Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Portuguese Journal of Nephrology & Hypertension
versão impressa ISSN 0872-0169
Port J Nephrol Hypert vol.29 no.3 Lisboa set. 2015
ORIGINAL ARTICLE
Pregnancy in renal transplanted patients: effects on the mother and the newborn – 29 years of experience in a single centre
Gravidez em doentes transplantadas renais: efeitos sobre a mãe e o recém-nascido – 29 anos de experiência num único centro
Cristina Cândido1, Márcio Viegas1, Patrícia Matias2, Rita Birne2, Cristina Jorge2, André Weigert2, Teresa Adragão2, Margarida Bruges2, Domingos Machado2
1 Nephrologyy Department,Centro Hospitalar de Setúbal, Setúbal, Portugal
2 Nephrology Department, Centro Hospitalar de Lisboa Ocidental, Lisboa, Portugal.
ABSTRACT
Background: Chronic kidney disease causes decreased fertility. With kidney transplantation, fertility is restored within a few months. Objective: To analyse the feasibility of pregnancy with renal transplantation and its impact on renal function, complications in women and newborns. Methods: Retrospective study of pregnancies that occurred in kidney transplant recipients between 1985 and 2014 in one Transplantation Unit, with a follow-up of 12 months post-partum. Results: Eighteen pregnancies were included (one twin pregnancy) in 13 kidney transplant recipients with an average age of 31 years. Of these, 12 pregnancies progressed, five resulted in miscarriage and one in abortion. Only one pregnancy was complicated by gestational diabetes. There were two stillbirths (twin pregnancy). The average weight of 11 newborns was 2.6 kilograms. There was a significant decrease of estimated glomerular filtration rate at 3 months post-partum [p < 0.05], but a year after delivery, the tendency was not maintained [p > 0.05]. Regarding proteinuria, the significant rise at 3 months was maintained until one year [p <0.05]. A significant increase in blood pressure was observed only on the 3rd trimester [p < 0.05], which did not maintain a year after delivery [p > 0.05]. In patients taking cyclosporine, a decrease in serum levels [p < 0.05] was found throughout the pregnancy. No rejection was detected, as well as graft failure during pregnancy or post-partum follow-up. Conclusion: Although the sample is limited, the number of miscarriages was higher than in the general population (24% versus 8 to 20%). The significant increase of the proteinuria throughout a year suggests a long-term increased risk of graft dysfunction. The decrease in serum cyclosporine levels during pregnancy implies a tighter monitoring of this parameter throughout this period.
Key-Words:Fertility; kidney transplantation; pregnancy.
RESUMO
Introducão: A doença renal crónica provoca a diminuição da fertilidade. Com a transplantação renal a ferti- lidade é recuperada em poucos meses. Objetivo: Analisar a viabilidade da gravidez no transplante renal e o seu impacto sobre a função renal, as complicações na mulher e no recém-nascido. Métodos: Estudo retro- spectivo das gravidezes ocorridas em transplantadas renais entre 1985 e 2014 numa Unidade de Transplantação, com um follow-up de 12 meses pós gravidez. Resultados: Foram incluídas 18 gravidezes (1 gravidez gemelar) em 13 transplantadas renais com uma média de idades de 31 anos. Destas, 12 gravidezes progrediram, 5 resultaram em aborto espontâneo e 1 em aborto induzido. Apenas uma gravidez se complicou por diabetes gestacional. Ocorreram dois nados-mortos (gravidez gemelar). O peso médio dos 11 recém-nascidos foi de 2,6 kg. Verificou-se uma diminuição significativa da taxa de filtração glomerular estimada aos 3 meses pós parto [p < 0.05], mas 1 ano pós parto a tendência deixou de ser significativa [p> 0.05]. Relativamente à proteinuria, o aumento significativo aos 3 meses pós parto manteve-se aos 12 meses [p < 0.05]. No 3o trimestre verificou-se um aumento significativo da tensão arterial [p < 0.05], que não se manteve aos 12 meses pós parto [p > 0.05]. Nos doentes sob ciclosporina verificou-se uma diminuição dos níveis séricos [p < 0.05] ao longo da gravidez. Não se detetou nenhuma rejeição assim como falência do enxerto durante a gravidez ou no follow-up pós parto. Conclusão: Embora a amostra seja limitada, o número de abortos espontâneos foi superior ao da população geral (24% versus 8 a 20%). O aumento significativo da proteinuria mantido após um ano sugere o aumento do risco de disfunção do enxerto a longo prazo. A diminuição dos níveis séricos de ciclosporina ao longo da gravidez implica uma vigilância mais apertada deste parâmetro neste período.
Palavras-Chave: Fertilidade; gravidez; transplante renal.
INTRODUCTION
Chronic kidney disease (CKD) in women can cause decreased fertility. Loss of libido can occur, as well as anovulatory vaginal bleeding or amenorrhoea and high prolactin levels1. In dialysis, conception is rare and occurs at a rate of no more than one in every 200 patients2. A kidney transplant rapidly restores the ability to conceive within a few months3 and to many women it is the opportunity to realize the dream of motherhood. In the first ages of renal transplantation pregnancy was contraindicated, however, the first offspring of a renal transplanted woman was born 48 years ago and, since then, the concepts have progressively changed, so that nowadays it is considered that pregnancy is just another positive aspect of kidney transplantation4.
Women are usually advised to wait at least 1 year after living related donor transplantation and 2 years after cadaver transplantation5. Beyond that, some considerations must be taken into account: if the patient has adequate and stable graft function, if she is at low risk for opportunistic infections, if she is not taking teratogenic medications or medication contraindicated in pregnancy, as mycophenolate mofetil and mammalian target of rapamycin (mTOR) inhibitors, then, pregnancy can be attempted only one year after transplantation without concern of increased risks. A longer waiting period may be advised if there have been recent episodes of acute graft rejection or if the serum creatinine is >,1.5 mg/ dl5. However, waiting 5 or more years may result in impaired renal function post-partum that fails to recover mainly because of gradually deteriorating renal function secondary to chronic rejection6. Beyond these considerations, little is known about the feasibility of pregnancy in renal transplantation and its impact on renal function, as well as complications in women and newborns. This study sought to address this knowledge gap.
METHODS
A restrospective observational study was carried out analysing 18 pregnancies that occurred in 13 kidney transplanted patients, between 1985 and 2014, in the Transplantation Unit of the Centro Hospitalar Lisboa Ocidental. The collected data was obtained by consulting medical records involving the preconception period, during each trimester of pregnancy and follow-up at 3 and 12 months after delivery.
Demographic data was evaluated, such as maternal age, ethnic group, aetiology of chronic kidney disease, type of donor and interval from transplantation to pregnancy. The immunosuppression taken before and during pregnancy was analysed. Different variables related to renal allograft were analysed during the months of pregnancy and after childbirth: kidney function, proteinuria, blood pressure, doses and levels of tacrolimus and cyclosporine, as well as other variables related to the pregnancy outcome (live birth, stillbirth, miscarriage and abortion), obstetric complications, delivery outcome (induced delivery or Caesarean section), newborn outcome (gestational age and birth weight, and congenital anomaly). The results are expressed as means, with the standard deviation (SD) and median, with interquartile range between brackets, when applying to continuous variables. Categorical variables are expressed as frequencies. The mean glomerular filtration rate was estimated by the CKD EPI equation. Nonetheless, taking into account that Creatinine-based formulas developed in non-pregnant populations are likely to be inaccurate when applied to pregnant women, it was only performed statistical analysis comparing the baseline eGFR (before pregnancy) with the post-partum period. Statistical evalu- ation of the results was performed using the paired t-test or Wilcoxon test in conformance with normality of the samples distribution, confirmed by the DAgostino-Pearson test.
RESULTS Patients characteristics
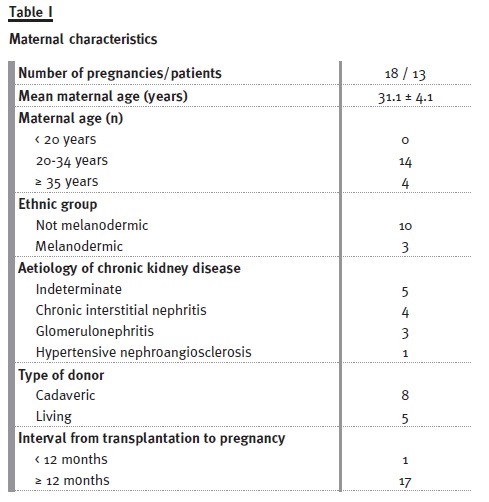
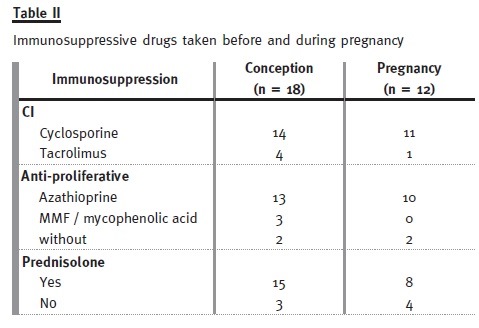
Eighteen pregnancies in 13 kidney transplant recipients (KTRs) were included, but only twelve progressed (one twin pregnancy). The average age was 31.1 ± 4.1 years and the mean duration of gestation was 36 ± 2.5 weeks. The immunosuppression regimen was variable, but in all pregnancies, at conception, patients were under 1 calcineurin inhibitor (CI); in 16 pregnancies the patients were under one anti-proliferative and in 15 pregnancies they were taking prednisolone. The characteristics of these KTRs are described in Table I and immunosuppression taken before and during pregnancy are described in Table II.
Pregnancy events and neonatal outcomes
Twelve pregnancies progressed (11 under cyclosporine); 5 (24%) resulted in miscarriage, all in the 1st trimester of pregnancy (3 under cyclosporine, azathioprine and prednisolone and 2 under tacrolimus, mycophenolate mofetil and prednisolone); one abortion (maternal wish). Only one pregnancy was complicated by gestational diabetes. Most deliveries were induced and submitted to Caesarean section.
As an average, the induced deliveries were carried out at 36.3 ± 2.5 weeks of gestation and only 3 of those (38%) were preterm. The Caesarean section was performed on average at 35.7 ± 2.5 weeks, 4 of those (40%) were preterm. Due to a lack of collected data, a clear reason for inducing delivery and/or Caesarean section was not found in the majority of cases.
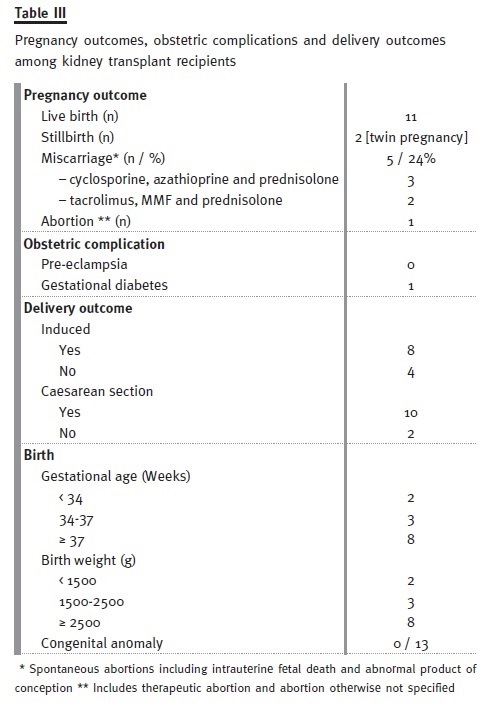
There were 2 stillbirths (twin pregnancy), thus resulting in a total of 11 newborns with a median weight of 2.88 Kg (2.21 – 3.03). All were born healthy, 8 of which at 37 or more weeks of gestation. Only 3 newborns (23%) presented low weight for the gestational age (< percentile 10). Pregnancy, obstetric complications and delivery outcomes among kidney transplant recipients are reported in Table III.
Allograft function
Regarding the estimated glomerular filtration rate (eGFR), in spite of an initial increase, there was a significant decrease between baseline and follow-up at 3 months post-partum [p < 0.05], but a year after delivery this tendency was not maintained [p > 0.05]. In the preconception period only 3 patients had proteinuria, all with values below 300 mg/24h. During pregnancy, there was worsening or development of proteinuria higher than 300 mg/24 h in 8 cases (67%), with a maximum value registered in the 3rd trimester [p < 0.05]. One year after childbirth, eight patients had proteinuria and the tendency was maintained [p < 0.05] (three under mTOR inhibitor and five under CNIs).
During pregnancy there was a significant increase in blood pressure (BP) only on the 3rd trimester [p <0.05]. A year after delivery there was no significant increase in BP relative to baseline [p > 0.05].
In patients taking cyclosporine, a progressive fall in serum levels was observed with minimum value on the 3rd trimester [p < 0.05], with the need of dose adjustment in four cases. No cases of acute rejection or graft failure during pregnancy or post-partum follow-up were registered. The mean value of the eGFR and proteinuria, and the median value of BP and cyclosporine levels are described in Table IV and illustrated in Figs. 1 and 2.
DISCUSSION
Although the sample is limited, data suggests that the risk of miscarriages among women with kidney transplants is higher compared to the general population (24% versus 8 to 20%)7,8 and may suggest that the interference of immunosuppressive agents can occur. Presently, there is limited information regarding the toxicities and teratogenic potentials of immunosuppressive drugs in pregnancy and it is still not clear what is the best immunosuppression regimen that should be followed. Most patients were under triple immunosuppressive therapy: cyclosporine, azathioprine and prednisolone. As for cyclosporine, the main calcineurin inhibitors used in this study population, there are conflicting reports on the transfer of cyclosporin across the human placenta6. Data showed that administration of cyclosporine was associated with low birth weights and a higher incidence of maternal diabetes, hyperten- sion and renal allograft dysfunction. The decrease in serum levels of cyclosporine observed in this study during pregnancy can be justified by the increase of both metabolism and volume of distribution in this period. Higher doses may be required to maintain plasma levels in the therapeutic range9. Some have suggested that pregnancy is an immu- nosuppressed state10.It is true that pregnant women are always a risk group for worse prognosis in epidemic diseases and it is also real that they do not reject the foetus, but a pronounced deal of evidence shows that pregnant women do not have diminished systemic immunity. This is an important concept to take into account because inappropriate reduction in immunosuppression during pregnancy will lead to rejection of the transplanted organ5. Rejection may be difficult to detect during pregnancy. In this sample there was no case of acute rejection. The immune system in the pregnant woman is not totally understood, which complicates the therapeutic orientation. Cyclosporine increases production of thromboxane and endothelin, both of which have been implicated in the pathogenesis of pre-eclamp- sia6. Because of this, some physicians have suggested that the dose should be limited to 2-4 mg/ kg per day6,11. There is a paucity of data concerning the effect of tacrolimus on pregnancy6. As well as cyclosporine patients, pregnant women taking tacrolimus require frequent monitoring of renal function and drug levels to achieve the therapeutic range.
With regard to azathioprine, the foetus is relatively protected from the effects of this drug. Low birth weight, prematurity, jaundice, respiratory distress syndrome and aspiration have been reported in kidney transplant recipients and associated with a dose-related myelosuppression in the foetus12. Because precise data is limited, at the moment it is not recommended mycophenolate mofetil use. Prednisone and prednisolone can cross the placenta. Adrenal insufficiency and thymic hypoplasia have occasionally been described but these problems are unlikely to occur if the dose of prednisone has been decreased to 15mg6,13. Steroids may be implicated in the increased frequency of premature rupture of membranes and they can also aggravate hypertension in the mother14. There was no patient under mTOR inhibitors, which are known to be contraindicated in pregnancy. In our unit, during the reported period, there was no specific protocol related with the ideal immunosuppressive serum levels during gestation.
Pregnancy causes an increase in the glomerular filtration rate. In theory, this could lead to hyperfiltration and glomerulosclerosis, however, the hyperfiltration of pregnancy is related to increased plasma flow, with no concomitant increase in intra-glomerular pressure6,15. In this study, although a significant decrease between baseline and follow-up at 3 months post-partum was registered, when analysed a year after delivery, there was no significant decrease in eGFR relative to baseline. This suggests that a gradual recovery of the renal function may occur at least after 3 months post-partum. Only proteinuria maintained significantly increased a year after delivery, suggesting a long-term increased risk of graft dysfunction. Overall, in the majority of the recipients studied, and in studies with a larger population sample, pregnancy does not appear to cause exces- sive or irreversible problems with graft function if the function of organ transplant is stable prior to pregnancy16.
When analysing the different published reviews of kidney transplanted patients, it was observed that high blood pressure is prevalent among patients on calcineurin antagonists4. In this study, a signifi- cant increase in systolic and diastolic blood pressure was registered in the 3rd trimester, with a recovery to baseline after 1 year of follow-up (Fig. 2). No state of pre-eclampsia occurred during this study, although there are other studies with rates up to 20% among pregnant transplanted patients17,18. This result may be due to the following facts: it is a small sample, the difficulty of diagnosis, the blood pressure tends to increase after the 20th week, many patients already have mild proteinuria before the pregnancy and also because of the limitations of a retrospective study.
With regard to delivery outcome, according to the published guidelines, although gestation in a kidneytransplanted patient should be considered a high-risk pregnancy, the vaginal delivery is recommended in most transplant recipient women. Caesarean section should be performed only for standard obstetric reasons4. However, in this sample, as well as in other published studies19,20, the rates of induction and Caesarean section were significantly higher than in the general population. The European, the American, and the British registries on pregnancy and transplantation report that in more than 50% of the cases, prematurity and low birth weight will occur4. The percentage in this modest sample is 38%. Other recent studies have also shown lower rates to 24%. A better health care may contribute to a more positive result 21, 22.
No malformation was observed in the newborns. Although a particular pattern of malformation has not been shown to be associated with prednisone, azathioprine or calcineurin antagonists, some mal- formations have been related to the administration of micophenolate mofetil, thus, it is recommended to discontinue this drug before conception4.
In summary, post-renal transplantation pregnancy should still be considered a high-risk gestation due to the complications that may occur in both the mother and the foetus4, thus, it should be approached in a multidisciplinary way and both the follow-up visits and immunosuppressant monitoring should be carried out more often. A major limitation of this study was the fact that data was collected over a long time period, which may be influenced by changes in perinatal care and protocol changes in immunosuppression regimens. Many uncertainties persist when we are faced with a pregnancy in a transplanted woman, being imperative the need to conduct a multicentre study with more patients.
References
1. Zingraff J, Jungers P, Pélissier C, Nahoul K, Feinstein MC, Scholler R. Pituitary and ovarian dysfunctions in women on haemodialysis. Nephron 1982;30(2):149-153. [ Links ]
2. Rizzoni G, Ehrich JH, Broyer M, et al. Successful pregnancies in women on renal replacement therapy: report from the EDTA Registry. Nephrol Dial Transplant 1992;7(4):279-287. [ Links ]
3. Bramham K, Nelson-Piercy C, Gao H, et al. Pregnancy in renal transplant recipients: a UK national cohort study. Clin J Am Soc Nephrol 2013;8(2):290-298. [ Links ]
4. Díaz JM, Canal C, Giménez I, et al. [Pregnancy in recipients of kidney transplantation: effects on mother and child.] Nefrologia 2008;28(2):174-177. [ Links ]
5. McKay DB, Josephson MA, Armenti VT, et al. with the Womens Health Committee of the American Society of Transplantation. Reproduction and transplantation: report on the AST Consensus Conference on Reproductive Issues and Transplantation Am J Transplant. 2005;5(7):1592-1599. [ Links ]
6. Lessan-Pezeshki M. Pregnancy after renal transplantation: points to consider. Nephrol Dial Transplant 2002;17(5):703-707. [ Links ]
7. Wang X, Chen C, Wang L, Chen D, Guang W, French J. Conception, early pregnancy loss, and time to clinical pregnancy: a population-based prospective study. Fertil Steril 2003;79(3):577-584. [ Links ]
8. Wilcox AJ, Weinberg CR, OConnor JF, et al. Incidence of early loss of pregnancy. N Engl J Med 1988;319(4):189-194. [ Links ]
9. Muirhead N, Sabharwal AR, Rieder MJ, Lazarovits AI, Hollomby DJ. The outcome of pregnancy following renal transplantation–the experience of a single center. Transplantation 1992;54(3):429-432. [ Links ] [ Links ]
11. Lindheimer MD, Katz AI. Pregnancy in the renal transplant patient. Am J Kidney Dis 1992;19(2):173-176. [ Links ]
12. Davison JM, Dellagrammatikas H, Parkin JM. Maternal azathioprine therapy and depressed haemopoiesis in the babies of renal allograft patients. Br J Obstet Gynaecol 1985;92(3):233-239. [ Links ]
13. Penn I, Makowski EL, Harris P. Parenthood following renal transplantation. Kidney Int 1980;18(2):221-233. [ Links ]
14. Chhabria S. Aicardis syndrome: are corticosteroids teratogens? Arch Neurol 1981;38(1):70. [ Links ]
15. Baylis C. Glomerular filtration and volume regulation in gravid animal models. Baillieres Clin Obstet Gynaecol 1994;8(2):235-264. [ Links ]
16. Armenti VT, Radomski JS, Moritz MJ, Philips LZ, McGrory CH, Coscia LA. Report from the National Transplantation Pregnancy Registry (NTPR): outcomes of pregnancy after transplantation. Clin Transpl 2000:123-134. [ Links ]
17. Thompson BC, Kingdon EJ, Tuck SM, Fernando ON, Sweny P. Pregnancy in renal transplant recipients: The Royal Free Hospital experience. QJM 2003;96(11):837-844. [ Links ]
18. Bramham K, Nelson-Piercy C, Gao H, et al. Pregnancy in renal transplant recipients: a UK national cohort study. Clin J Am Soc Nephrol 2013;8(2):290-298. [ Links ]
19. Deshpande NA, James NT, Kucirka LM, et al. Pregnancy outcomes in kidney transplant recipients: a systematic review and meta-analysis. Am J Transplant 2011;11(11):2388-2404. [ Links ]
20. Levidiotis V, Chang S, McDonald S. Pregnancy and maternal outcomes among kidney transplant recipients. J Am Soc Nephrol. 2009;20(11):2433-2440. [ Links ]
21. Armenti VT, Radomski JS, Moritz MJ, et al. Report from the National Transplantation Pregnancy Registry (NTPR): outcomes of pregnancy after transplantation. Clin Transpl 2004:103-114. [ Links ]
22. Briggs JD, Jager K. The first year of the new ERA-EDTA Registry. Nephrol Dial Transplant 2001;16(6):1130-1131. [ Links ]
Dra Cristina Dias Cândido
Nephrology Department
Centro Hospitalar de Setúbal, Setúbal, Portugal
Rua Camilo Castelo-Branco
2910-446 Setúbal, Portugal
E-mail: cristinadcandido@gmail.com
Conflict of interest statement: None declared.
Received for publication: 02/06/2015 Accepted in revised form: 09/08/2015














