Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Nascer e Crescer
versão impressa ISSN 0872-0754versão On-line ISSN 2183-9417
Nascer e Crescer vol.28 no.1 Porto mar. 2019
https://doi.org/10.25753/BirthGrowthMJ.v28.i1.13020
WHAT IS YOUR DIAGNOSIS? | QUAL O SEU DIAGNÓSTICO?
Dermatology clinical case
Caso clínico dermatológico
Carolina BaptistaI, Maria Adriana RangelI, Carlos NeivaI, Jorge RomarizII, Fátima PraçaII, Herculano CostaII, Cláudia PedrosaII
I Pediatrics Department, Unidade 2. Centro Hospitalar Vila Nova de Gaia/Espinho. 4400-129 Vila Nova de Gaia, Portugal. carolina.baptista@gmail.com; mariaadrianarangel@hotmail.com; cjneiva@gmail.com
II Immunoallergology and Pediatric Pulmonology Unit, Pediatrics Department, Unidade 2. Centro Hospitalar Vila Nova de Gaia/Espinho. 4400-129 Vila Nova de Gaia, Portugal. jaromariz@gmail.com; fatimapraca@sapo.pt; herculano.costa@hotmail.com; claudia.pedrosa@gmail.com
Endereço para correspondência | Dirección para correspondencia | Correspondence
ABSTRACT
Allergic contact dermatitis (ACD) is a delayed hypersensitivity reaction. ACD’s incidence increases with age and rarely presents in the first year of life. Diagnosis of ACD is suspected based on a detailed history and physical examination and confirmed with patch testing. Avoidance of allergen(s) involved is essential for symptom control. The authors present a case of ACD associated with multiple allergens manifesting in the first year of life which resolved with avoidance measures.
Keywords: allergic contact dermatitis; infancy; nickel; cobalt; potassium dichromate
RESUMO
A dermatite de contacto alérgica (DCA) é uma reação de hipersensibilidade tardia. A incidência de DCA aumenta com a idade e raramente se manifesta no primeiro ano de vida. Uma anamnese detalhada, associada ao exame físico, permite estabelecer uma hipótese diagnóstica, que é confirmada pelas provas de sensibilidade cutânea (testes de contacto patch). A evicção do(s) alergénio(s) envolvido(s) é crucial para o controlo sintomático.
Os autores apresentam um caso de DCA associada a múltiplos alergénios, manifestada no primeiro ano de vida, e que resolveu com medidas de evicção.
Palavras-chave: dermatite de contacto alérgica; lactente; níquel, cobalto, dicromato de potássio
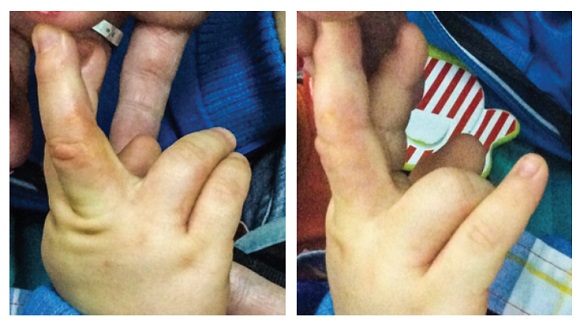
A previously healthy ten-month-old male was referred to the Pediatric Immunoallergology Department due to pruritic skin lesions on the hands over the past two months. The infant usually played with rusty keys. He presented with dermatitis of the intertriginous areas of the hands with papules and vesiculation. Emollients, topical steroids, and avoiding key contact were recommended. On follow-up consultation, the infant remained symptomatic and was submitted to skin prick tests (Atopy Patch Test) with the European Baseline Series.
What is the diagnosis?
Diagnoses
Allergic Contact Dermatitis (ACD) to metals
The infant had a local reaction and eruptions on the wrist and perioral region, and diagnosis was confirmed by Patch Test that tested positive to nickel, cobalt, and potassium dichromate.
After family education and information about sources of involved allergens, dermatitis resolved, and the child remained asymptomatic.
Discussion
ACD is a delayed hypersensitivity reaction triggered by direct skin contact with the allergen or by its ingestion.1,2 It is histologically characterized by an inflammatory reaction with intraepidermal intercellular edema and monocyte and histiocyte infiltration of the dermis.3
In pediatric patients, incidence of ACD increases with age, with few reported cases of ACD in the first year of life.4-6 However, sensitization to allergens may begin at an early age.1,4,7-9
In children, the most common allergens causing ACD include metals, fragrances, preservatives, and p-tert-butylphenol- formaldehyde resin.4 Most frequently involved metals (nickel, cobalt, and potassium dichromate) are found on jewelry, coins, keys, and costume accessories, but also in cosmetic products, foods (oatmeal, beans, chocolate…), electronic devises (mobile phones, tablets, computers…), and orthopedic and orthodontic equipments.3
Several factors are associated with risk of ACD: genetic predisposition, frequency, concentration, and duration of contact with the allergen, skin-barrier disruption, and contact with corrosive metal with increasing hapten release.10-12
On the acute phase, ACD presents with a localized erythematous dermatitis with pruritus, edema, papules, and vesicles. Chronic ACD presents with erythema, desquamation, fissuring, lichenification, and excoriations. Typical ACD appears in areas that were in contact with the allergen, but it can also present as symmetrical drug-related intertriginous and flexural exanthema or on previous sites of atopic dermatitis.3,9,13,12
Clinically, localized ACD involving the hands can mimic acute palmoplantar eczema (APE), also known as dyshidrotic eczema or pompholyx. APE is a pruritic, vesicular eruption of the palms, soles, or both. Lesion distribution is generally bilateral and symmetrical. The etiology of APE is unknown, and management involves general skin care measures and application of moderate to potent topical corticosteroids. Topical ointments of tacrolimus 0.1% or aluminum chloride 12−20% and phototherapy with narrow band ultraviolet B or high doses of UVA1 light have also been used in some cases.12 Diagnosis of ACD and identification of involved allergen(s) is crucial for improving child’s quality of life and may have an impact on child’s future career. The gold standard for diagnosis is patch testing.1,2,4 Treatment consists on avoidance measures, oral antihistamines, steroids (topical or oral), and skin barrier protection. Phototherapy, immunomodulatory, and anti-inflammatory agents may be necessary in refractory ACD.3,10
With this report, the authors intend to demonstrate that, although the incidence of ACD increases with age, some children may have disease manifestations within the first months of life. Diagnosis of APE was initially considered, but symptoms did not resolve until implementation of contact avoidance measures with metals identified in the Patch Test. A detailed history, physical examination, and follow-up visits are essential for diagnosis.
REFERENCES
1. Simonsen AB, Deleuran M, Johansen JD, Sommerlund M. Contact allergy and allergic contact dermatitis in children - a review of current data. 2011; 8:254-65. DOI: 10.1111/j.1600-0536.2011.01963.x.
2. Mortz CG, Kjaer HF, Eller E, Osterballe M, Norberg LA, Høst A, et al. Positive nickel patch tests in infants are of low clinical relevance and rarely reproducible. 2013; 24:84-7. DOI: 10.1111/pai.12027.
3. Tuchman M, Silverberg JI, Jacob SE, Silverberg N. Nickel contact dermatitis in children. Clin Dermatol. 2015; 33:320-6. DOI: 10.1016/j.clindermatol.2014.12.008. [ Links ]
5. de Waard-van der Spek FB, Andersen KE, Darsow U, Mortz CG, Orton D, Worm M, et al. Allergic contact dermatitis in children: which factors are relevant? (review of the literature). Pediatr Allergy Immunol. 2013; 24:321-9. DOI: 10.1111/pai.12043.
6. Gonçalo S, Gonçalo M, Azenha A, Barros MA, Sousa Bastos A, Brandato FM, et al. Allergic Contact Dermatitis in Children. Contact Dermatitis. 1992; 26:112-5.
7. Smith VM, Clark SM, Wilkinson M. Allergic contact dermatitis in children : trends in allergens , 10 years on . A retrospective study of 500 children tested between 2005 and 2014 in one UK centre. 2015; 3:37-43. DOI: 10.1111/cod.12489.
8. Fortina AB, Romano I, Peserico A. Contact sensitization in very young children. J Am Dermatology. 2011;65(4):772-779. DOI: 10.1016/j.jaad.2010.07.030.
9. Silverberg NB, Licht J, Friedler S, Sethi S, Laude TA. Nickel Contact Hypersensitivity in Children. 2002; 19:110-3.
10. Goldenberg A, Silverberg N, Silverberg JI, Treat J. Pediatric Allergic Contact Dermatitis : Lessons for Better Care. J Allergy Clin Immunol Pract. 2017;3:661-7. DOI: 10.1016/j.jaip.2015.02.007.
11. Torres F, Graças M. Management of contact dermatitis due to nickel allergy : an update. 2009:39-48.
12. Thyssen JP. Nickel and Cobalt Allergy befire and after nickel regulation - evalution of a public health intervention. Contact Dermatitis. 2011; 65:1-68. DOI: 10.1111/j.1600-0536.2011.01957.x.
13. Paller AS, Mancini AJ. Hurwitz’s Clinical Pediatric Dermatology: A Textbook of Skin Disorders of Childhood and Adolescence. 4th ed. Elsevier; 2011.
14. Yoshihisa Y, Shimizu T. Metal Allergy and Systemic Contact Dermatitis : An Overview. Dermatol Res Pract. 2012; 2012:749561. DOI: 10.1155/2012/749561.
Endereço para correspondência | Dirección para correspondencia | Correspondence
Carolina Baptista
Pediatrics Department
Unidade 2
Centro Hospitalar Vila Nova de Gaia/ Espinho
Rua Francisco Sá Carneiro, s/n
4400-129 Vila Nova de Gaia
Email: carolina.baptista@gmail.com
Received for publication: 06.09.2017
Accepted in revised form: 16.10.2017