Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Nascer e Crescer
versão impressa ISSN 0872-0754versão On-line ISSN 2183-9417
Nascer e Crescer vol.28 no.1 Porto mar. 2019
https://doi.org/10.25753/BirthGrowthMJ.v28.i1.12891
WHAT IS YOUR DIAGNOSIS? | QUAL O SEU DIAGNÓSTICO?
Imaging clinical case
Caso imagiológico
Joana Brandão SilvaI, Mafalda SantosII
I Pediatrics Department, Unidade 2. Centro Hospitalar Vila Nova de Gaia/Espinho. 4400-129 Vila Nova de Gaia, Portugal. joanarbsilva0@gmail.com
II Pediatric Orthopedics Department, Unidade 2. Centro Hospitalar Vila Nova de Gaia/Espinho. 4400-129 Vila Nova de Gaia, Portugal. mafalda.orto@gmail.com
Endereço para correspondência | Dirección para correspondencia | Correspondence
ABSTRACT
A ten-year-old soccer practitioner female presented with right anterior knee pain lasting one month and exacerbated by running, with no constitutional symptoms or recent trauma. Physical examination revealed pain on the inferior pole of the patella and infrapatellar swelling.
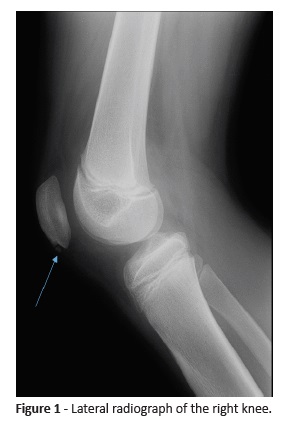
Lateral radiography of the right knee revealed fragmentation of the lower pole of the patella. These findings are suggestive of Sinding- Larsen-Johansson syndrome, an osteochondrosis that affects the extensor mechanism of the knee and is a self-limited condition. The patient was treated with analgesics, rest, and abstention from sports activity during four weeks, with progressive improvement.
Keywords: knee; overuse injury; Sinding-Larsen-Johansson syndrome
RESUMO
Uma adolescente de dez anos, jogadora de futebol, foi observada no Serviço de Urgência por gonalgia direita com evolução de um mês e agravamento com a corrida, sem história de trauma ou outra sintomatologia associada. Ao exame físico, apresentava dor à palpação do pólo inferior da rótula e edema discreto infra-rotuliano. A radiografia do joelho revelou fragmentação do pólo inferior da rótula. Estes achados são compatíveis com o Síndrome de Sinding- Larsen-Johansson, uma osteocondrose que afeta o mecanismo extensor do joelho, geralmente auto-limitada. A doente foi tratada com analgesia, repouso e evicção de exercício físico durante quatro semanas, com melhoria progressiva.
Palavras-chave: lesão de sobrecarga; joelho; Síndrome de Sinding- Larsen-Johansson
A ten-year-old soccer practitioner female presented with right anterior knee pain, lasting one month and exacerbated by running. She denied recent trauma, fever, night pain, or other symptoms.
On physical examination, the girl experienced pain on palpation of the lower pole of the patella, with mild infrapatellar edema and no other associated inflammatory signs, limited joint mobility, or lameness. A lateral radiograph of the knee was performed, showing fragmentation of the inferior pole of the patella (Figure 1).
What is your diagnosis?
Diagnosis
Sinding-Larsen-Johansson syndrome
Discussion
Sinding-Larsen-Johansson syndrome (SLJS) was described for the first time in 1921 and is an osteochondrosis affecting the extensor mechanism of the knee, similarly to Osgood-Schlatter disease. SLJS is a rare syndrome, with incidence of radiographic abnormalities of the inferior pole of the patella reported to be low (2−5%) in healthy adolescents. It typically occurs between 10 and 14 years of age, but most often in males who play sports that involve running and jumping.1-3
There is no consensus on the etiology of this syndrome, with apophysitis, periostitis, tendinitis, or osteochondritis suggested as underlying mechanisms.2 The repetitive traction by the patellar tendon on the lower pole of the patella (partly cartilaginous in adolescents) during contraction of the quadriceps muscle may lead to cartilage damage, swelling, and pain (particularly after exercise), with subsequent tendon thickening and fragmentation of the lower pole of the patella.1
Athletes present with pain located in the lower pole of the patella and proximal attachment of the patellar tendon (exacerbated during flexion), infrapatellar edema, and functional limitation.1,4
Although this is a clinical diagnosis, radiography can be performed to exclude differential diagnoses when presentation is atypical.2,5 Radiologically, four stages of the disease have been described by Medlar: stage 1, normal findings; stage 2, irregular calcifications at the inferior pole of the patella; stage 3, coalescence of the calcification; stage 4A, incorporation of the calcification into the patella to yield a normal radiographic configuration of the area; and stage 4B, a coalesced calcification mass separated from the patella. Other complementary diagnostic tools, such as ultrasound or even magnetic resonance imaging (MRI), may evidence all manifestations of this syndrome.2
The differential diagnosis is important because treatment depends on the type of injury. Sleeve fracture is one type of lesion for which differential diagnosis with SLJS is important. The avulsion of a small bony fragment from the distal pole of the patella, together with a sleeve of articular cartilage and periosteum, results from a major trauma, as opposed to SLJS that results from overuse. In sleeve fracture, pain is usually more severe and with sudden onset, and active extension of the knee is difficult, especially with resistance.2 In the present case, presentation with pain of gradual onset lasting one month and exacerbated by running, absence of trauma, typical age, and the considered sports (soccer) suggest SLJS diagnosis. The localized tenderness and radiographic evidence of fragmentation of the inferior pole of the patella corroborate this diagnosis.
Treatment is conservative, and rest and avoiding physical activity is advised for at least one to two months, especially in the case of activities involving significant pressure on the quadriceps femoris muscle. Pain disappears when the patella is completely ossified, although it may persist for 12 to 18 months in some cases. Acute painful episodes respond well to decreased activity, local ice massage, and short-term use of non-steroidal anti-inflammatory drugs.1,2
In this case, the adolescent was treated with analgesia whenever necessary and advised to rest for four weeks, with subsequent restart of physical activity as tolerated.
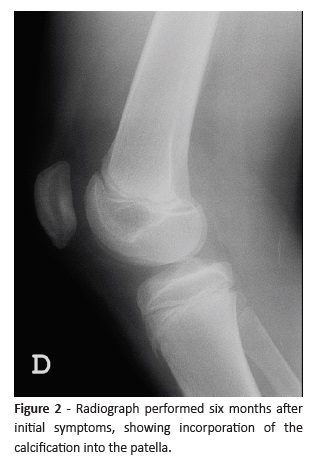
Symptoms rapidly regressed and after six months the patient was fully recovered. Radiographic assessment at the time revealed incorporation of the calcification into the patella (Figure 2).
REFERENCES
1. Valentino M, Quiligotti C, Ruggirello M. Sinding-Larsen- Johansson syndrome : A case report. J Ultrasound. 2012; 15:127-9. [ Links ]
2. Iwamoto J, Takeda T, Sato Y, Matsumoto H. Radiographic abnormalities of the inferior pole of the patella in juvenile athletes. Keio J Med. 2009; 58:50-3. [ Links ]
3. López-Alameda S, Alonso-Benavente A, López-Ruiz A, Miragaya- López P, Alonso-Del Olmo JA, González-Herranz P. Enfermedad de Sinding-Larsen-Johansson: análisis de factores asociados. Rev Esp Cir Ortop Traumatol. 2012; 56:354-60. [ Links ]
4. Patel DR, Villalobos A. Evaluation and management of knee pain in young athletes: overuse injuries of the knee. Transl Pediatr. 2017; 6:190-8. [ Links ]
5. Jaramillo D, Bancroft L, Varich L, Logsdon G. Imaging of Sports-related Injuries of the Lower Extremity in Pediatric. Radiographics. 2016;:1807-27. [ Links ]
Endereço para correspondência | Dirección para correspondencia | Correspondence
Joana Brandão Silva
Pediatrics Department
Unidade 2
Centro Hospitalar Vila Nova de Gaia/Espinho
Rua Francisco Sá Carneiro, s/n
4400-129 Vila Nova de Gaia
Email: joanarbsilva0@gmail.com
Received for publication: 29.12.2017
Accepted in revised form: 24.04.2018