Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Jornal Português de Gastrenterologia
versão impressa ISSN 0872-8178
J Port Gastrenterol. vol.19 no.2 Lisboa fev. 2012
Gummatous hepatic syphilis simulating malignancy
Sífilis hepática simulando metastização hepática
Bruno Arroja,a,* Isabel Cotrim,a Martinha Henriqueb
aDepartment of Gastroenterology, Hospital de Santo André, EPE, Leiria, Portugal
bDepartment of Dermatology and Venereology, Hospital de Santo André, EPE, Leiria, Portugal
*Corresponding author
KEYWORDS Hepatic gummas; Tertiary syphillis; Granulos
PALAVRAS-CHAVE Gomas hepáticos; Sífilis terciária; Granulomas
Case description
A 67 year‑old female was observed in our gastroenterology department with a history of weight loss (10% total weight) during the previous year, malaise and anorexia. She denied fever and gastrointestinal symptoms. She was a divorced house wife living in a rural area in Portugal. She did not take any kind of medication and had no previous history of infectious diseases whatsoever.
On physical examination she appeared pale. The abdómen was tender and slightly painful on deep palpation of the right upper quadrant. A tender hepatomegaly with irregular borders was palpable two centimeters below the right costal margin.
Blood analysis revealed: haemoblogin 10.5 g/dL (11.5‑15.5), leucocytes 6 100/mL (5000‑13 000), platelets 310 000/mL (150 000‑400 000), INR 1.02, C‑reactive protein 102 mg/L (0‑5), erythrocyte sedimentation rate 109 mm, aspartate aminotransaminase 57 U/L (<31), alanine aminotransaminase 47 U/L (<34), gamma‑glutamyltransferase (GGT) 300 U/L (<38), alkaline phosphatase 950 U/L (40‑150), total bilirubin 1.2 mg/dL (0.3‑1.2), albumin 3.5 g/dL (3.5‑5.2).
Ultrasonography showed multifocal hypoechoic hepatic nodules suggestive of malignancy and a normal spleen.
A more thorough laboratory work‑up yielded negative serologies for the following viruses: HAV, HBV, HCV, HIV, EBV, CMV, HSV 1 and 2. Wright reaction and Venereal Disease Research Laboratory (VDRL) were non reactive; tuberculin test was negative; alpha‑fetoprotein was normal.
The computed tomography (CT) scan showed an enlarged and heterogeneous liver with bosselated borders and multiple hypodense nodular lesions suggesting primary liver malignancy or secondary metastasis (Figs. 1A and 1B). The largest lesion was seen in the right hepatic lobe measuring 5.5 centimeters. Histological analysis after nodule biopsy showed an infl ammatory infi ltrate, multiple granulomas with hepatocellular necrosis and rare multinucleated giant cells (Fig. 2). There were no signs consistent with malignancy.
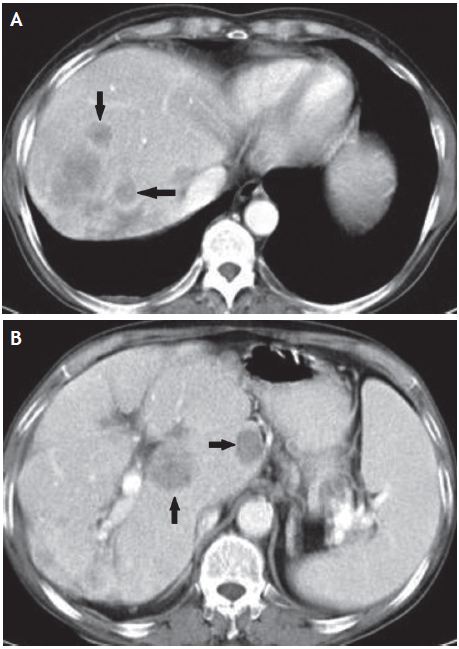
Figures 1A and 1B Multiple hypodense nodular lesions (black arrows) in both lobes of the liver seen on CT‑scan.
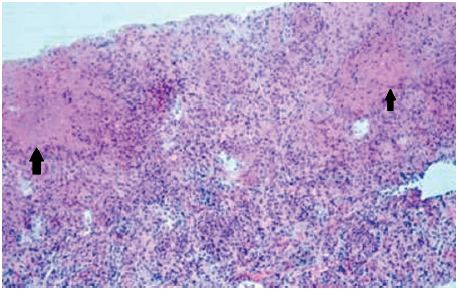
Figure 2 Biopsy specimen (hematoxylin & eosin) showing hepatic granulomas with central necrosis (black arrows).
Repeat VDRL plus treponemal tests added new data: VDRL 1280 dils, TPHA 1/20480, FTA‑ABS + with positive IgM.
Neurosyphilis was ruled out after lumbar puncture.
Antibiotic therapy was started with penicillin G 2.4 million units IM once weekly for three weeks, with excellent clinical improvement. Six months after treatment, serum VDRL titer was 128 dils and alkaline phosphatise/GGT levels were normal. A follow‑up CT‑scan one year later did not show any remaining hepatic nodular lesions (Fig. 3).
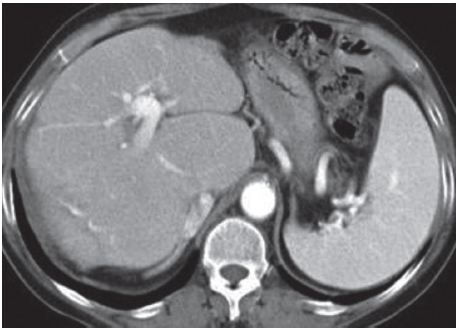
Figure 3 CT‑scan demonstrates liver healing one year after successful treatment.
In the antibiotic era, tertiary syphilis is a very rare disease.1,2
Gummas are the hallmark of tertiary syphilis and can affect the skin, bones or internal organs.2,3
Gummata in the liver are typically multiple and scattered through both hepatic lobes, simulating malignant lesions.2,3 Identification of bacteria in late syphilis necrosis occurs in 0 to 5% of all cases.3
Non‑treponemal tests like VDRL lose diagnostic power (sensitivity ranging from 37‑94%) in tertiary syphilis and measured alone can give rise to false negative results.4 For this reason, it is essential to obtain a highly accurate treponemal test such as FTA‑Abs (Fluorescent Treponemal Antibody Test) or TPHA (Treponema pallidum hemagglutination assay) early during the investigation if suspicion of syphilis is strong.4,5
Favourable response to treatment is monitored with a decrease in VDRL titer of at least four‑fold, over a period of six to twelve months.1,2
References
1. Avelleira JCR, Bottino G. Sífilis: diagnóstico, tratamento e controle. An Bras Dermatol. 2006;81:111‑26. [ Links ]
2. Rampal P, Veyres B, Agrati D, et al. Les atteintes hepátiques de la syphilis. Ann Gastroentérol Hépatol. 1986;22:77‑81. [ Links ]
3. Maincent G, Labadie H, Fabre M, et al. Tertiary hepatic syphilis: a treatable cause of multinodular liver. Dig Dis Sci. 1997;42:447‑50. [ Links ]
4. Young H. Syphilis. Serology. Dermatol Clin. 1998;16:691‑8. [ Links ]
5. Larsen SA, Steiner BM, Rudolph AH. Laboratory diagnosis and interpretation of tests for syphilis. Clin Microbiol Rev. 1995;8:1‑21. [ Links ]
Funding
The authors did not receive any financial support for the purposes of this article.
Conflicts of interest
The authors do not have any conflicts of interest to disclose
*Corresponding author
E-mail address: brunoarroja@gmail.com (B. Arroja).
Received January 11, 2011; accepted February 19, 2011













