Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Jornal Português de Gastrenterologia
versão impressa ISSN 0872-8178
J Port Gastrenterol. vol.21 no.3 Lisboa jun. 2014
https://doi.org/10.1016/j.jpg.2014.01.006
ENDOSCOPIC SPOT
Esophagitis dissecans superficialis
Esofagite dissecante superficial
Pedro Cardoso Figueiredob,∗, Pedro Pinto-Marquesa, Jorge O. Netab, João Freitasa
a Serviço de Gastrenterologia, Hospital Garcia de Orta, Almada, Portugal
b Serviço de Anatomia Patológica, Hospital Garcia de Orta, Almada, Portugal
*Corresponding author
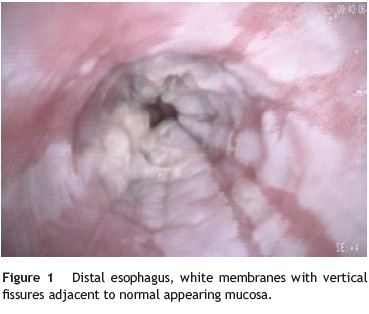
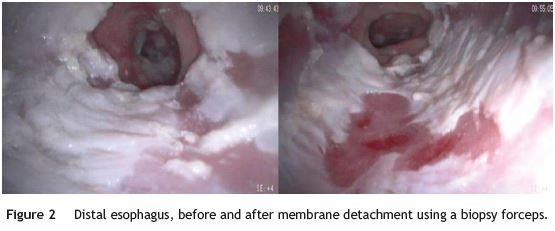
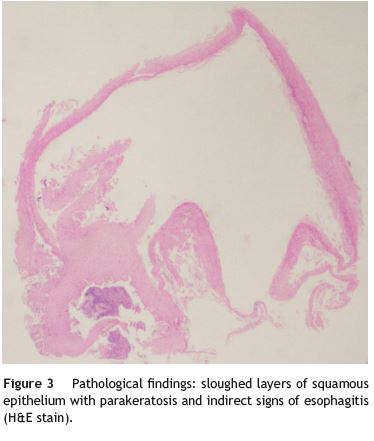
58-year-old woman was referred to our Gastroenterology Clinic for long-lasting history of heartburn, chest pain and regurgitation. Her past medical history was notable for major depressive disorder and essential hypertension. She was under pantoprazole qd, valsartan and hydrochlorothiazide. During the two previous years, she had been submitted to two upper digestive endoscopies which described a severe reflux esophagitis and a papyraceous esophagus in the lower third of the esophagus. In the absence of clinical response the pantoprazole dose was increased. She stopped the antihypertensive drug and started limiting her diet to mashed food. As symptoms progressed to mixed (solid and liquid) dysphagia and odynophagia we performed an upper digestive endoscopy. It revealed white membranes with vertical fissures adjacent to normal appearing mucosa in the distal esophagus (Fig. 1). These membranes were easily detached and exposed a normal appearing mucosa (Fig. 2). Biopsies showed mild chronic esophagitis, sloughed layers of squamous epithelium with parakeratosis and no microorganisms, namely fungi (Fig. 3). Correlating the endoscopic and histologic findings the diagnosis made was esophagitis dissecans superficialis (EDS).
EDS was first described in 1892 and it is a rare, probably under-recognized and underreported, entity.1,2 It has been associated with drinking hot beverages, medications (bisphosphonates and nonsteroidal anti-inflammatory drugs), heavy smoking, achalasia, skin conditions (prurigo nodularis and bullous dermatoses), esophageal iatrogenic injury (variceal sclerotherapy and band ligation, esophageal dilation and mediastinal radiation for lung cancer), celiac disease, immunosuppression and impaired mobility.2-4 Nevertheless, EDS has been found in the absence of obvious predisposing conditions, as was the case in our patient.2 The pathogenesis remains unknown: some argue it represents a common reaction of esophageal squamous mucosa to various types of insult (physical, chemical, thermal and immunological) while others hypothesize it is a topical allergic response (although no sensitizing antigens have yet been proposed).2,3 Patients complain of dysphagia, odynophagia and reflux symptoms or may be asymptomatic. Endoscopic findings, as described above, are similar to those found in Candida esophagitis which might lead to misdiagnoses.4 The literature suggests that in many cases EDS is a benign condition and that mucosal healing can be obtained through combination of acid suppression and discontinuation of precipitating medications.2 When associated to bullous dermatoses, EDS treatment also includes steroids.5 Our patient had persistent symptoms despite high doses of pantoprazole and on a repeat endoscopy she maintained the esophageal findings. She was switched to rabeprazole with a lack of benefit and, ultimately, she refused further tests and abandoned follow-up.
This report aims to raise awareness to this often forgotten and misdiagnosed entity. Of note, this was the first of the two cases diagnosed by a single operator during a 2-year period. Only with the improvement of detection of EDS we might increase our knowledge of this peculiar condition and treat patients who do not respond to acid suppression.
References
1. Rosenberg B. Oesophagitis dissecans superficialis. Centralbl Allg Pathol Path Anat. 1892;3:753-9. [ Links ]
2. Carmack SW, Vemulapalli R, Spechler SJ, Genta RM. Esophagitis dissecans superficialis (sloughing esophagitis): a clinicopathologic study of 12 cases. Am J Surg Pathol. 2009;33:1789-94. [ Links ]
3. Lin DE, Vanagunas A. Esophagitis dissecans superficialis: a case series. Am J Gastroenterol. 2000;95:2426. [ Links ]
4. Purdy JK, Appelman HD, McKenna BJ. Sloughing esophagitis is associated with chronic debilitation and medications that injure the esophageal mucosa. Mod Pathol. 2012;25:767-75. [ Links ]
5. Hokama A, Yamamoto Y, Taira K, Nakamura M, Kobashigawa C, Nakamoto M, et al. Esophagitis dissecans superficialis and autoimmune bullous dermatoses: a review. World J Gastrointest Endosc. 2010;2:252-6. [ Links ]
Ethical disclosures
Protection of human and animal subjects. The authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of data. The authors declare that no patient data appear in this article.
Right to privacy and informed consent. The authors declare that no patient data appear in this article.
Conflicts of interest
The authors have no conflicts of interest to declare.
*Corresponding author
E-mail address: pedro.c.figueiredo@hotmail.com (P. Cardoso Figueiredo).
Received 23 October 2013; accepted 19 January 2014













