Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Portuguese Journal of Nephrology & Hypertension
versão impressa ISSN 0872-0169
Port J Nephrol Hypert vol.31 no.1 Lisboa mar. 2017
CASE REPORT
Rare aetiology of obstructive kidney injury: Bilateral ureteral endometriosis
Maria Inês Correia1, Pedro Vieira2, António M Gonçalves2, José M Durães2, Dina Santos1, Nuno G Rosa2, Gil Silva2
1 Serviço de Medicina Interna do Hospital Central do Funchal Hospital dos Marmeleiros, Estrada dos Marmeleiros, 9050-495 Funchal 2 Serviço de Nefrologia do Hospital Central do Funchal Avenida Luís de Camões Nº 57, 9004-514 Funchal
ABSTRACT
Endometriosis is highly prevalent in women at the reproductive age, ranging from 6-10%, though ureteral involvement is rare, only seen in 0.1% of the cases, but may lead to urinary tract obstruction with potential renal function loss. As endometriosis has a non-specific symptomology, diagnosis may be elusive, though it must be considered in order to prevent irreversible kidney injury and resultant morbidity. Here we present a 29-year-old Caucasian female with a past medical history of infertility and dysmenorrhoea who presented with a stage II acute kidney injury. On initial diagnostic approach, moderate bilateral ureterohydronephrosis was detected by ultrasound, assuming extrinsic compression, but no specific cause was recognizable. In order to diagnose the obstructions aetiology, Magnetic Resonance Imaging was used. This did not reveal an objective cause. Given the circumstances, workup ended in an explorative laparotomy, revealing a frozen pelvis due to endometriosis, confirmed histologically.
Due to difficult ressecability, a conservative approach was taken through hormonal treatment and bilateral ureteral pigtail placement, given the necessity to salvage renal function and decrease disease burden.
Key-Words: Endometriosis, Ureteral Obstruction, Hydronephrosis, Acute Kidney Injury, Chronic Renal Insufficiency
INTRODUCTION
Endometriosis is an oestrogen-dependent disorder characterized by the presence of functional endometrial-like tissue outside the uterine cavity, capable of prompting complications due to its infiltrative nature or by formation of adhesions1. It is highly prevalent among women of reproductive age, ranging from 6-10%2. Urinary tract involvement, however, is rarer, accounting for only 1-2% of all cases3 and prevalence of ureteral endometriosis is much lower, with studies reporting incidences of only 0.1%4. The disease usually affects the distal segment of the ureter, usually the left one, denoting a clear lateral asymmetry which is compatible with the menstrual reflux theory5. Nonetheless, bilateral involvement has been described in up to 10-20% of cases6. Ureteral endometriosis can be further classified into either intrinsic or extrinsic, the latter more common and usually less symptomatic, raising the likelihood of silent loss of renal function7.
As a timely diagnosis is important we present a case of bilateral ureteral endometriosis with a dim prognosis.
CASE REPORT
A 29-year-old Caucasian woman, gravida 0, para 0, was referred to our emergency department due to routine laboratory analysis finding a stage II acute kidney injury (AKI)8. Apart from previous history of infertility and dysmenorrhoea, her medical history was unremarkable with no relevant family history, no previous surgeries and no relevant occupational exposure.
She was not currently on any chronic medication, referring only sporadic use of paracetamol and a previous history of oral contraceptive use. At admission, the patient presented no symptomatology, including genitourinary or abdominal complaints, and had no apparent changes on physical examination. Ensuing diagnostic approach included laboratory tests that confirmed a stage II AKI (serum creatinine 2.86 mg/dL as opposed to a basal level of 1,00 mg/dL and an urea level of 82 mg/dL) paired with an otherwise normal evaluation, including no urinalysis abnormalities.
A renal ultrasound (Fig. 1) found moderate bilateral hydroureteronephrosis (grade 3) along with normalsized kidneys and preserved parenchymal differentiation.
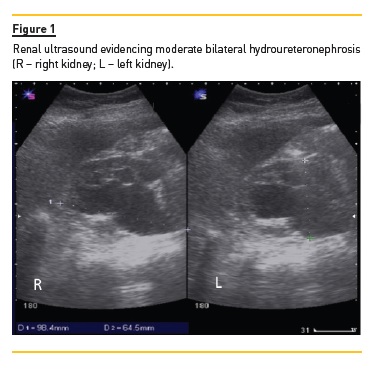
A computerized tomography (Fig. 2) was performed to clarify the obstructions aetiology and confirmed a bilateral obstruction but shed no further light on the cause. However, the finding of a thickened right mesorectal fascia raised the possibility of either a colorectal or uterine cervix cancer. Suspecting a bilateral urinary obstruction secondary to a pelvic tumour, we performed a conservative urinary derivation by double pigtail ureteral stenting to allow investigation of the aetiology. Subsequent diagnostic workup revealed normal gastrointestinal endoscopies and cervical pathology studies but elevated serum CA-125 levels (332.7 IU/mL) stood out. During followup, a uro-magnetic resonance (Fig. 3) was performed but no additional information was obtained, outlining the need for an explorative laparotomy, where macroscopic appearance suggested multiple foci of scattered endometriosis (diaphragmatic cupula, parietal peritoneum over the anterior abdominal wall, parietocolic gutters and pelvic involvement of uterus, bladder and rectum) presenting as a frozen pelvis.
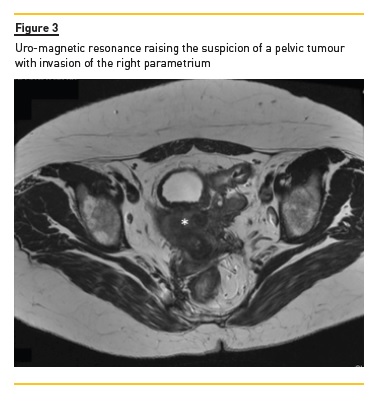
This was later confirmed histologically by the finding of endometrial glands and stroma staining positive against CD10 antibody and oestrogen receptor antibodies.
Given the widespread bilateral ureteral involvement determining an unresectable disease, a conservative approach was taken consisting of hormonal therapy (combined oral contraceptives) and bilateral ureteral pigtail placement in order to salvage renal function and decrease disease burden. Postoperative follow-up showed reduction of serum creatinine and urea levels to 1.45 mg/dL and 43 mg/dL, respectively. Uro-magnetic resonance showed improvement of previously diagnosed hydronephrosis, still sustaining residual ureteral obstruction, while CA-125 was normalized to 16.12 IU/mL after 4 months.
She was kept on cyclical combined oral contraceptives for 12 months but residual dysmenorrhoea led to hormonal therapy being exchanged for a Levonorgestrel-Releasing Intrauterine System, with complete symptomology resolution while bilateral ureteral pigtails were kept, with periodical replacement every 6 months. The patient has now been under a 3-year follow-up with no current symptomology and no suggestion of worsening hydronephrosis. However, she has experienced multiple complicated urinary tract infections episodes and evidence of renal function decline, with serum creatinine level increasing to 2.00 mg/dL suggesting chronic kidney diseases progression, with all its inherent complications, meaning a poor long-term prognosis.
DISCUSSION
Endometriosis is considered a benign condition though it may present an aggressive clinical behaviour, given its progressive and elusive course with a reported risk of silent renal loss as high as 25-50%9. Ureteral endometriosis potential deterioration in renal function is rare but must be considered, as a timely diagnosis may grant an easier treatment and better prognosis.
At an early stage of the disease, hormone therapy alone may be sufficient to prevent any development of fibrosis10, whereas at later stages, with progression of fibrosis, more aggressive approaches must be considered with the main aim of relieving renal obstruction and functional loss11. In terms of treatment approaches, one must then consider multiple factors, from extent of disease to the degree of hydronephrosis and renal function compromise. Treatment ranges from hormonal therapy alone or with double-J stent insertion, ureterolysis, segmental ureterectomy and end-to-end anastomosis, or segmental ureterectomy and uretrocystoneostomy, and nephrectomy (5, 12).
References
1. Audebert A, Backstrom T, Barlow DH, Benagiano G, Brosens I, Buhler K, et al. Endometriosis 1991: a discussion document. Hum Reprod. 1992;7(3):432-435. [ Links ]
2. Bulun SE. Endometriosis. The N Engl J Mede. 2009;360(3):268-79. [ Links ]
3. Westney OL, Amundsen CL, McGuire EJ. Bladder endometriosis: conservative management. J Urol. 2000;163(6):1814-1817. [ Links ]
4. Donnez J, Brosens I. Definition of ureteral endometriosis? Fertil Steril. 1997;68(1):178-180. [ Links ]
5. Maccagnano C, Pellucchi F, Rocchini L, Ghezzi M, Scattoni V, Montorsi F, et al. Ureteral endometriosis: proposal for a diagnostic and therapeutic algorithm with a review of the literature. Urol Int. 2013;91(1):1-9. [ Links ]
6. Chapron C, Chiodo I, Leconte M, Amsellem-Ouazana D, Chopin N, Borghese B, et al. Severe ureteral endometriosis: the intrinsic type is not so rare after complete surgical exeresis of deep endometriotic lesions. Fertil Steril. 2010;93(7):2115-2120. [ Links ]
7. Kumar S, Tiwari P, Sharma P, Goel A, Singh JP, Vijay MK, et al. Urinary tract endometriosis: review of 19 cases. Urol Ann. 2012;4(1):6-12. [ Links ]
8. Khwaja A. KDIGO clinical practice guidelines for acute kidney injury. Nephron ClinPractice. 2012;120(4):c179-184. [ Links ]
9. Watanabe Y, Ozawa H, Uematsu K, Kawasaki K, Nishi H, Kobashi Y. Hydronephrosis due to ureteral endometriosis treated by transperitoneal laparoscopic ureterolysis. Int J Urol. 2004;11(7):560-562. [ Links ]
10. Umar SA, MacLennan GT, Cheng L. Endometriosis of the ureter. J Urol. 2008;179(6):2412. [ Links ]
11. Yohannes P. Ureteral endometriosis. J Urol. 2003;170(1):20-25. [ Links ]
12. Papakonstantinou E, Orfanos F, Mariolis-Sapsakos T, Vlahodimitropoulos D, Kondi-Pafiti A. A rare case of intrinsic ureteral endometriosis causing hydronephrosis in a 40-year-old woman. A case report and literature review. Clin Exp Obstet Gynaecol. 2012;39(2):265-268. [ Links ]
Maria Inês Correia
Serviço de Medicina Interna do Hospital Central do Funchal
Hospital dos Marmeleiros, Estrada dos Marmeleiros
9050-495 Funchal
E-mail: mariaines.dpc@gmail.com
Disclosure of potential conflicts of interest: none declared
Received for publication: Sep 26, 2016
Accepted in revised form: Jan 30, 2017














