Community Psychology 34(5) 523-40. [ Links ]
Israel, T., & Selvidge, M. (2003). Contributions of Multicultural Counseling to Counselor Competence with Lesbian, Gay, and Bisexual Clients. Journal of Multicultural Counseling and Development, 31, 84‑98. [ Links ]
King, M., Semlyen, J., Killaspy, H., Nazareth, I., & Osborn, D. (2007). A systematic review of research on counselling and psychotherapy for lesbian, gay, bisexual & transgender people. British Association for Counselling & Psychotherapy. London: BACP. [ Links ]
Kinsey, A.C., Pomeroy, W.B., & Martin, C.E. (1948). Sexual behavior in the human male. Philadelphia: W.B. Saunders. [ Links ]
Krueger, R., & Casey, M. (2000). Focus Groups: A Practical Guide for Applied Research (3rd ed.). CA, USA: Sage Publications.
La Roche, M.J., & Christopher, M.S. (2010). Cultural Competences. In J. C. Thomas & M. Hersen (Eds.), Handbook of Clinical Psychology Competencies (Vol. 1; pp. 95‑122). New York, NY: Springer.
Meyer, I.H. (2003). Prejudice, social stress, and mental health in lesbian, gay, and bisexual populations: Conceptual issues and research evidence. Psychological Bulletin, 129, 674-697. [ Links ]
Minas, H. (2007). Developing mental‑health services for multicultural societies. In: D Bhugra & K Bhui (Eds), Textbook of Cultural Psychiatry. Cambridge, UK: Cambridge University Press. [ Links ]
Morant, N. (2006). Social representations and professional knowledge: the representation of mental illness among mental health practitioners. British Journal of Social Psychology, 45, 817‑838. [ Links ]
Ordem dos Psicólogos Portugueses (2011). Código Deontológico. Regulamento n.º 258/2011, Diário da República, 258, 17931‑17936. [ Links ]
Pachankis, J.E., & Goldfried, M.R. (2004). Clinical issues in working with lesbian, gay, and bisexual clients. Psychotherapy: Theory, Research, Practice, and Training, 41, 227-246. [ Links ]
Sue, D.W., Arredondo, P.A., & Davis, R.J. (1992) Multicultural counseling competencies and standards: A Call to the profession. Journal of Multicultural Counseling and Development, 20, 64‑88. [ Links ]
Vandrevala, M.H., Willis, J., & John, M. (2007). A move towards a culture of involvement: involving service users and carers in the selection of future clinical psychologists. The Journal of Mental Health Training, Education and Practice, 2(3), 34‑43. [ Links ]
Carla Moleiro, ISCTE‑IUL, Psychology Department, Avenida das Forças Armadas, 1649‑026 Lisbon – Portugal. Phone: +351.21.7903216
E-mail: carla.moleiro@iscte.pt













