Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Análise Psicológica
versión impresa ISSN 0870-8231versión On-line ISSN 1646-6020
Aná. Psicológica vol.38 no.1 Lisboa mar. 2020
https://doi.org/10.14417/ap.1701
Leventhal’s self-regulatory Model applied to breast cancer
Modelo de auto-regulação de Leventhal no cancro da mama
Susana Fernandes1, Teresa McIntyre2
1Universidade Lusófona do Porto, Porto, Portugal
2College of Nursing and Texas Institute for Measurement, Evaluation and Statistics, University of Houston, Houston, USA
ABSTRACT
The aim of this study was to examine psychosocial adjustment to breast cancer, according to Leventhal’s self-regulation model. We tried to understand the role of emotional adjustment and illness representations in coping. The participants were 74 Portuguese recently diagnosed breast cancer patients. Measures included the Portuguese versions of: The Hospital Anxiety and Depression Scale (HADS), to assess emotional adjustment (anxiety; depression); the Brief Illness Perception Questionnaire (B-IPQ), to evaluate illness perceptions; and the Mental Adjustment to Cancer Scale (Mini-MAC) to assess coping style. The principal hypothesis was that illness perceptions and emotional adjustment would be significant predictors of coping before surgery. The hypothesis was confirmed for most coping strategies. Emotional adjustment and illness representations were significant predictors of coping, which supports Leventhal’s Self-Regulatory Model, in this sample. Emotional adjustment and illness perceptions were significant predictors of Helplessness/Hopelessness, Anxious Preoccupation, and Fighting Spirit coping strategies.
Key words: Leventhal’s self-regulatory model, Breast cancer, Psychosocial adjustment, Coping, Illness representations, Emotional adjustment, Psycho-oncology.
RESUMO
Este estudo analisa o ajustamento psicossocial ao cancro da mama, tendo por base o Modelo de auto-regulação de Leventhal. Procura compreender o papel do ajustamento emocional e representações de doença no coping. A amostra foi constituída por 74 mulheres Portuguesas recentemente diagnosticadas com cancro da mama. As medidas utilizadas foram: A Escala Hospitalar de Ansiedade e Depressão (HADS), para avaliar o ajustamento emocional (ansiedade e depressão); o Questionário de Perceções de Doença Breve (IPQ-B), para avaliar as perceções de doença; e a Escala de Ajustamento Mental ao Cancro (mini-Mac), para avaliar o coping. A hipótese previa que as perceções de doença e o ajustamento emocional fossem preditores significativos do coping, antes da cirurgia. A hipótese confirmou-se para a maioria das estratégias de coping, o que vai de encontro ao Modelo de auto-regulação de Leventhal. O ajustamento emocional e as perceções de doença são preditores significativos das estratégias de coping Impotência/Desesperança, Preocupação Ansiosa e Espírito de Luta.
Palavras-chave: Modelo de auto-regulação de Leventhal, Cancro da mama, Ajustamento psicossocial, Coping, Representações de doença, Ajustamento emocional, Psico-oncologia.
Introduction
Breast cancer is the leading cancer in Portuguese women and in all countries of Europe and it is also the first cause of death from cancer in European women (Ferlay et al., 2013). In Portugal, 6000 new cases are detected annually, and approximately 1500 women die with this disease (Direção Geral de Saúde, 2017). Breast cancer has the highest mortality of any cancer in women worldwide (Stewart & Wild, 2014). Breast cancer threatens an organ that is closely related to self-esteem, sexuality, femininity, the social roles and life itself, causing changes to various dimensions of patient’s life. Despite the progress in the diagnosis and treatment of disease, women with breast cancer are still struggling with several consequences of this health condition. Anxious symptoms, depression, anger, sadness, grief, denial, hopelessness, discouragement, body image changes and sexual problems, are some of the common responses of these women (Burgess et al., 2005; Fobair et al., 2006; Travado & Reis, 2013; Vedhara et al., 2001). The degree to which these responses appear is dependent on many aspects, and research about psychosocial adjustment to breast cancer, has given importance to several factors that explain this individual variation. Some factors have been emphasized, such as socio-demographic factors (age and education); clinical and disease factors (type and disease stage); emotional adjustment (anxiety and depression); personality; coping strategies; past experiences of stress; social support and knowledge about the treatment and prognosis (e.g., Akechi, Okuyama, Imoto, Yamawaki, & Uchitomi, 2001; Costanzo et al., 2007; Dunn & Steginga, 2000; Edgar, Remmer, Rosberger, & Fournier, 2000; Hack & Degner, 2004; Hjerl et al., 2003; Manuel et al., 2007; Ranchor & Sanderman, 2006; Reynolds et al., 2000). Studies have shown that the impact of breast cancer in the adjustment of women is greater immediately following diagnosis (Ranchor & Sanderman, 2006). Given the variability in adjustment to breast cancer (Glanz & Lerman, 1992), becomes crucial to identify psychosocial factors that facilitate or disturb this adjustment. The Self-regulation Model of Leventhal, Nerenz and Steele (1984; Leventhal et al., 1997), can be used to explain some of these differences in the adjustment to disease. Studies have confirmed that cognitive representations are important determinants for adaptative outcomes in chronic patients (Weinman & Petrie, 1997; Williams, 1997). The cognitions are a common theme to various models, being crucial to the understanding of the adjustment of women with breast cancer (Scheier & Carver, 2003), for adherence to treatment regimens (Horne, 2003), as well as for the results of the disease (Bradley, Calvert, Pitts, & Redma, 2001).The self-regulation model of Leventhal provides a way of studying illness representations and is implication in the adjustment of women with breast cancer.
In the model of Leventhal and colleagues (1997), both emotions and cognitions will guide coping behaviour and consequently influence breast cancer adjustment This model suggests that individuals construct cognitive and emotional perceptions of threats that will guide and regulate the behaviour (Leventhal et al., 1997). Leventhal and colleagues (1997), proposed a parallel-processing model in which people make simultaneously, cognitive and emotional representations of their disease. The authors suggested that there are five dimensions of the cognitive component of illness representation: identity (composed of factors such as symptoms and “labels”), timeline (expected duration), consequences (quantity of pain and impact on daily life activities), causes (internal or external – genes or infection), control (perception of disease as manageable, possibility of prevention or curing) (Leventhal, Brissette, & Leventhal, 2003). In this model, people are active, as processing information and elaborate representations of disease, reacting emotionally to the same (Leventhal, Leventhal, & Cameron, 2001). In this way, we can analyse the interconnection between illness representations, emotional adjustment, coping and subsequently psychological adjustment in women with breast cancer. Empirical studies testing this model have mainly focus on the relationship between cognitive representation dimension and coping behaviour (Vaughan, Morrison, & Miller, 2003) and not so much in emotional dimension. Which makes us believe in the existence of a gap in understanding the parallel processing of cognitions and emotions, as determinants of coping.
A meta-analytic study suggested a strong positive relationship between the cognitive representation dimensions, identity, consequences and timeline, and maladaptive outcomes such as anxiety and depression (Hagger & Orbell, 2003). Women perception of the consequences of her illness influences the process of adjustment (Broadbent, Petrie, & Weinman, 2006; Buick, 1997). As well according to Thuné-Boyle, Myers and Newman (2006), patients receiving treatment for cancer who consider their illness has a more serious impact on their lives were found to be more anxious and depressive. The study of Buick (1997), showed that high symptoms (identity dimension), keep the fear of recurrence and predict increased use of health care. The author also found that negative perceptions about breast cancer may interfere with the ability of patients to interpret and understand the treatment experience. In the study conducted by Rozema, Völlink and Lechner (2009), the illness representations seem to play an important role on perceived health in breast cancer. The authors find that women who view their illness as a condition associated to serious symptoms and consequences, patients who believe they have a chronic disease and patients who consider their illness uncontrollable, were found to report worse physical and mental health. In contrast, illness perceptions that facilitate the development of a more positive meaning, can also have a direct effect on adjustment to treatment through an increase in the perception of control and self-worth.
The adjustment to breast cancer disease and treatment involves strong emotional responses, especially at the level of anxiety and depression (Baumeister, Kriston, Bengel, & Härter, 2010; Härter et al., 2001), closely related to quality of life (Hutter et al., 2013). According to Akechi et al. (2001), the prevalence of psychiatric morbidity (including anxiety and depression, assessed through the HADS) was 23% in breast cancer. Thus, the emotional state appears as a crucial aspect in the psychosocial adjustment to breast cancer, with implications on psychological distress, coping responses, and in the course of the disease (Hjerl et al., 2003; Iwamitsu et al., 2005; Lueboonthavatchai, 2007; Reich, Lesur, & Perdrizet-Chevallier, 2007). Anxiety and depression have been referred as the main emotional alteration for women with breast cancer (Reich et al., 2007; Travado & Reis, 2013). Groarke, Curtis and Kein (2013), revealed that high depression was related with low fighting spirit and helplessness/hopelessness coping strategies. The authors also exposed that fighting spirit was related to high positive affect. Akechi et al. (2001), revealed that one of the major determinants of psychiatric morbidity in patients with breast cancer was high levels of helplessness/hopelessness. Another interesting aspect pointed out by Reich et al. (2007), is that the main risk factors for depression 5 years after diagnosis of breast cancer, relate more to the characteristics of the patient than with aspects of the disease and treatment. These risk factors include symptoms of fatigue, history of depression or recent episode of depression (after the onset of the disease), helplessness/hopelessness and resignation. These studies seems to indicate a bidirectional relationship between emotional state and coping, as had already been suggested by Watson et al. (1991).
The recent experience of a breast cancer is considered a crisis that in most patients extends to a year after surgery (Ganz, Kwan, Staton, Bower, & Belin, 2011) and, the way woman deal with this crisis can play an important role in adjustment. During this first year, women usually face various situations, such as diagnosis, surgery, treatments, for which make sense to use differentiated coping strategies with different goals (Culver, Arena, Winberly, Antoni, & Carver, 2002). In this way, it’s important to understand what strategies can be more effective at every stage of the disease, since we know that an effective strategy in a given time will not be necessarily effective in another time. Some studies have examined the relationship between coping style and psychological adjustment of women with breast cancer at different stages of the disease, such as initial stage of the disease, after the diagnosis, after mastectomy and during chemotherapy (e.g., Carver et al., 1993; Classen, Koopman, Angell, & Spiegel, 1996; Hack & Degner, 2004). In the study of Carver et al. (1993), women who reported more positive coping strategies, such as acceptance and humour, at the diagnosis, had less distress than women who used strategies as denial and disinvestment, at 1-year follow-up. Another longitudinal study conducted by Hack and Degner (2004), revealed that women who were depressed at the time of treatment planning and who responded to the diagnosis with a passive coping (avoidance and resignation), had a worse adjustment three years later. This seems to indicate that women who respond to their diagnosis of breast cancer with a passive coping, have a higher risk of developing a poor adjustment in the long term. Similarly, Jim, Richardson, Golden-Kreutz and Andersen (2006), studied longitudinally the relationship between coping and self-report about the disease meaning in the lives of women with breast cancer, two years after the diagnosis. The results indicated that positive coping strategies, predicted the attribution of a positive meaning to life (feelings of peace, satisfaction with current life and with the future, spirituality and “struggle”) and the absence of these strategies predicted reports of loss of meaning or confusion. Following the evidences of the studies, the active coping strategies seem to act as a relief for emotional stress, reflecting a positive adjustment to the disease (Carver et al., 2003; Jim et al., 2006). Studies also seem to indicate that avoidance, as a coping strategy, seems to contribute to a worse adjustment to breast cancer (Hack & Degner, 2004).
Several studies have been reported in the literature demonstrating associations between illness representations and cognitive and behavioural responses to disease (e.g., Jessop & Rutter, 2003; Petrie, Weinman, Sharpe, & Buckley, 1996, cit. Rees, Fry, Cull, & Sutton, 2004). Nevertheless, we consider that research has provided some limited evidence to support the relationship between illness representations and emotional adjustment in coping behaviour in breast cancer patients. We consider that greater specificity about illness representations, emotions and the situation with which women are coping is required. In addition, there are few studies about Leventhal’s self-regulation model in breast cancer patients and no one in Portuguese women.
This study: Aim and hypothesis
The general objective of this study is to examine psychosocial adjustment to breast cancer, in newly diagnosed women, according to Leventhal’s self-regulation model. Thus, this study proposed to test Leventhal’s Self-regulatory Model in breast cancer patients.
Method
Participants and procedures
The sample consisted of 74 women newly diagnosed with breast cancer, recruited at the Portuguese Institute of Oncology of the Northern region of Portugal. The eligibility criteria for inclusion in the study were: (1) have been diagnosed with breast cancer for the first time, (2) have been diagnosed at stage I-III of the disease, (3) have not yet performed surgery, (4) do not participate in other psychological studies.
The study was initiated after the authorization of the Ethics Committee of the Hospital. Women were invited to participate when they heading to surgical planning. Nurses forwarded patients for a contact with a psychologist. After being informed about the study and obtained the informed consent, patients were interviewed by the psychologist. It was adopted a standardized procedure of administration of instruments in hetero report, due to the low socio-educational level of the participants. This contact had a duration of about 30 minutes.
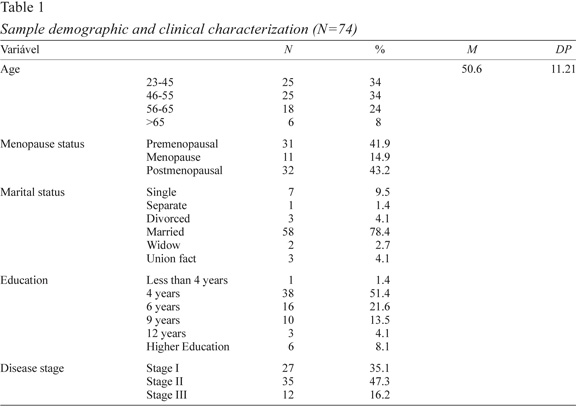
As can be analysed in Table 1, the number of women who agreed participate in the study were 74. The mean age of the sample was 50.6 years old (SD=11.21). Most women were married, 78.4%, more than a half have only 4 years of education (51.4%) and only 8.1% have higher education. In what respect to menopause, 41.9% were in menopause. Predominantly, women were diagnosed in stage II of disease (47.3%); in stage I (35.1) and in stage III (16.2%).
Measures
Sociodemographic and disease-related information. Data were collected through a social and demographic questionnaire; medical records (to obtain information about disease stage) and questionnaires that evaluated psychological variables (illness perception; coping; anxiety and depression).
Illness perception. The Brief Illness Perception Questionnaire (Broadbent, Petrie, Main, & Weinman, 2006), consists in nine items that evaluate the emotional and cognitive representations of disease. Each of these statements is assigned a response on a 5-point Likert scale. In this study we used the Portuguese version of the IPQ-B. To evaluate the psychometric qualities of IPQ-B, in this sample, the authors followed the same procedures of the original study (Broadbent et al., 2006). Similarly, to the original authors, the construct validity of the IPQ-B was evaluated through Pearson correlations between the dimensions of the instrument, verifying that the correlations between the scales are low to moderate and mostly non-significant, which supports the specificity of these dimensions. The data found allow us to use IPQ-B in our study.
Coping strategies. Coping strategies were assessed using the Portuguese version of Mental Adjustment to Cancer Scale, Mini-MAC (Pais-Ribeiro, Ramos, & Samico, 2003; Watson et al., 1994). It consists in 29 items, and five sub-scales: Fighting Spirit, Helplessness/hopeless, Fatalism, Anxious Preoccupation and Cognitive Avoidance. Each item is a statement describing reactions from the patient with cancer diagnosis. The patient must respond to an ordinal scale of four positions (between “does not apply in any way to me” until “totally applies to me”). The score of the scales can range from 4 to 40. The Mini-MAC is a multidimensional scale that does not allow obtaining a total result, i.e., does not allow to sum the partial scores in a total score. In this study, it was not possible to perform internal consistency analysis or factorial analysis due to the number of participants not allowing. The study of convergent and divergent validity was performed through correlations between Mini-MAC and HADS subscales. The results indicated that the helplessness/ hopelessness is positively correlated with the subscales of anxiety and depression of the HADS (R=.47 and. 64, p≤.01, respectively), as well as anxious preoccupation (R=.68 and. 59, p≤.01, respectively). These associations were also found by Watson et al. (1994). A negative correlation was found between the fighting spirit and the subscales of anxiety and depression (r=-.36 and -.58, p≤.01 respectively), like the original study (r=-.19 and -.24, p<.001). In general, the correlation pattern found in our study goes in the expected direction, supporting the convergent and divergent validity of the scales. The analyses allow us to affirm the multidimensionality of the Mini-MAC and indicate its convergent and divergent validity.
Emotional adjustment. Emotional adjustment was evaluated with the Portuguese version of Hospital Anxiety and Depression Scale, HADS (Zigmond & Snaith, 1983). The Hospital Anxiety and Depression Scale consists of a sub-scale of anxiety, consisting of 7 items, and a sub-scale of depression, consisting of other 7 items. The responses to each item can be quantified on a Lickert-type scale, varying from 0 to 3, with the highest values revealing higher psychological distress. Thus, each item allows the choice of four response options, in which the patient must choose the one that corresponds to the way it has been felt during the last week. Each subscale can have a score that varies between 0 and 21; The higher the score, the higher the levels of anxiety and depression. Scores of 11 or higher, indicate possible anxiety or mood disorder. Cronbach’s alpha was calculated in this sample, with values of 0.75 for depression 0.81 for anxiety and 0.86 for the total scale. The results obtained in the test-retest fidelity analysis show that in the period of 1-month, the subscales have good temporal stability, with correlations above. 50 (p≤.01). We can conclude that this instrument presents good fidelity in terms of internal consistency and temporal stability.
Results
To test this hypothesis, we used hierarchical multiple regression analysis (Enter model), in which the representations of disease and treatment, and emotional state, enter as predictors and coping, as variable of result. In the block 1 were introduced the age or educational level (if they are significant variables), in block 2 were introduced anxiety and depression and in block 3 representations of disease and treatment.
Before we proceed to the hierarchical regression analyses, we have conducted a correlation between the emotional state, the representations of disease and coping (see Table 2). These correlations allow us to select which predictive variables, correlate with the result and that should be included in the hierarchical regression analysis.
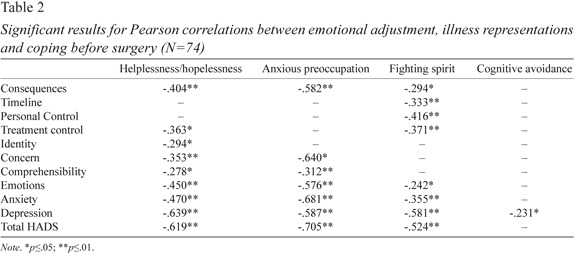
Illness perception and emotional state as predictors of coping before surgery
Table 3 results showed that emotional adjustment is a significant predictor of Helplessness/Hopelessness before surgery (F=22.864, p<.001), explaining about 35% of the variance. Anxiety seems to be the significant predictor of concomitant coping, observing that as the higher the anxiety, the greater the use of coping by helplessness/hopelessness. The illness perceptions explain about 10% of the variance of helplessness/hopelessness. The perception of the consequences presents a positive partial correlation, indicating that the greater the perception of interference of the disease in the life of the patient, the greater use of helplessness/hopelessness coping strategy. As to the treatment control, this belief presents a partial negative correlation with the coping, which indicates that the higher the belief in the efficacy of the treatments, the smaller coping by helplessness/hopelessness. Another significant variable that predicts the helplessness/hopelessness coping strategy is education (about 12% of the variance), checking that with the increase of education decreases the helplessness/hopelessness. Thus, the variables included in our model explains about 51% of the variance in this coping strategy.
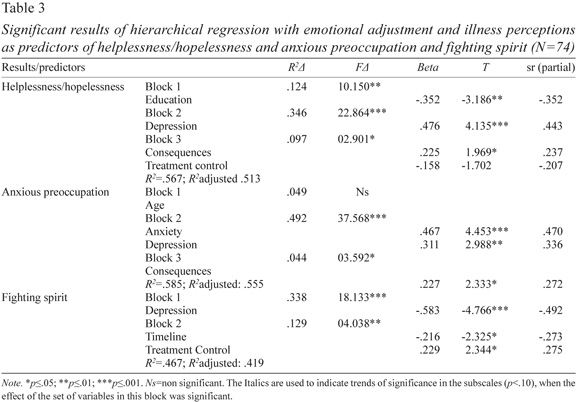
About the anxious preoccupation, results exposed that the emotional adjustment is a significant predictor of anxious preoccupation coping strategy, explaining a large part of the variance in the use of this strategy (49%). The increases of anxiety and depression conducts to the greater use of anxious preoccupation coping strategy. Regarding illness perceptions, these have proved to be significant predictors of anxious preoccupation, explaining about 4% of the variance. Univariate results show that only the consequences perception of the disease is a significant predictor of this coping strategy in the period before the surgery, noting that a more negative consequences perception of the disease is associated with the major anxious preoccupation. We can achieve that with the variables included in our model we obtained a variance explained about 56% on this coping strategy.
The results concerning the fighting spirit, revealed that the emotional adjustment explained 34% of variance of this coping strategy, with depression contributing significantly to this relation (sr=-.49). Thus, the higher pre-surgery depression, less recourse to fighting spirit as a way of dealing with the disease. The illness perceptions explain about 13% of the use of fighting spirit. The variables that were significant were the timeline and treatment control. The partial correlation between timeline and fighting spirit is negative, indicating that with the greater perception of disease chronicity, the lower the use of this coping strategy. In what concerns to the treatment control, the correlation between the variables is positive, revealing that the higher the perception of effectiveness of proposed treatments, greater recourse to coping by fighting spirit. The global model presented here explain in about 42% the variance found in fighting spirit.
Results summary
The results obtained revealed that emotional adjustment and illness perceptions are concomitant predictors of coping, proving for this sample, the Leventhal’s self-regulation model. We found that the emotional adjustment and illness perceptions are significant predictors of coping strategies, helplessness/hopelessness, anxious preoccupation and fighting spirit. The variance explained by these two sets of variables is very high (between 41 and 55%), which confirm the relevance of these variables in this model. The emotional adjustment was the most important predictor, for all coping strategies, explaining more than twice the variance of the illness perceptions. Emotional adjustment tends to be a stronger predictor of coping than the illness representations. Depression was a significant predictor of the three coping strategies, positively correlated with helplessness/hopelessness and anxious preoccupation and negatively with fighting spirit. In terms of illness perceptions, the perception of negative consequences of the disease in the life of the person, was a predictor of greater use of coping by helplessness/hopelessness and anxious preoccupation, while the less chronic perception of the duration of the disease and greater efficacy of treatments, was associated with greater use of the fighting spirit. In conclusion, emotional adjustment and illness representations are predictors of coping, which proves the hypothesis, in its generality.
Discussion
This study intends to test the self-regulation model of disease, which postulates the occurrence of parallel emotional process and cognitive mechanisms, which together will guide and determine the behaviour, including coping with the disease (Leventhal et al., 1997).
The results show that emotional adjustment and illness perceptions predict much of the coping before surgery. The hypothesis is confirmed for helplessness/hopelessness, anxious preoccupation and fighting spirit coping strategies. It was found that negative emotions (more specifically the Depression) and negative representations of disease (i.e. the perception of negative consequences), predict the use of helplessness/hopelessness. Regarding anxious preoccupation, negative emotions such as anxiety and depression predict the use of this coping strategy, as well as the negative disease perceptions, especially the consequences. Both helplessness/hopelessness and anxious preoccupation are coping strategies that can indicate a poor adjustment at this stage of the disease and, as we can verify, both can be predicted by a negative emotions and illness representations, such as the perception of disease interference in daily activities. We can consider that the fighting spirit is an appropriate coping strategy at this stage of the disease, and it is possible to verify that a more positive emotional adjustment and positive health perceptions predict the use of this coping strategy. Thus, depression is the only variable that emerges as a significant predictor. Consequently, women who present lower levels of depression are those who use more the fighting spirit coping strategy. The illness perception, related to the duration of the disease, is also a predictor of fighting spirit, and the lower the perception of the duration, the greater fighting spirit. Women who believe in the efficacy of treatments (treatment control), use the fighting spirit, more, as a coping strategy. The adoption of a coping strategy that we can consider adaptive, appears associated either to a more positive emotional state or to more positive health beliefs that reflect optimism regarding a limited duration of the disease and efficacy of the proposed treatments. With these results we are led to believe that a more positive perception about the disease, can be an important predictor of adjusted coping strategies, as fighting spirit. Our results are aligned with Watson et al. (1991), who report that the adoption of a fighting spirit appears associated with a decrease in anxiety and depression. What makes us believe in a bilateral relationship between emotional state and coping, that is, a more positive emotions contributes to a greater use of adaptive coping, and in turn, the adoption of the fighting spirit leads to a decrease in anxiety and depression.
Since the depression and the most optimistic illness perceptions (limited duration of the disease and confidence in the efficacy of the treatments), emerge as predictors of an adaptive coping strategy, it is believed that intervention at these levels will be pertinent to facilitate adjustment at this stage of the disease. In their study, McCorry and colleagues (2013), concluded that illness perceptions in breast cancer are resistant to change without directed intervention designed specifically at modifying them. Other studies suggest that designing an intervention that specifically targets patients’ illness perceptions might yield positive results for patients’ emotional well-being (Fisher et al., 2013). To improve these aspects, we suggest that illness representations may be enhanced through educational interventions, with information about the consequences of the disease, duration, type of treatment, its efficacy and prognosis. At the emotional level, a cognitive-behavioural intervention can be used. To improve the adjustment of breast cancer patients, health professionals should be aware about the illness representations, emotional state and coping strategies who are more efficient at each moment of the treatment.
Limitations and strengths
To better interpret the results of this study, it is important to consider some methodological limitations associated with this in terms of its internal and external validity. Firstly, it is important to consider the reduced size of the sample and the use of the consecutive non-probabilistic sampling method (Luna, 1998). The small number of subjects raises obstacles to the generalization of the results (external validity) and the representativeness of the sample in relation to the study population (Conboy, 1995). An important limitation of this study relates to the fact that most participants have a diagnosis of stage II, limiting the comprehension of the disease in more advanced stages such as IV. However, the results obtained are in the same direction of the existing literature suggesting that our data has some external validity. A second limitation relates to the instruments used that are administered in hetero-report, which may have increased the effect of social desirability. Despite this limitation, the questionnaires used are reference instruments in this type of investigation and presented good psychometric qualities in the study sample, which increases confidence in the validity of the data obtained. Regardless these limitations, this study is innovative because it seeks to analyse the psychosocial adjustment of newly diagnosed Portuguese women, with breast cancer. The data related to this type of study are important for the identification of predictors, of the result variables when they are testing theoretical models referring to the adjustment process. One of the critics that has been raised to interventions in the field of psycho-oncology is the lack of a theoretical orientation that support them (Helgeson, 2005). This study also represents an effort to integrate theory and research, as it seeks to test the role of the emotional adjustment and the illness representation in coping with breast cancer, according to the Leventhal’s Self-regulatory Model.
References
Akechi, T., Okuyama, T., Imoto, S., Yamawaki, S., & Uchitomi, Y. (2001). Biomedical and psychosocial determinants of psychiatric morbidity among postoperative ambulatory breast cancer patients. Breast Cancer Research Treatment, 65, 195-202. [ Links ]
Baumeister, H., Kriston, L., Bengel, J., & Härter, M. (2010). High agreement of self-report and physician-diagnosed somatic conditions yields limited bias in examining mental-physical comorbidity. Journal of Clinical Epidemiology, 63, 393-406. [ Links ]
Bradley, E. J., Calvert, E., Pitts, M. K., & Redman, C. W. E. (2001). Illness identity and self-regulatory model in recovery from early stage gynaecological cancer. Journal of Health Psychology, 6, 511-521. [ Links ]
Broadbent, E., Petrie K. J., Main, J., & Weinman, J. (2006). The brief illness perception questionnaire. Journal of Psychosomatic Research, 60, 631-637. Retrieved from https://doi.org/10.1016/j.jpsychores.2005.10.020 [ Links ]
Buick, D. L. (1997). Illness representations and breast cancer: Coping with radiation and chemotherapy. In K. J. Petrie & J. Weinman (Eds.), Perceptions of health and illness (pp. 379-410). Amesterdam: Harwood Academic Publishers. [ Links ]
Burgess, C., Cornelius, V., Love, S., Graham, J., Richards, M., & Ramirez, A. (2005). Depression and anxiety in women with early breast cancer: Five year observational cohort study. British Medical Journal, 330, 702-705. [ Links ]
Carver, C. S., Pozo-Kaderman, C., Harris, S. D., Noriega, V., Scheier, M. F., Robinson, D. S., . . . Clark, K. C. (1993). How coping mediates the effect of optimism on distress: A study of women with early stage breast cancer. Journal Personality and Social Psychology, 65, 375-390. [ Links ]
Classen, C., Koopman, C., Angell, K., & Spiegel, D. (1996). Coping styles associated with psychological adjustment to advanced breast cancer. Health Psychology, 15, 434-437. [ Links ]
Conboy, J. (1995). A estimativa da magnitude do N de uma amostra. Aveiro: CIDINE. [ Links ]
Costanzo, E. S., Lutgendorf, S. K., Mattes, M. L., Trehan, S., Robinson, C. B., Tewfik, F., & Roman, S. L. (2007). Adjusting to life after treatment: distress and quality of life following treatment for breast cancer. British Journal of Cancer, 97, 1625-1631. Retrieved from https://doi.org/10.1038/sj.bjc.6604091 [ Links ]
Culver, J. L., Arena, P. L., Winberly, S. R., Antoni, M. H., & Carver, C. S. (2002). Coping and distress among women under treatment for early stage breast cancer: Comparing African Americans, Hispanics and non-hispanic whites. Psycho-oncology, 11, 495-504. [ Links ]
Direção Geral de Saúde. (2017). Portugal: Doença oncológica em números 2017. Retirado a 8 de Janeiro de 2019, de https://www.dgs.pt/portal-da-estatistica-da-saude/diretorio-de-informacao/diretorio-de-informacao/pornivel-de-informacao.aspx [ Links ]
Dunn, J., & Steginga, S. K. (2000). Young women’s experience of breast cancer: Defining young and identifying concerns. Psycho-Oncology, 9, 137-146.
Edgar, L., Remmer, J., Rosberger, Z., & Fournier, M. (2000). Resource use in women completing treatment for breast cancer. Psycho-Oncology, 9, 428-438. [ Links ]
Ferlay, J., Steliarova-Foucher, E., Lortet-Tieulent, J., Rosso, S., Coebergh, J. W., Comber, H., . . . Bray, F. (2013). Cancer incidence and mortality patterns in Europe: Estimates for 40 countries in 2012. European Journal of Cancer, 49, 1374-1403. [ Links ]
Fobair, P., Stewart, S. L., Chang, S., D’Onofrio, C., Banks, P. J., & Bloom, J. R. (2006). Body image and sexual problems in young women with breast cancer. Psycho-Oncology, 15, 579-594. Retrieved from https://doi.org/10.1002/pon.991
Ganz, P., Kwan, L., Staton, A., Bower, J., & Belin, T. (2011). Physical and psychosocial recovery in the year after primary treatment of breast cancer. Journal of Clinical Oncology, 29, 1101-1109. [ Links ]
Glanz, K., & Lerman, C. (1992). Psychological impact of breast cancer: A critical review. Annals of Behavioral Medicine, 14, 204-212. [ Links ]
Groarke, A., Curtis, R., & Kein, K. (2013). Global stress predicts both positive and negative emotional adjustment at diagnosis and post-surgery in women with breast cancer. Psycho-Oncology, 22, 177-185. [ Links ]
Hack, T. F., & Degner, L.F. (2004). Coping responses following breast cancer diagnosis predict psychological adjustment three years later. Psycho-Oncology, 13, 235-247. [ Links ]
Hagger, M. S., & Orbell, S. (2003). A meta-analytic review of the common sense model of illness representations. Psychology and Health, 18, 141-184. Retrieved from https://doi.org/10.1080/088704403100081321 [ Links ]
Härter, M., Reuter, K., Aschenbrenner, A., Schretzmann, B., Marschner, N., Hasenburg, A., & Weis, J. (2001). Psychiatric disorders and associated factors in cancer: Results of an interview study with patients in inpatient, rehabilitation and outpatient treatment. European Journal of Cancer, 37, 1385-1393. [ Links ]
Helgeson, V. S. (2005). Recent advances in psychosocial oncology. Journal of Consulting and Clinical Psychology, 75, 268-271. [ Links ]
Hjerl, K., Andersen, E., Keiding, N., Mouridsen, H., Mortensen, P., & Jorgensen, T. (2003). Depression as a prognostic factor for breast cancer mortality. Psychosomatics, 44, 24-30. [ Links ]
Horne, R. (2003). Treatment perceptions and self-regulation. In L. D. Cameron & H. Leventhal (Eds.), The self regulation of health and illness behaviour (pp. 138-154). New York: Routledge. [ Links ]
Hutter, N., Vogel, B., Alexander, T., Baumeister, H., Helmes, A., & Bengel, J. (2013). Are depression and anxiety determinants or indicators of quality of life in breast cancer patients?. Psychology, Health and Medicine, 18, 412-419. Retrieved from https://doi.org/10.1080/13548506.2012.736624 [ Links ]
Iwamitsu, Y., Shimoda, K., Abe, H., Tani, T., Okawa, M., & Buck, R. (2005). Anxiety, emotional supression, and psychological distress before and after breast cancer diagnosis. Psychosomatics, 46, 19-24. [ Links ]
Jessop, D. C., & Rutter, D. R. (2003). Adherence to asthma medication: The role of illness representations. Psychology and Health, 18, 595-612. Retrieved from https://doi.org/10.1080/0887044031000097009 [ Links ]
Jim, H. S., Richardson, S. A., Golden-Kreutz, D. M., & Andersen, B. L. (2006). Strategies used in coping with a cancer diagnosis predict meaning in life for survivors. Health Psychology, 25, 753-761. [ Links ]
Leventhal, H., Nerenz, D. R., & Steele, D. J. (1984). Illness representation and coping with health threats. In A. Baum, S. E. Taylor, & J. E. Singer (Eds.), Handbook of psychology and health: Social psychological aspects of health (Vol. 4, pp. 219-252). Hillsdale, NY: Erlbaum. [ Links ]
Leventhal, H., Benyamnini, Y., Brownlee, S., Diefenbach, M., Leventhal, E. A., Patrick-Miller, L., & Robitaille, C. (1997). Illness representations: Theoretical foundations. In K. J. Petrie & J. A. Weinman (Eds.), Perceptions of health & illness (pp. 19-45). Amsterdam: Harwood Academic Publishers. [ Links ]
Leventhal, H., Leventhal, E. A., & Cameron, L. (2001). Representations, procedures and affect in illness self-regulation: A perceptual-cognitive model. In A. Baum, T. A. Revenson, & J. E. Singer (Eds.), Handbook of health psychology (pp. 19-47). Mahwah, NJ: Lawrence Erlbaum Associates. [ Links ]
Leventhal, H., Brissette, I., & Leventhal, E. A. (2003). The common-sense model of self-regulation of health and illness. In L. D. Cameron & H. Leventhal (Ed.), The self-regulation of health and illness behaviour (pp. 42-65). New York: Routledge. [ Links ]
Lueboonthavatchai, P. (2007). Prevalence and psychosocial factors of anxiety and depression in breast cancer. Journal Medical Association of Thai, 90, 2164-2174. [ Links ]
Luna, F. B. (1998). Sequência básica na elaboração de protocolos de pesquisa. Arquivo Brasileiro de Cardiologia, 71, 735-740. [ Links ]
Manuel, J. C., Burwell, S. R., Crawford, S. L., Lawrence, R. H., Farmer, D. F., Hege, A., . . . Avis, N. E. (2007). Younger women’s perceptions of coping with breast cancer. Cancer Nursing, 30, 85-94.
McCorry, N. K., Dempster, M., Quinn, J., Hogg, A., Newell, J., Moore, M., . . . Kirk, S. J. (2013). Illness perception clusters at diagnosis predict psychological distress among women with breast cancer at 6 months post diagnosis. Psycho-Oncology, 22, 692-698. Retrieved from https://doi.org/10.1002/pon.3054
Pais-Ribeiro, J. L., Ramos, D., & Samico, S. (2003). Contribuição para uma validação conservadora da escala reduzida de ajustamento mental ao cancro (Mini-Mac). Psicologia, Saúde & Doença, 4, 231-247. [ Links ]
Ranchor, A. V., & Sanderman, R. (2006). The role of personality in cancer onset and survival. In M. E. Vollrath (Ed.), Handbook of personality and health (pp. 35-49). England: John Wiley & Sons, Ltd. [ Links ]
Reich, M., Lesur, A., & Perdrizet-Chevallier, C. (2007). Depression, quality of life and breast cancer: A review of the literature. Breast Cancer Research and Treatment, 110, 9-17. [ Links ]
Rees, G., Fry, A., Cull, A., & Sutton, S. (2004). Illness perceptions and distress in women at increased risk of breast cancer. Psychology and Health, 19, 749-765. [ Links ]
Reynolds, P., Huley, S., Torres, M., Jacson, J., Boyd, P., & Chen, V. W. (2000). Use of coping strategies and breast cancer survival: Results from black/white cancer survival study. American Journal of Epidemiology, 153, 757-763. [ Links ]
Rozema, H., Völlink, T., & Lechner, L. (2009). The role of illness representations in coping and health of patients treated for breast cancer. Psycho-Oncology, 18, 849-857. [ Links ]
Scheier, M. F., & Carver, C. S. (2003). Goals and confidence as self-regulatory elements underlying health and illness behavior. In L. D. Cameron & H. Leventhal (Eds.), The self-regulation of health and illness behaviour (pp. 17-41). New York: Routledge. [ Links ]
Stewart, B. W., & Wild, C. P. (Eds.). (2014). World cancer report. Lyon, France: International Agency for Research on Cancer. [ Links ]
Thuné-Boyle, I. C., Myers, L. B., & Newman, S. P. (2006). The role of illness beliefs, treatment beliefs, and perceived severity of symptoms in explaining distress in cancer patients during chemotherapy treatment. Behavioural Medicine, 32, 19-29. [ Links ]
Travado, L., & Reis, J. C. (2013). Breast cancer meanings: A cognitive-developmental study. Psycho-Oncology, 22, 2016-2023. [ Links ]
Vaughan, R., Morrison, L., & Miller, E. (2003). The illness representations of multiple sclerosis and their relations to outcome. British Journal of Health Psychology, 8, 287-301. [ Links ]
Vedhara, K., Bennett, P., Brooks, E., Gale, L., Munnoch, K., Schreiber-Koutine, C., . . . Farndon, J. (2001). Risk factors for psychological morbidity in women attending a one-stop diagnostic clinic with suspected breast disease. Psychology and Health, 16, 179-190. [ Links ]
Watson, M., Greer, S., Rowden, L., Gorman, C., Robertson, B., Bliss, J. M., & Tunnore, R. (1991). Relationships between emotional control adjustment to cancer and depression and anxiety in breast cancer patients. Psychological Medicine, 21, 51-57. [ Links ]
Watson, M., Law, M., Santos, M., Greer, S., Baruch, J., & Bliss, J. (1994). The mini-Mac: Fither development of the mental adjustment to cancer scale. Journal of Psychosocial Oncology, 12, 33-46. [ Links ]
Weinman, J., & Petrie, K. J. (1997). Illness perceptions: A new paradigm for psychosomatics?. Journal of Psychosomatic Research, 42, 113-116. [ Links ]
Williams, C. (1997). A cognitive model of dysfunctional illness behaviour. British Journal of Health Psychology, 2, 153-165. [ Links ]
Zigmond, A. S., & Snaith, R. P. (1983). The Hospital Anxiety and Depression Scale. Acta Psychiatry Scand, 67, 361-370. [ Links ]
Correspondence concerning this article should be addressed to: Susana Fernandes, Universidade Lusófona do Porto, R. de Augusto Rosa, 24, 4000-098 Porto, Portugal. E-mail: susanamrfernandes@gmail.com
Submitted: 17/03/2019 Accepted: 01/10/2019